IHD Imaging Overview - Heart Under Scrutiny
Ischemic Heart Disease (IHD) arises from an imbalance between myocardial oxygen supply and demand, primarily due to coronary artery disease (CAD). Its clinical spectrum ranges from stable angina to Acute Coronary Syndromes (ACS) like Unstable Angina, NSTEMI, and STEMI. Imaging is crucial for diagnosis, risk stratification, and guiding therapy.
-
Core Imaging Objectives in IHD:
- Detecting and characterizing CAD.
- Assessing myocardial ischemia and viability.
- Evaluating left ventricular (LV) function and identifying complications.
- Guiding revascularization decisions.
-
Key Imaging Modalities:
- Echocardiography (ECHO): Initial assessment of LV function, regional wall motion abnormalities (RWMA). Stress ECHO for inducible ischemia.
- Myocardial Perfusion Imaging (MPI - SPECT/PET): Detects ischemia, assesses myocardial viability.
- CT Coronary Angiography (CTCA): Non-invasive anatomical evaluation of coronary arteries; high negative predictive value for CAD.
- Cardiac MRI (CMR): Gold standard for LV/RV volumes, function, mass. Assesses edema, infarction (LGE), ischemia, and viability.
⭐ Late Gadolinium Enhancement (LGE) on Cardiac MRI is the reference standard for assessing myocardial scar and viability, critical for predicting recovery post-revascularization in IHD patients.
Coronary CT (CCTA/CAC) - Plaque Patrol
Error: Failed to generate content for this concept group.
MPI & Cardiac MRI - Hot Spots & Heart Scars
- Myocardial Perfusion Imaging (MPI - SPECT/PET): Assesses myocardial perfusion & viability.
- Tracer uptake = viable, perfused tissue. Defects = ↓flow/viability.
- Tracers: $^{99m}$Tc-Sestamibi/Tetrofosmin (SPECT); $^{82}$Rb, $^{13}$N-Ammonia (PET perfusion); $^{18}$F-FDG (PET viability).
- Key Patterns:
- Ischemia: Reversible defect (stress defect, rest normal).
- Infarct: Fixed defect (stress & rest).
- Hibernating: ↓Perfusion, preserved/↑FDG (mismatch).
- Cardiac MRI (CMR): Gold standard for function, mass, viability.
- LGE (Late Gadolinium Enhancement): Identifies "heart scars" (infarcts).
- Ischemic LGE: Subendocardial → transmural.
- Viability (transmurality): <25% (good), >50% (poor recovery).
- MVO (Microvascular Obstruction): Dark core in LGE; poor prognosis.
- T2W: Myocardial edema (acute MI).
- LGE (Late Gadolinium Enhancement): Identifies "heart scars" (infarcts).
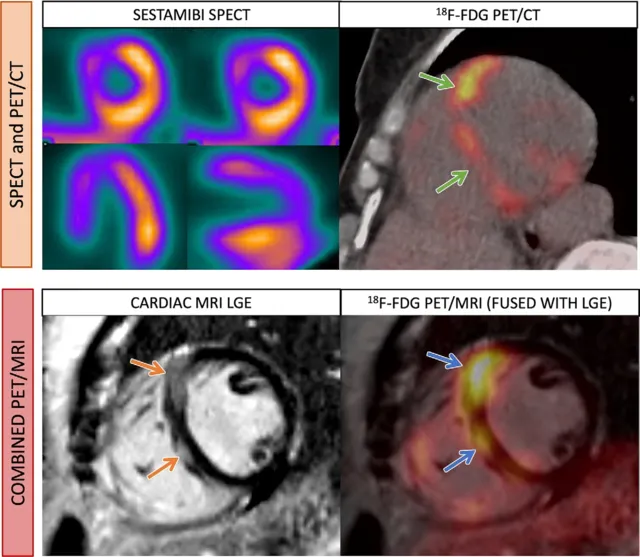
⭐ LGE in CMR: Subendocardial enhancement is the hallmark of ischemic injury; its transmural extent (e.g., >50% thickness) predicts poor functional recovery post-revascularization.
High‑Yield Points - ⚡ Biggest Takeaways
- Stress ECG is initial for stable angina; imaging stress tests (Echo/MPI) for equivocal ECG.
- CCTA excels at ruling out CAD (high NPV), best for low-intermediate risk.
- MPI (SPECT/PET) assesses ischemia & viability; PET offers superior quantification.
- Stress Echo detects inducible wall motion abnormalities, guiding diagnosis/prognosis.
- CMR is gold standard for viability (LGE), infarct sizing, and function.
- Reversible defects on MPI mean ischemia; fixed defects mean infarction.
- Calcium score predicts events; 0 score = excellent prognosis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

