ILD Overview & HRCT Patterns - Lungs in Distress
-
Interstitial Lung Disease (ILD): Heterogeneous group of disorders affecting lung interstitium, often leading to inflammation & fibrosis.
-
Broad Classification:
- Known causes: Drugs (Amiodarone, Bleomycin), Connective Tissue Diseases (CTD - RA, SSc), Environmental (Silicosis, Asbestosis).
- Idiopathic Interstitial Pneumonias (IIPs): e.g., Usual Interstitial Pneumonia (UIP), Non-Specific Interstitial Pneumonia (NSIP).
- Granulomatous: Sarcoidosis, Hypersensitivity Pneumonitis (HP).
- Rare ILDs: e.g., Lymphangioleiomyomatosis (LAM), Pulmonary Langerhans Cell Histiocytosis (PLCH).
-
Key HRCT Patterns:
- Ground-Glass Opacity (GGO): Hazy ↑ lung density, vessels visible.
- Reticular pattern: Network of fine lines.
- Honeycombing: Clustered, stacked subpleural cysts (typically 3-10 mm diameter, <3 mm walls); key for UIP.
- Nodules (distribution): Perilymphatic (Sarcoidosis, Silicosis), Centrilobular (HP, RB-ILD), Random (Miliary TB, fungal).
- Traction bronchiectasis/bronchiolectasis: Irreversible airway dilatation due to adjacent fibrosis.
- Consolidation; Cysts.
-
Distribution Patterns:
- Apical: Silicosis, Sarcoidosis (chronic), PLCH, Ankylosing Spondylitis.
- Basal & Peripheral: UIP/IPF, Asbestosis, most CTD-ILDs.
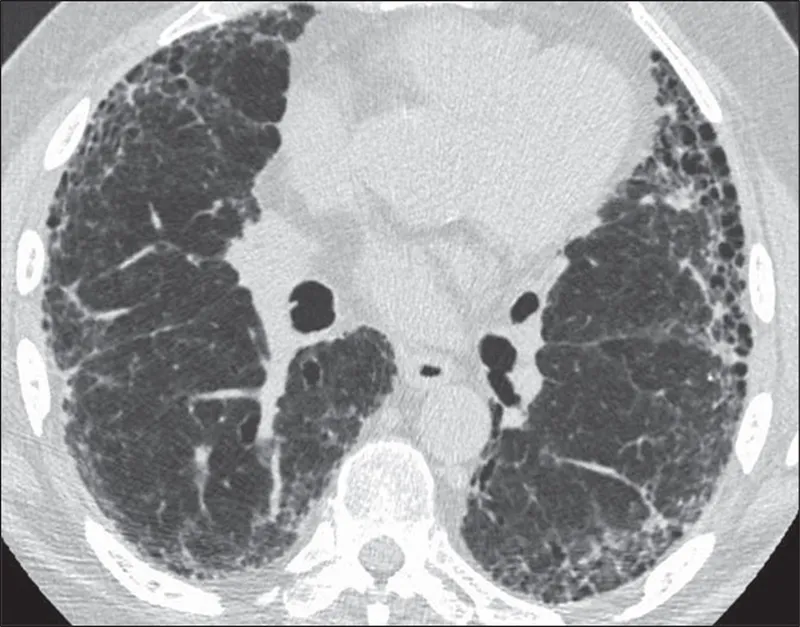
⭐ Honeycombing on HRCT is a hallmark of the Usual Interstitial Pneumonia (UIP) pattern, indicating irreversible fibrosis and generally associated with a poorer prognosis compared to other IIPs without honeycombing.
IIPs - The Usual Suspects
-
Idiopathic Pulmonary Fibrosis (IPF) / Usual Interstitial Pneumonia (UIP): Most common IIP, progressive, poor prognosis.
- UIP Pattern (HRCT): Basal, subpleural, reticular pattern; honeycombing is hallmark. +/- traction bronchiectasis. Absence of features suggesting alternative diagnoses.
- See flowchart for diagnostic categories (Definite, Probable, Indeterminate, Alternative Dx).
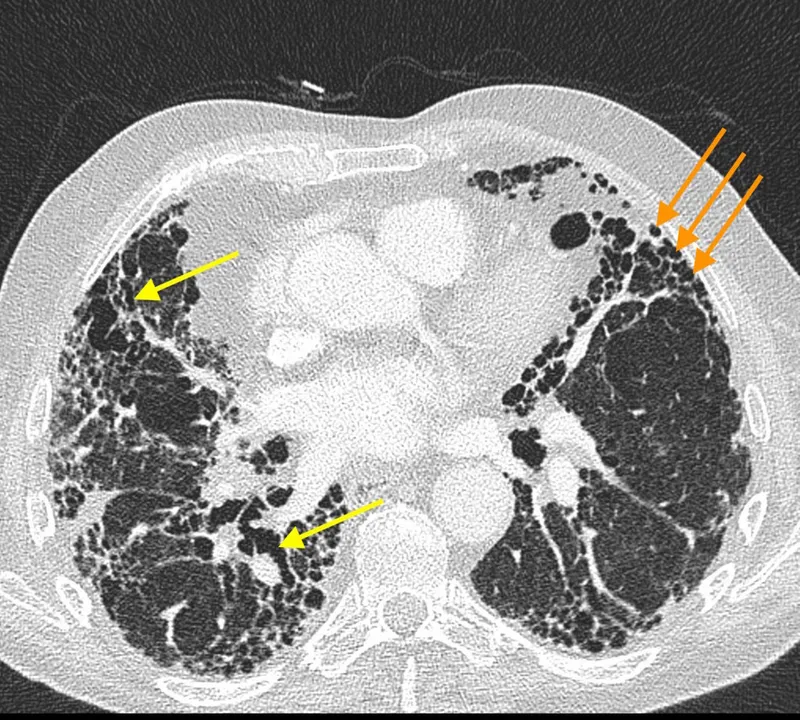
-
Nonspecific Interstitial Pneumonia (NSIP): Better prognosis than IPF.
- HRCT: Ground-glass opacities (GGO), reticulation, traction bronchiectasis. Typically basal predominant; subpleural sparing can occur.
- Cellular (more GGO, better response) vs. Fibrotic.
-
UIP vs. NSIP Key Differences:
Feature UIP (IPF) NSIP Distribution Basal, subpleural Basal (subpleural sparing possible) GGO Minimal/Absent Often Prominent (esp. cellular) Honeycombing Common, Hallmark Rare/Absent Prognosis Poor Better
⭐ Honeycombing on HRCT is the most specific finding for a UIP pattern.
- Other Major IIPs: Cryptogenic Organizing Pneumonia (COP), Respiratory Bronchiolitis-ILD (RB-ILD), Desquamative Interstitial Pneumonia (DIP), Lymphocytic Interstitial Pneumonia (LIP), Acute Interstitial Pneumonia (AIP). 📌 Can Really Do Lung Assessment.
Sarcoid & HP - Granuloma Spotlight
-
Sarcoidosis: Multisystem granuloma; common thoracic involvement.
- HRCT:
- Perilymphatic nodules (along bronchovascular bundles, interlobular septa, subpleural regions).
- Bilateral, symmetrical hilar/mediastinal lymphadenopathy (LAPs).
- Fibrosis in later stages (upper/mid zone predominant).
- Scadding Stages: 0 (Normal CXR) to IV (Pulmonary fibrosis).
- 📌 Mnemonic: "1-2-3 sign" (Right paratracheal + bilateral hilar LAPs); perilymphatic "beading".
- HRCT:
-
Hypersensitivity Pneumonitis (HP): Immune response to inhaled antigens.
- HRCT:
- Acute/Subacute: Centrilobular GGO nodules, mosaic attenuation (air trapping on expiration).
- Chronic: Fibrosis (often mid/upper zone or diffuse), honeycombing (can mimic UIP but distribution differs), significant air trapping.
- HRCT:
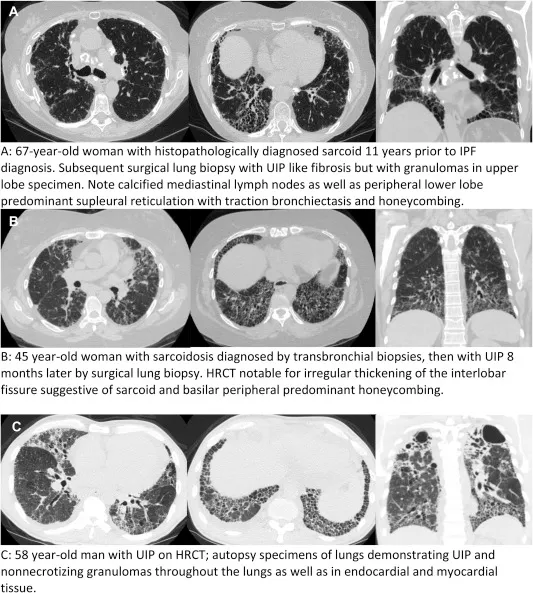
⭐ "Three-density pattern" ("headcheese sign": normal lung, GGO, air trapping) on HRCT strongly suggests subacute HP.
Pneumoconioses & CTD‑ILDs - Occupational & Systemic
- Pneumoconioses: ILDs from inhaled inorganic dusts.
- Silicosis: Upper lobe nodules, hilar eggshell calcification. Risk of Progressive Massive Fibrosis (PMF).
- CWP: Similar to silicosis; simple vs. complicated (PMF).
- Asbestosis: Lower lobe fibrosis, pleural plaques (parietal, diaphragmatic), benign effusions.
- CTD-ILD: Systemic autoimmune disease-associated ILD.
- Patterns:
CTD Common ILD Pattern(s) Scleroderma NSIP (most common) Myositis NSIP, OP RA UIP (most common) Sjögren's LIP, NSIP
⭐ Asbestosis: only pneumoconiosis significantly ↑ mesothelioma risk, esp. in smokers.
- Patterns:
High‑Yield Points - ⚡ Biggest Takeaways
- UIP/IPF: Characterized by basal, subpleural honeycombing.
- NSIP: Shows ground-glass opacities with subpleural sparing; linked to CTDs.
- Sarcoidosis: Presents with bilateral hilar lymphadenopathy and upper lobe predominant reticulonodular patterns.
- Silicosis/CWP: Features upper lobe nodules and eggshell calcification of hilar nodes.
- HP: Key findings include centrilobular nodules, air trapping, and the headcheese sign.
- LCH: Upper lobe cysts and nodules in smokers, typically spares costophrenic angles.
- LAM: Diffuse thin-walled cysts in women of childbearing age; associated with tuberous sclerosis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

