Initial Scan & Scope - Trauma Triage Tools
- Primary Survey (ABCDE): Crucial first step. Imaging aids 'B' (Breathing - pneumothorax) & 'C' (Circulation - hemothorax, tamponade).
- eFAST (Extended FAST): Bedside ultrasound for immediate life-threats: pneumothorax, hemothorax, pericardial effusion.
- 📌 Key Chest Views: Bilateral anterior & lateral thoracic scans (parasternal, midclavicular, axillary lines).
- Findings:
- Pneumothorax: Absent lung sliding ("barcode sign" on M-mode); lung point (pathognomonic, confirms PTX).
- Hemothorax: Anechoic/hypoechoic fluid in pleural space.
⭐ eFAST has a high specificity but moderate sensitivity for detecting pneumothorax and hemothorax in trauma patients.
- Chest X-Ray (CXR - AP Supine): Initial, widely available.
- Limitations: Supine position hinders detection (small pneumothorax, layering effusions), magnification.
- Key Findings: Pneumothorax, hemothorax, widened mediastinum (aortic injury soft sign: >8cm), fractures, contusions.

- MDCT Chest: Gold standard for definitive diagnosis of complex injuries.
- Indications: High-energy trauma, abnormal/equivocal CXR/eFAST, suspected vascular (CTA), tracheobronchial, diaphragmatic injury.
- Protocols: Whole-body CT (WBCT) for polytrauma; CTA for arterial injury.
Ribs, Air & Blood - Walls & Linings
-
Rib Fractures: Most common chest trauma.
- Complications: Pulmonary contusion, neurovascular/visceral injury.
- Associated injuries by location:
Ribs Associated Injury Potential 1-3 Major vascular (subclavian), brachial plexus, lung 4-8 Lung (pneumothorax, contusion) 9-12 Liver, spleen, kidneys (solid abdominal organs)
⭐ First and second rib fractures are markers of severe trauma and have a high association with vascular and brachial plexus injuries.
-
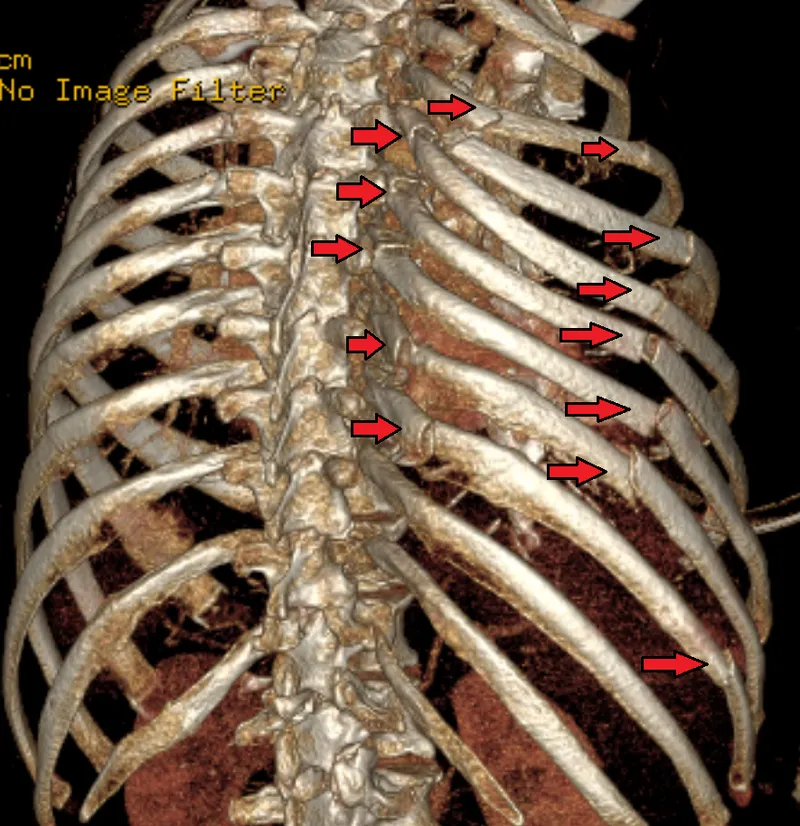
Flail Chest:
- Definition: ≥3 consecutive ribs fractured in ≥2 places.
- Key sign: Paradoxical chest wall movement.
- Often requires mechanical ventilation.
-
Sternal Fractures:
- High-energy trauma; suspect cardiac/aortic injury (ECG, enzymes, CT aortogram).
-
Scapular Fractures:
- Marker of significant trauma force; associated injuries common.
-
Pneumothorax (Air in Pleural Space):
- Simple: Air, no mediastinal shift.
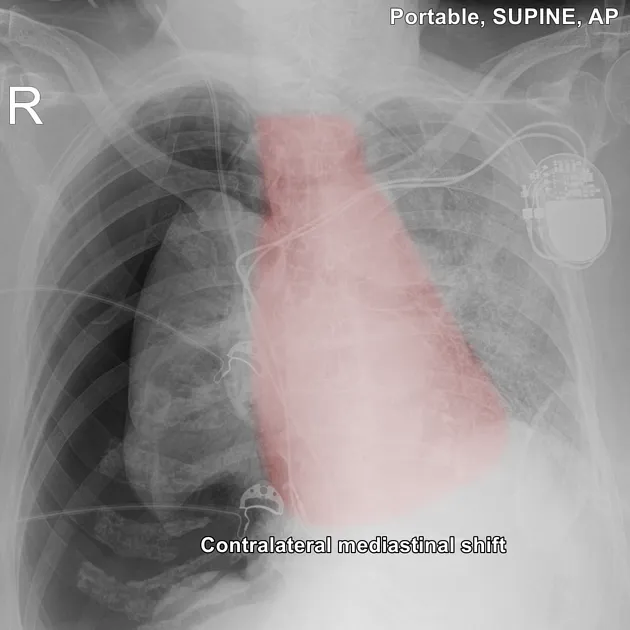
- Tension: Medical emergency!
- Signs: Hypotension, JVD, tracheal deviation (away), ↓air entry.
- Imaging: CXR (visceral line, deep sulcus), CT (most sensitive).
- Needle Decompression: 2nd ICS MCL or 5th ICS AAL/MAL.
- Occult: Seen on CT, not CXR.
-
Hemothorax (Blood in Pleural Space):
- Imaging: CXR (meniscus, opacification), CT.
- Massive Hemothorax:
-
1500ml initial drainage.
- OR >200ml/hr for 2-4 hours.
- Requires urgent thoracotomy.
-
Lungs, Airways & Great Vessels - Deep Impact Damage
- Pulmonary Contusion: Most common. Lung "bruising"; opacities on CXR/CT (ground-glass, consolidation). Appears <6 hrs, resolves 3-7 days.
- Pulmonary Laceration/Hematoma: Parenchymal tear. CT: air/fluid-filled cavities, hematoma.
- Tracheobronchial Injury (TBI): Rare, high mortality. Persistent pneumothorax despite chest tube.
⭐ The 'fallen lung' sign on CXR is highly suggestive of a major tracheobronchial injury.
- Aortic & Great Vessel Injury:
- Mechanisms: Deceleration, penetrating.
- 📌 CT Signs: Direct (Intimal flap, Pseudoaneurysm, Active extravasation, Irregular contour); Indirect (Mediastinal hematoma >1cm, periaortic hematoma).
- Diaphragmatic Rupture: More common on left (~90%). "Collar sign" (constriction of herniated organ). Herniation of abdominal contents.
- Esophageal Injury: Rare. Odynophagia, hematemesis, mediastinal air. Gastrografin swallow or CT with oral contrast.
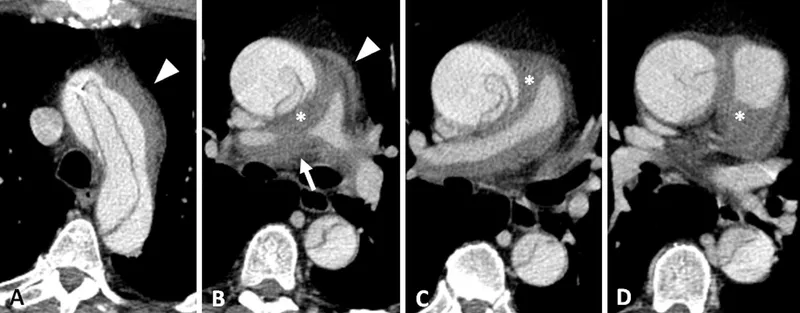
- Cardiac Injury: Blunt Cardiac Injury (BCI) spectrum. Tamponade risk. CT: pericardial effusion, myocardial hematoma.
High‑Yield Points - ⚡ Biggest Takeaways
- CXR is first-line for detecting pneumothorax, hemothorax, and rib fractures.
- CT Chest is the gold standard for detailed evaluation, especially in polytrauma or equivocal CXR.
- Tension pneumothorax: Look for mediastinal shift away from the affected side.
- Aortic injury: Widened mediastinum on CXR is a critical sign; CTA confirms.
- Pulmonary contusion: Patchy opacities appearing ~6 hours post-trauma, typically resolving in 3-7 days.
- Diaphragmatic rupture: More common on the left; suspect with bowel sounds in chest or NG tube coiled in thorax.
- Flail chest: ≥3 consecutive ribs fractured in ≥2 places leading to paradoxical chest wall movement.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

