CXR Basics & Views - X-Ray Vision 101
- Standard Views:
- Posteroanterior (PA): Gold standard; minimal cardiac magnification.
- Lateral: Localizes lesions, assesses retrosternal/retrocardiac spaces.
- Other Views:
- Anteroposterior (AP): Portable, sick patients; heart magnified.
- Lateral Decubitus: Detects small pleural effusions.
- Apical Lordotic: Visualizes lung apices (e.g., for TB).
- Quality (📌 RIPE):
- Rotation: Clavicular heads equidistant to spinous process.
- Inspiration: 5-7 anterior / 8-10 posterior ribs visible.
- Penetration: Vertebrae visible behind heart.
- Exposure: Lung markings clear.

- Interpretation (ABCDE): Airway, Bones & soft tissues, Cardiac silhouette, Diaphragm, Effusions/Everything else/Fields.
⭐ PA view is preferred over AP view for routine chest radiography due to less cardiac magnification and better lung field clarity.
Lung Fields & Pleura - Breath of Fresh Air
- Lung Fields (Zones):
- Assess symmetry, translucency.
- Zones: Upper, Middle, Lower (not lobes on PA).
- Markings: Vascular, taper peripherally. Absent in pneumothorax.
- Hila: Left usually higher (~1-2.5 cm) than right. 📌 LASH: Left Aortic Arch, Sits Higher.
- Contents: Vessels, bronchi, nodes.
- Hilum overlay sign: Differentiates anterior mediastinal vs. hilar mass.
- Pleura:
- Normally invisible. Visible if thickened, fluid/air.
- Visceral (lung), Parietal (chest wall).
- Fissures:
- Major (oblique): Separates lower from upper/middle lobes.
- Minor (horizontal): Right side only (RUL/RML). Seen in ~60% PA CXRs.
- Costophrenic angles: Sharp. Blunting = effusion (~175-200 mL PA).
- Apices: Check for masses (Pancoast).
⭐ The right minor fissure is typically at the 4th anterior rib/interspace.
 oka
oka
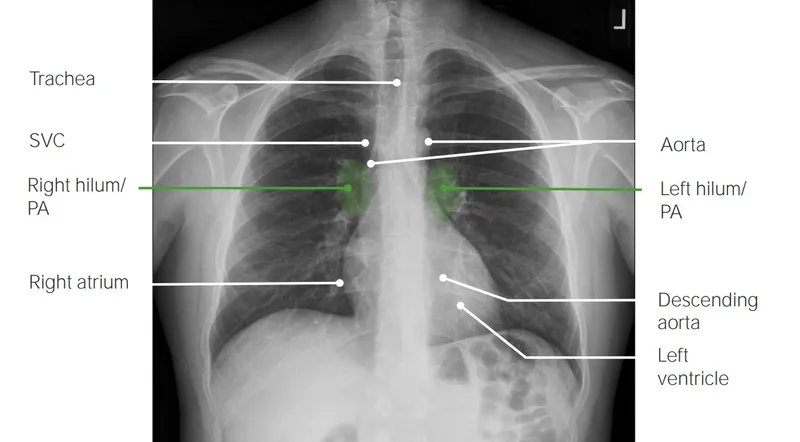
Mediastinum & Heart - Central Command
- Mediastinal Divisions:
- Anterior: Sternum to pericardium. Thymus, nodes.
- Middle: Heart, great vessels (ascending aorta, PA), trachea, hila.
- Posterior: Pericardium to vertebrae. Descending aorta, esophagus.
- Cardiac Silhouette:
- Cardiothoracic Ratio (CTR): < 0.5 (PA view).
- PA Borders:
- Right: SVC, RA.
- Left: Aortic Knob, MPA, LAA, LV.
- Lateral Borders:
- Anterior: RV.
- Posterior: LA, LV.
- Hila:
- Left hilum typically higher (≤ 2.5 cm) than right.
- Contents: Pulmonary vessels, bronchi, nodes.
- Key Lines/Windows:
- Right Paratracheal Stripe: < 4 mm.
- Aortopulmonary (AP) Window: Concave; aortic arch to left PA.
⭐ CTR < 0.5 is key for normal heart size on PA CXR; consider patient factors.
 oka
oka
Diaphragm, Bones & Soft Tissues - The Supporting Cast
- Diaphragm:
- Dome-shaped; right hemidiaphragm usually 1-2.5 cm higher than left (due to liver).
- Costophrenic (CP) angles: Sharp, acute. Blunting suggests effusion.
⭐ On an erect PA chest X-ray, lateral CP angle blunting typically indicates ~175-200 ml of pleural fluid. Posterior CP angle (seen on lateral view) is most sensitive, showing blunting with ~75 ml.
- Cardiophrenic angles: Medial, between heart and diaphragm.
- Bones:
- Ribs: Posterior aspects more horizontal. Adequate inspiration: 9-10 posterior ribs visible. Check for integrity.
- Clavicles, Scapulae, Sternum, Vertebrae: Assess for alignment, fractures, lesions.
- Soft Tissues:
- Examine chest wall, axillae, supraclavicular areas.
- Identify breast shadows, nipple shadows (potential nodule mimics).
- Note symmetry, swelling, calcifications, subcutaneous emphysema.
High‑Yield Points - ⚡ Biggest Takeaways
- PA view is standard; AP view causes cardiac magnification.
- Trachea is midline; carina lies at T4-T5 vertebral level.
- Left hilum is usually slightly higher than the right hilum.
- Normal Cardiothoracic Ratio (CTR) is < 0.5 on PA films.
- Costophrenic angles must be acutely angled and clear.
- Right hemidiaphragm is typically superior to the left.
- Always check for aortic knob and gastric air bubble under the left hemidiaphragm_._
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

