Post-Tx Baseline & Goals - New Normal Nav
- Primary Goal: Detect recurrence/new primaries; differentiate from expected post-treatment changes.
- "New Normal" Establishment:
- Treatment alters breast architecture (scars, seromas, fat necrosis).
- Baseline imaging captures these changes for future comparison.
- Baseline Mammography Timing (Post-BCT):
- Typically 6-12 months after completing Radiation Therapy (RT).
⭐ First post-RT mammogram: 6-12 months after RT completion is crucial for establishing a new baseline.
- Earlier if clinically indicated.
- Typically 6-12 months after completing Radiation Therapy (RT).
- Surveillance:
- Annual mammography.
- Ultrasound/MRI for specific indications (e.g., dense breasts, high-risk).
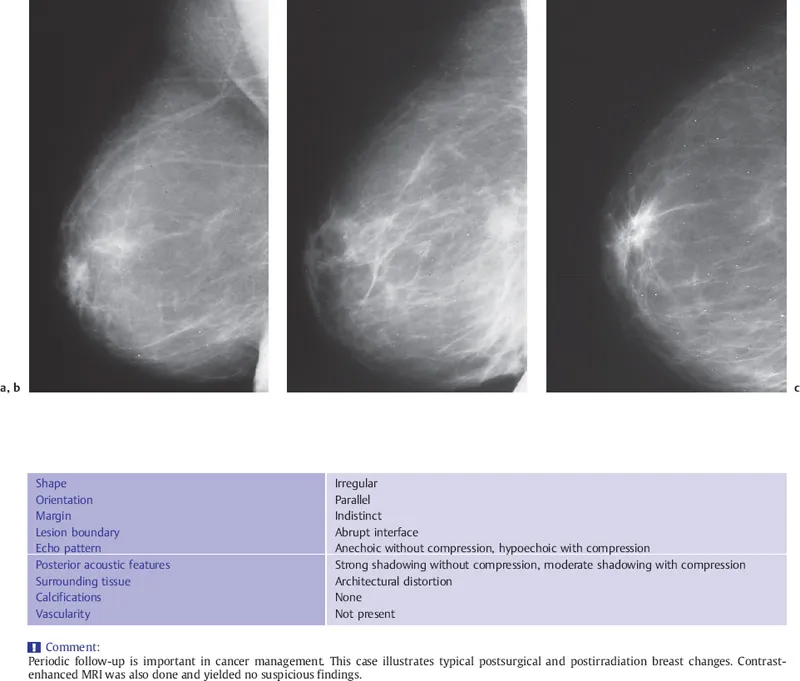
- Challenge: Differentiating benign post-tx changes from recurrence.
Surgical Sequelae - Surgical Souvenirs
- Common Post-Op Changes (All Modalities):
- Early: Seroma (clear fluid), hematoma (blood), edema, skin thickening. Usually resolve.
- Late: Scar/fibrosis (spiculated, stable/shrinking), fat necrosis (oil cysts: lucent mammo, anechoic US; dystrophic calcifications: coarse, rim), architectural distortion.
- Surgical clips: Mark lumpectomy bed.
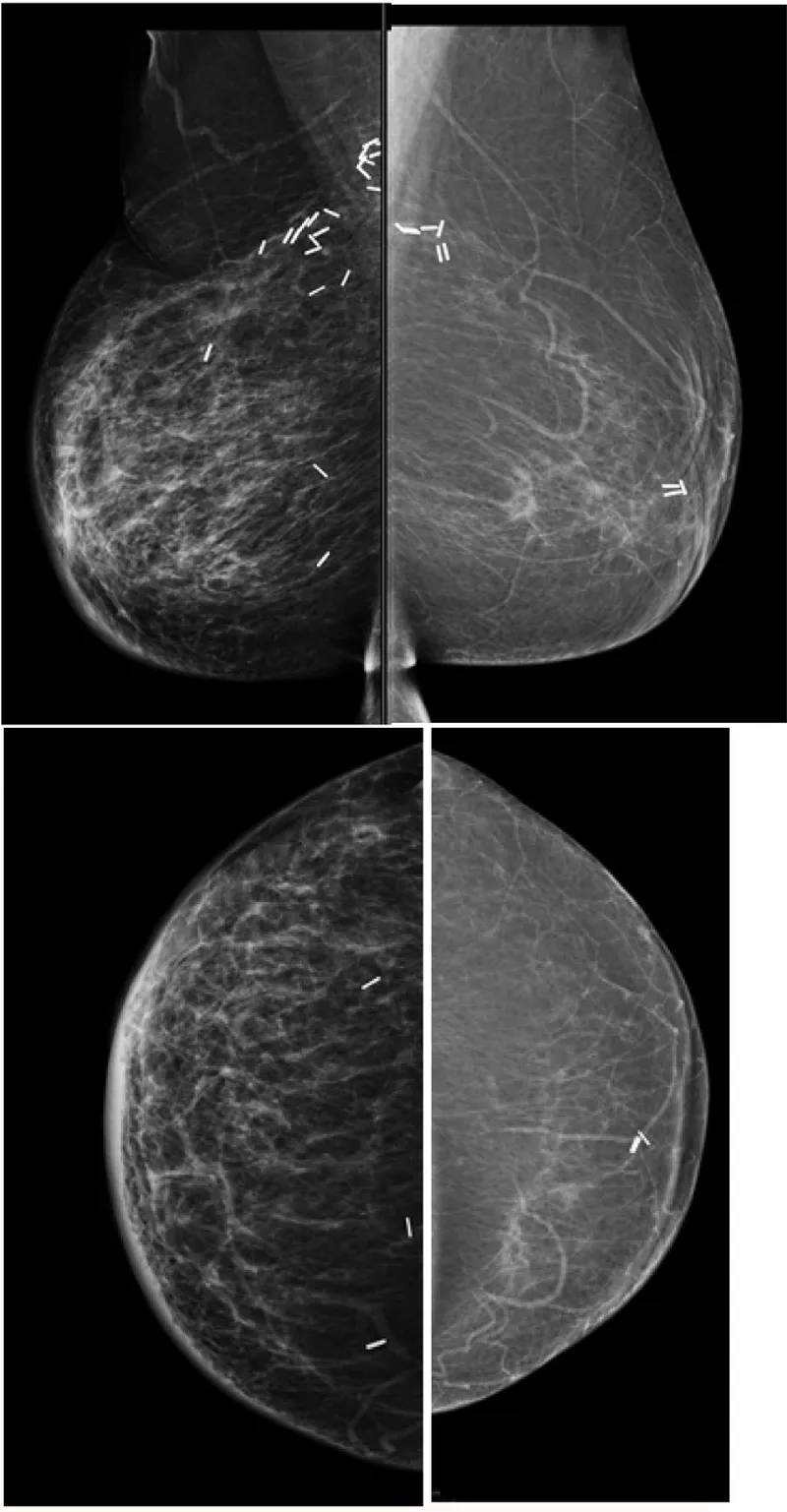
- Lumpectomy Cavity: Evolves from fluid → granulation tissue → scar. Stability is key.
- Mastectomy: Absence of breast tissue; monitor chest wall.
- Reconstruction:
- Implants: Check for rupture (e.g., linguine sign MRI for intracapsular).
- Flaps (TRAM/DIEP): Monitor for fat necrosis, seroma.
⭐ > A post-surgical scar can mimic malignancy (spiculation) but stability or regression on serial imaging is reassuring; growth is a red flag.
Radiation & Systemic Rx - Ray & Rx Remnants
- Radiation Therapy (RT) Changes:
- Acute (0-6 months): Skin thickening, ↑ breast density, edema, ill-defined haziness.
- Developing (6-12 months): Peak skin changes, early fibrosis, architectural distortion may begin.
- Chronic (>12 months): Established fibrosis, scarring, architectural distortion, fat necrosis (oil cysts, dystrophic calcifications), skin retraction, telangiectasias, volume ↓.
- Calcifications: Typically benign, coarse, dystrophic; may appear 1-2 years post-RT.
- ⭐ > Radiation-induced angiosarcoma is a rare but serious late complication, typically presenting 5-10 years post-RT.
- Systemic Therapy Changes:
- Chemotherapy: Generally minimal direct breast imaging changes. May show tumor shrinkage if neoadjuvant. Ovarian suppression can induce menopausal changes (↓ density).
- Hormonal Therapy:
- Tamoxifen: Variable effects; can ↑ breast density in some postmenopausal women. Associated with endometrial changes.
- Aromatase Inhibitors (AIs): Tend to ↓ breast density and promote glandular atrophy.
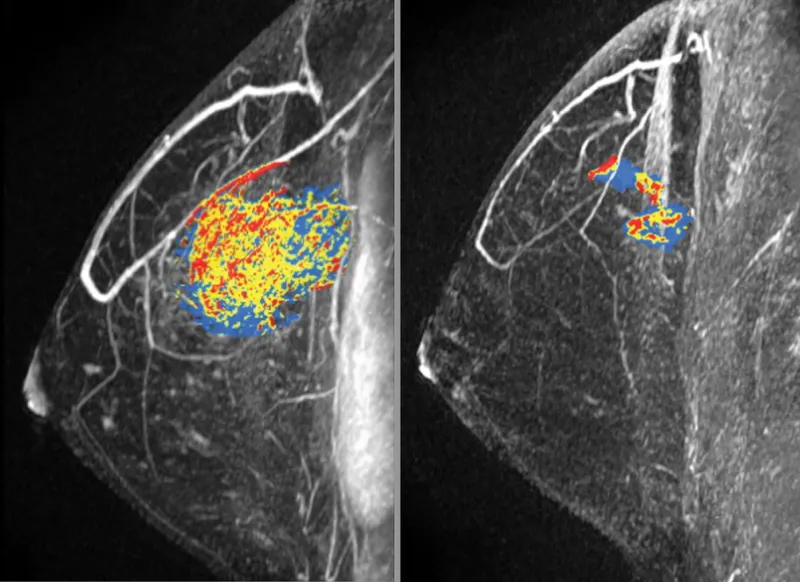
Recurrence Radar - Red Flag Recon
Key: Differentiate recurrence from benign changes.
-
General Red Flags:
- New/growing mass/density.
- New/increasing suspicious microcalcifications.
- Architectural distortion developing >2 years post-op.
-
Modality Specific Signs:
- Mammography:
- New/enlarging opacity at/near surgical site.
- New pleomorphic/linear microcalcifications.
- Ultrasound (US):
- New solid hypoechoic mass (irregular/spiculated).
- Increased vascularity on Doppler.
- MRI:
- New enhancing mass (Type II/III kinetics).
- New non-mass enhancement (NME) (segmental/ductal).
- Mammography:
-
Differentiating Benign Changes:
- Scar: Stable/retracts over time. Initial distortion possible.
- Fat Necrosis: Oil cysts, dystrophic Ca++ (rim/coarse). Predictable evolution.
- Seroma: Simple fluid, resolves/shrinks.
⭐ Architectural distortion at the lumpectomy site developing >2 years post-treatment is highly suspicious for recurrence.
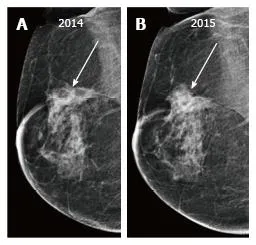
High‑Yield Points - ⚡ Biggest Takeaways
- Baseline mammogram post-treatment (lumpectomy/radiation) is crucial at 6-12 months.
- Differentiating scar (stable/shrinks) from recurrence (grows, new calcifications) is key.
- Fat necrosis is common; look for stability or pathognomonic lucent-centered calcifications.
- MRI has the highest sensitivity for detecting local recurrence, especially in dense breasts.
- Post-mastectomy imaging is typically for palpable concerns or high-risk individuals.
- New or enlarging axillary lymph nodes may indicate axillary recurrence.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

