Mammography Basics - X-ray Vision Unveiled
- Principle: Low-dose X-rays for breast imaging.
- X-ray Tube:
- Low kVp (25-35 kVp) for high soft tissue contrast.
- Targets: Molybdenum (Mo), Rhodium (Rh), Tungsten (W).
- Filters: Mo, Rh, Aluminium (Al).
⭐ Molybdenum (Mo) target/filter combination is optimal for average breast thickness due to its characteristic X-rays (17.5 & 19.6 keV).
- Small focal spot (0.3 mm routine; 0.1 mm magnification) for high resolution.
- Compression: Essential for image quality.
- ↓Thickness, ↓scatter, ↓motion, ↓dose; separates tissues.
- Grids: Anti-scatter; improve contrast.
- AEC: Automatic Exposure Control for consistent image density.
 oka
oka
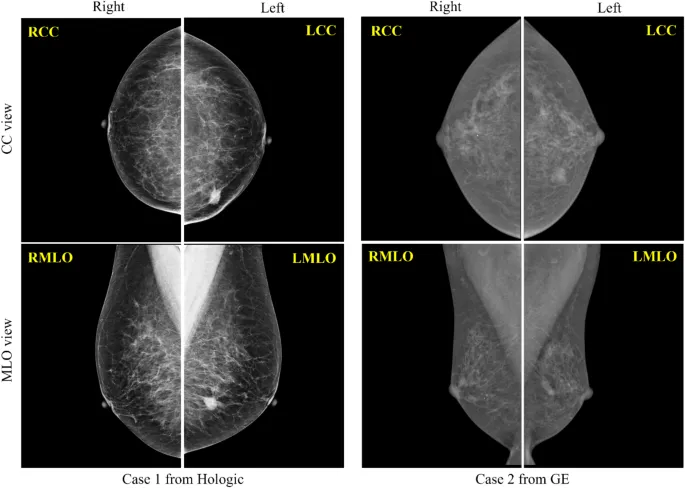
Standard Projections - Two-Angle Truth
- Two views/breast for 3D localization.
- 1. Craniocaudal (CC) View:
- Beam: Superior → Inferior.
- Shows: Medial vs. Lateral position.
- Adequacy: Pectoral muscle (~30%); PNL visualized.
- 2. Mediolateral Oblique (MLO) View:
- Beam: Medial → Lateral, angled 45-60°.
- Shows: Superior vs. Inferior position; most tissue.
⭐ In an adequate MLO view, the pectoral muscle should be visible to the level of the posterior nipple line (PNL) or deeper.
- Adequacy: Inframammary fold (IMF) open.
- "Two-Angle Truth": Differentiates lesions vs. superimposition.
Special Techniques - Problem Solvers Pro
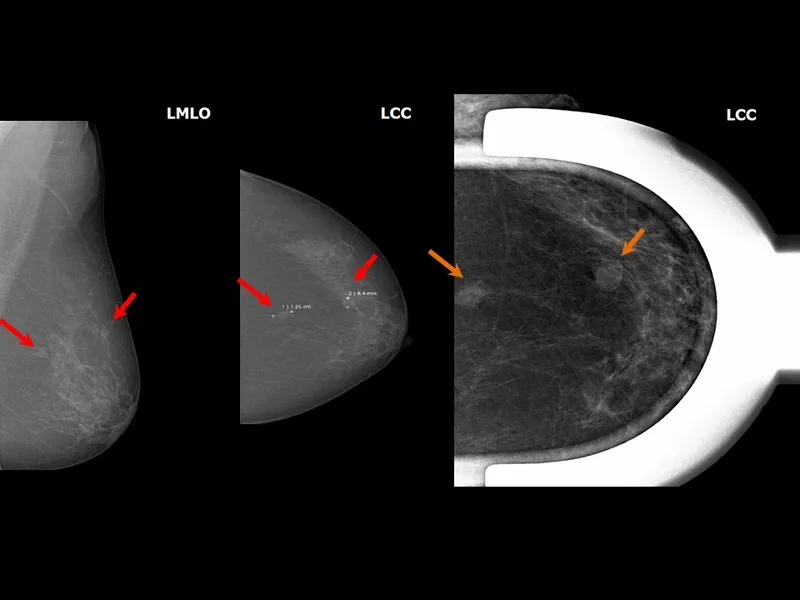
- Magnification Views (M-views):
- Details calcifications & mass margins.
- Small focal spot, air gap. ↑Resolution, ↓scatter.
- Spot Compression:
- Displaces tissue, clarifies margins, checks pliability.
- Focal compression.
- Rolled Views (e.g., RM, RL):
- Localizes lesions, separates tissue.
- Exaggerated Craniocaudal (XCCL, XCCM):
- Visualizes extreme lateral/medial tissue.
- Cleavage View (CV):
- Images deep medial breast.
- Digital Breast Tomosynthesis (DBT):
- 3D mammography; thin slices.
- ↓Overlap, ↑detection, ↓recall.
⭐ Digital Breast Tomosynthesis (DBT) improves lesion detection and characterization by reducing tissue overlap, especially in dense breasts.
- Contrast-Enhanced Mammography (CEM):
- Functional; contrast highlights neovascularity.
- Dual-energy subtraction.
Quality & Safety - Sharp & Shielded
- Image Sharpness (Quality):
- Focal Spot: Small (0.3mm std, 0.1mm mag) for ↑spatial resolution.
- Compression: Key for ↓motion blur, ↓scatter, ↓superimposition, ↓geometric unsharpness, ↓dose, ↑contrast.
- Anti-scatter Grid: ↑contrast (↓scatter); may ↑dose by ~2x.
- kVp: 25-35 kVp; impacts contrast & penetration.
- Target/Filter: Mo/Mo (fatty), Mo/Rh, Rh/Rh, W/Rh (dense/digital).
- Radiation Safety (Shielded):
- ALARA principle (As Low As Reasonably Achievable).
- Average Glandular Dose (AGD):
⭐ Average Glandular Dose (AGD) per view in mammography should ideally be less than 3 mGy with a grid.
- AGD factors: breast thickness/composition, compression, kVp, mAs, grid use.
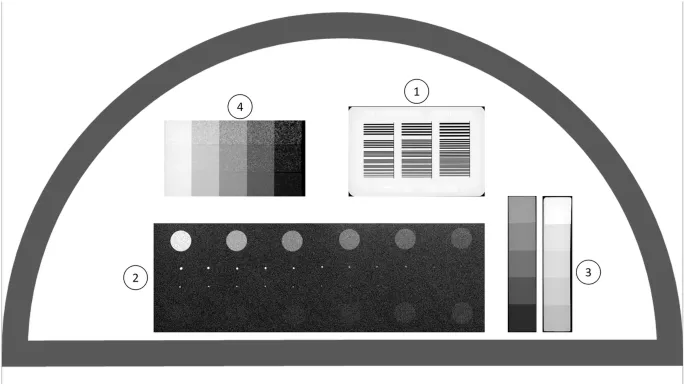
- QC: Regular phantom tests, dose audits. Staff shielding.
High‑Yield Points - ⚡ Biggest Takeaways
- Standard views: Craniocaudal (CC) and Mediolateral Oblique (MLO) form the baseline.
- MLO view: Paramount for visualizing most breast tissue, including axillary tail and pectoral muscle.
- CC view: Best depicts medial and extreme lateral lesions with superior-inferior compression.
- Adequate compression: Crucial for reducing motion blur, radiation dose, and separating overlapping tissues.
- Magnification views: Essential for detailed analysis of microcalcifications and mass characteristics.
- Digital Breast Tomosynthesis (DBT/3D): Significantly improves cancer detection, reduces false positives/recalls.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

