CABG Imaging - Grafting Goods
- Graft Types:
- Arterial: LIMA (to LAD = workhorse), RIMA.
- Venous: SVG (Saphenous Vein Graft).
- Radial Artery.
- CTA (Coronary CT Angiography):
- Primary non-invasive tool.
- Assesses: Patency, stenosis (>50% significant), occlusion, aneurysm.
- Optimal timing: 1-6 months post-op (baseline), then as needed.
- DSA (Digital Subtraction Angiography):
- Gold standard for diagnosis/intervention.
- Use if CTA inconclusive or intervention planned.
- Key CTA Checks:
- Graft origin, course, anastomosis, run-off.
- Competitive flow from native vessels.
- Stenosis: Proximal/distal anastomosis, body.
⭐ Patency: LIMA to LAD > Radial Artery > SVG. LIMA to LAD is gold standard graft. 📌 Mnemonic: LIMA Lasts, SVG Sags (Saphenous Vein Grafts sag/stenose earlier).
Prosthetic Valve Imaging - Valve Vibes
- Valve Types:
- Mechanical: Durable (e.g., bileaflet). Lifelong anticoagulation.
- Bioprosthetic (Tissue): Porcine, bovine. Risk of Structural Valve Deterioration (SVD).
- Key Imaging:
- Echocardiography (TTE/TEE): Initial & follow-up. Assesses gradients, regurgitation.
- CT Angiography (CTA): Anatomy, Paravalvular Leak (PVL), thrombus, pannus.
- Fluoroscopy: Mechanical valve leaflet motion.
- Complications (📌 Mnemonic: "VALVES"):
- Valve thrombosis/pannus
- Abscess (Endocarditis)
- Leak (Paravalvular)
- Vegetations (Endocarditis)
- Embolism
- Structural failure/Dehiscence
- Thrombus vs. Pannus (CT):
Feature Thrombus Pannus Attenuation Low (<90 HU) Higher (soft tissue) Onset Acute/Subacute Chronic
⭐ Cine fluoroscopy is excellent for assessing mechanical valve disc mobility; Cine MRI is a radiation-free alternative.
Aortic Repair Imaging - Aorta Alerts

- Primary Goal: Detect complications post EVAR/TEVAR (Endovascular/Thoracic Endovascular Aortic Repair).
- Key Complications:
- Endoleaks (most common, see flowchart)
- Graft infection, migration, kinking
- Pseudoaneurysm at anastomoses
- Graft limb stenosis/occlusion
- Aortoenteric fistula (rare, catastrophic)
- Imaging: CTA is gold standard. Monitor aneurysm sac diameter: stability or shrinkage indicates success. Sac expansion >5mm is concerning for endoleak or endotension.
- Surveillance: Lifelong imaging (CTA/MRA/US) crucial. Typically at 1, 6, 12 months, then annually if stable.
⭐ Type II endoleak is the most common type following EVAR, often from lumbar arteries or IMA. Many are managed conservatively if aneurysm sac is stable/shrinking.
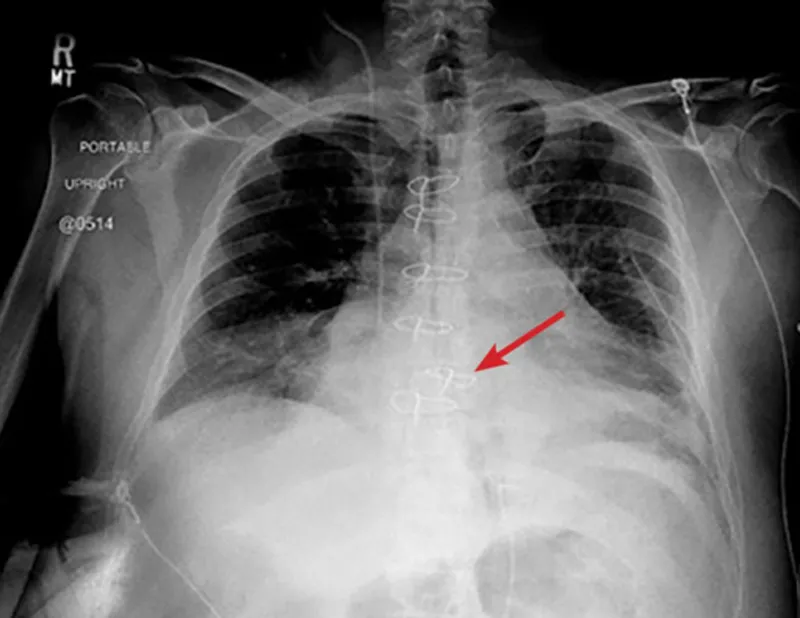
Post-Op Complications - Sternal Scares & More
- Sternal Dehiscence & Instability:
- Clinical: Sternal pain, clicking, palpable gap, instability.
- CXR: Wire fracture/migration, sternal separation > 2-3 mm.
- CT: Defines extent, associated collections, early osteomyelitis.
- Sternal Wound Infection & Mediastinitis:
- Spectrum: Superficial cellulitis to deep mediastinitis.
- Mediastinitis: Fever, sepsis, chest pain, purulent discharge.
- Risk factors: Diabetes, obesity, smoking, prolonged bypass.
- CT (gold standard):
- Retrosternal fluid collections, abscess formation.
- Peristernal soft tissue stranding, edema, enhancement.
- Gas bubbles, air-fluid levels (ominous).
- Sternal osteomyelitis (erosion, sequestrum, involucrum).
⭐ CT signs of mediastinitis include retrosternal fluid collections, soft tissue stranding, and gas bubbles.
- Other common issues: Post-op hematoma, seroma, hypertrophic scarring, keloid formation.
High‑Yield Points - ⚡ Biggest Takeaways
- CABG: CTA for graft patency, sternal dehiscence, and mediastinitis.
- Prosthetic Valves: Echo (TTE/TEE) for leaks, thrombus, vegetations; CT for pannus/structure.
- Aortic Grafts (EVAR/TEVAR): CTA is crucial for endoleaks, infection, and pseudoaneurysms.
- Device Leads: CXR for position/fracture; CT/Echo for perforation, thrombosis.
- LVADs: Echo/CT for pump thrombosis, outflow graft issues, and device infection.
- Sternal Complications: CT is best for early detection of dehiscence or mediastinitis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

