Congenital Heart Disease - Heart's Blueprint
Structural heart abnormalities present from birth. Classified broadly by cyanosis and pulmonary blood flow (PBF).
Radiological Approach:
- CXR: Evaluates heart size, shape, pulmonary vascularity.
- Echocardiography: Primary diagnostic tool for anatomy and function.
- CT/MRI: For complex anatomy, extracardiac connections.
⭐ Tetralogy of Fallot classically presents with a "boot-shaped" heart (coeur en sabot) on CXR due to RV hypertrophy and an upturned apex. This is a common exam question!
Congenital Heart Disease - Pink & Puffy
-
Acyanotic lesions with Left-to-Right (L-R) shunts.
-
Presentation: "Pink" (no cyanosis initially), "Puffy" (signs of congestive heart failure due to ↑ pulmonary blood flow).
-
Radiological Hallmark: Pulmonary plethora (engorged pulmonary vessels).
-
Ventricular Septal Defect (VSD)
- Most common CHD (excluding bicuspid aortic valve).
- X-ray: Cardiomegaly (LV, LA, ±RV enlargement), ↑ pulmonary vascularity.
- Holosystolic murmur.
-
Atrial Septal Defect (ASD)
- X-ray: RA, RV enlargement, prominent main pulmonary artery (MPA), ↑ pulmonary vascularity.
- Wide, fixed splitting of S2.
- Ostium secundum most common type.
-
Patent Ductus Arteriosus (PDA)
- X-ray: Cardiomegaly (LV, LA), prominent MPA, aortic knuckle, ↑ pulmonary vascularity.
- Continuous "machinery" murmur.
- Differential cyanosis if Eisenmenger develops (pink fingers, blue toes).
⭐ Eisenmenger Syndrome: Long-standing L-R shunts (VSD, ASD, PDA) can lead to pulmonary hypertension, shunt reversal (R-L), and cyanosis. Irreversible changes often preclude surgical correction of the primary defect once established. This is a critical complication to recognize early.
- Other causes: Atrioventricular Septal Defect (AVSD).
Congenital Heart Disease - Blue & Booted
- Cyanotic CHDs: Result from Right-to-Left (R→L) shunts.
- 📌 Mnemonic: The 5 T's (Tetralogy of Fallot, Transposition of Great Arteries, Truncus Arteriosus, Total Anomalous Pulmonary Venous Return, Tricuspid Atresia).
- Tetralogy of Fallot (ToF): Most common cyanotic CHD >1 year of age. Classic "boot-shaped" heart.
- 📌 Features (PROVe):
- Pulmonary stenosis (Right Ventricular Outflow Tract Obstruction - RVOTO)
- Right Ventricular Hypertrophy (RVH)
- Overriding aorta
- Ventricular Septal Defect (VSD)
- X-ray: "Boot-shaped" heart (Coeur en sabot); ↓ pulmonary vascularity.

- Clinical: "Tet spells" (hypercyanotic episodes); squatting ↑SVR (Systemic Vascular Resistance), ↓R-L shunt.
- 📌 Features (PROVe):
- Transposition of Great Arteries (TGA): Most common cyanotic CHD in newborns.
- Pathophysiology: Parallel circulation (Aorta from RV, Pulmonary Artery from LV). Survival depends on mixing shunts (e.g., PDA, ASD, VSD).
- X-ray: "Egg-on-string" sign; typically ↑PBF (pulmonary blood flow).
- Truncus Arteriosus: Single arterial trunk supplies all circulations; VSD always present. ↑PBF.
- TAPVR (Total Anomalous Pulmonary Venous Return): All pulmonary veins drain to RA or systemic veins (not LA).
- X-ray: "Snowman" sign / "Figure-of-8" (supracardiac type); ↑PBF.
- Tricuspid Atresia: Absent tricuspid valve, hypoplastic RV. Requires ASD & VSD/PDA for survival. ↓PBF.
⭐ In Tetralogy of Fallot, the clinical severity and degree of cyanosis are primarily determined by the severity of pulmonary stenosis (RVOTO).
Congenital Heart Disease - Bottlenecks & Boxes
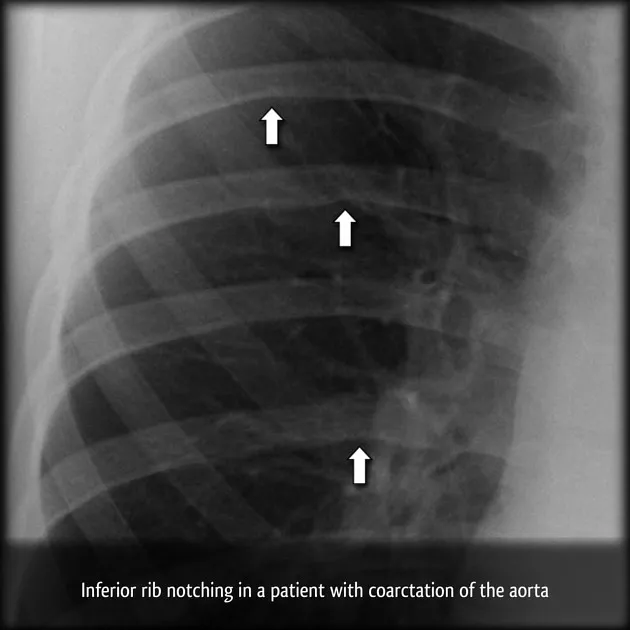
- Coarctation of Aorta (CoA)
- Localized narrowing of aorta, typically juxtaductal.
- Signs: Upper limb HTN, radio-femoral delay.
- CXR: "3" sign (aortic knob, coarctation, post-stenotic dilatation), rib notching (inferior, 3rd-8th ribs).
- CT/MRI Angio: Definitive.
- Ebstein's Anomaly
- Apical displacement of septal & posterior tricuspid valve leaflets.
- Atrialization of RV; small functional RV.
- CXR: Globular or "box-shaped" heart, massive cardiomegaly (RA enlargement).
- 📌 Associated with maternal lithium use.
- Hypoplastic Left Heart Syndrome (HLHS)
- Underdevelopment of LV, aorta, aortic/mitral valves.
- Ductal-dependent systemic circulation.
- Pulmonary Atresia with Intact Ventricular Septum (PA/IVS)
- Complete RVOT obstruction, often hypoplastic RV.
- Ductal-dependent pulmonary circulation.
⭐ In Coarctation of Aorta, the "figure 3" sign on CXR is formed by pre-stenotic dilatation of the aorta/left subclavian artery, the indentation of the coarctation, and post-stenotic dilatation of the descending aorta.
High‑Yield Points - ⚡ Biggest Takeaways
- Tetralogy of Fallot (TOF): Most common cyanotic CHD; CXR shows "boot-shaped" heart.
- Transposition of Great Arteries (TGA): CXR shows "egg-on-string" sign; severe neonatal cyanosis.
- Ventricular Septal Defect (VSD): Most common overall CHD; can lead to pulmonary hypertension.
- Atrial Septal Defect (ASD): Pulmonary plethora and right ventricular enlargement on CXR.
- Coarctation of Aorta: Rib notching (inferior, posterior ribs 3-8); "3" sign on barium/aortogram.
- Patent Ductus Arteriosus (PDA): Continuous "machinery" murmur; risk of Eisenmenger syndrome.
- Ebstein's anomaly: Apical displacement of tricuspid valve; "box-shaped" heart, atrialized RV.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

