Male Breast Anatomy - More Than Meets the Eye
- Structure: Rudimentary system; primarily ducts & connective tissue.
- Lacks terminal duct lobular units (TDLUs) & acini typically.
- Nipple-areolar complex present.
- Composition: Mainly adipose tissue (fat); minimal glandular tissue.
- Subareolar region: site of most ductal elements.
- Physiology: Ductal system is hormone-sensitive (estrogen/androgen balance).
- No cyclical changes as seen in females.
- Vasculature & Lymphatics: Similar to female breast, but less extensive.
⭐ Normal male mammogram primarily shows radiolucent fat; a small amount of subareolar ductal tissue can be a normal finding, especially in younger or leaner individuals.
Gynecomastia & Benign Buddies - Common Concerns
- Gynecomastia: Benign male breast glandular proliferation; due to ↑estrogen/androgen ratio.
- Etiology:
- Physiological: Neonatal, pubertal, senescent.
- Pathological: Drugs (📌 Spironolactone, Cimetidine, Ketoconazole - "Some Cool Kinds"), liver cirrhosis, testicular tumors (e.g., Leydig, Sertoli), Klinefelter's syndrome.
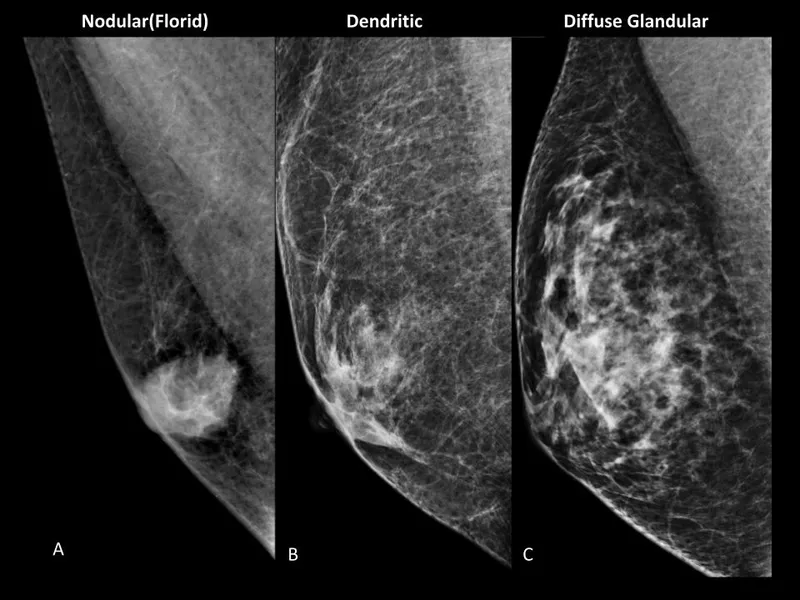
- Mammography Patterns:
- Nodular (florid/acute): Flame-shaped, retroareolar, often tender. Duration <1 year.
- Dendritic (fibrous/chronic): More fibrotic, less tender, branched appearance. Duration >1 year.
- Diffuse Glandular: Resembles female breast tissue; seen with exogenous estrogen.
- USG: Retroareolar hypoechoic glandular tissue; no suspicious features (e.g., spiculation, marked hypoechogenicity, posterior shadowing).
- Etiology:
- Pseudogynecomastia: Fat deposition without glandular tissue; differentiated on USG (fat is hyperechoic compared to gland).
- Lipoma: Common; encapsulated fat; radiolucent (mammo), variable echogenicity, often isoechoic to fat (USG).
- Sebaceous Cyst (Epidermal Inclusion Cyst): Superficial, well-defined, often with a punctum; "claw sign" on mammo; dermal lesion on USG with posterior acoustic enhancement.
- Duct Ectasia: Dilated retroareolar ducts; may present with nipple discharge; often bilateral.
⭐ On mammography, gynecomastia typically presents as a retroareolar density, whereas male breast cancer is often eccentric to the nipple and may have suspicious calcifications or spiculation.
Male Breast Cancer - The Unseen Threat
- Epidemiology:
- Rare, < 1% of all breast cancers.
- Peak incidence: 60-70 years.
- Poorer prognosis (often late diagnosis).
- Risk Factors:
- Genetic: BRCA2 (most common), Klinefelter syndrome.
- Family Hx of breast cancer.
- ↑ Estrogen states: Obesity, liver disease, testicular issues (e.g., cryptorchidism, orchitis).
- Prior chest radiation.
- Advanced age.
- 📌 Mnemonic: BRoCA-K (BRCA, Radiation, Obesity, Cirrhosis, Age, Klinefelter).
- Clinical Presentation:
- Painless, firm, subareolar mass (most common, 75-90%).
- Nipple retraction/discharge (often bloody).
- Skin ulceration/fixation.
- Axillary lymphadenopathy.
- Histopathology:
- Invasive Ductal Carcinoma (IDC) No Special Type (NST) is most common (>85%).
- Lobular carcinoma is rare.
- Most are ER+, PR+, HER2- (Luminal A-like).
- ⭐ > Male breast cancers are more frequently hormone receptor-positive (ER+, PR+) compared to female breast cancers.
- Imaging:
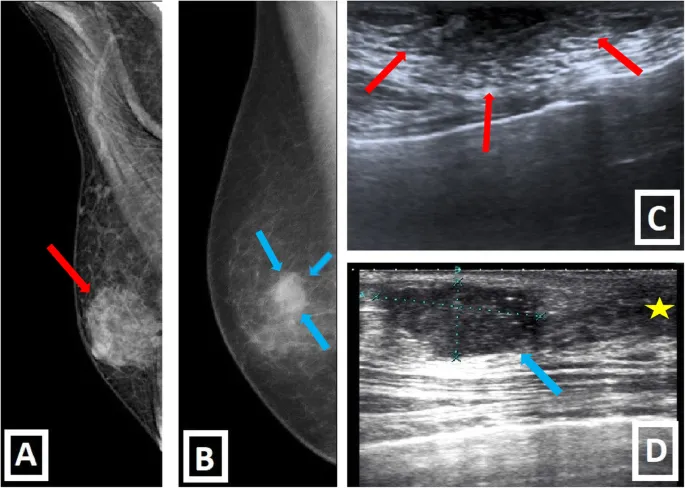
- Mammography: Eccentric, spiculated mass; microcalcifications less common.
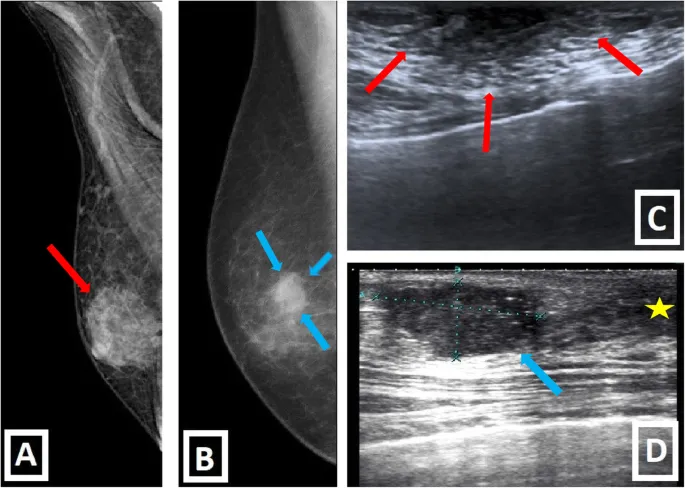
- Ultrasound: Hypoechoic, irregular mass; posterior acoustic shadowing.
- Mammography: Eccentric, spiculated mass; microcalcifications less common.
Imaging Arsenal & Workup - Detecting Danger
- Initial Imaging (Palpable Lump):
- Men <25 yrs / low suspicion: USG.
- Men ≥25 yrs / high suspicion: Mammography (MMG) + USG.
- Mammography (MMG):
- Views: Craniocaudal (CC), Mediolateral Oblique (MLO).
- Malignancy: Spiculated, eccentric mass; suspicious calcs.
- Ultrasound (USG):
- Differentiates cystic vs. solid.
- Malignancy: Irregular, anti-parallel, spiculated, shadowing, vascular.
- Axillary node assessment.
- MRI: Problem-solving, staging; not primary.
- BI-RADS: Standard categories (0-6) used.
⭐ Male breast cancer is rare (<1% of all breast cancers), but often presents at a later stage.
- Biopsy: USG-guided Core Needle Biopsy (CNB) for BI-RADS 4 or 5 lesions.
High‑Yield Points - ⚡ Biggest Takeaways
- Gynecomastia: Most common male breast condition; typically bilateral, symmetrical glandular proliferation.
- Male Breast Cancer: Rare (<1% of all breast cancers), predominantly Invasive Ductal Carcinoma (IDC).
- Key Cancer Risk Factors: BRCA2 mutations, Klinefelter syndrome, family history, ↑estrogen.
- Imaging Modalities: Mammography is primary; ultrasound for problem-solving and biopsy guidance.
- Typical Cancer Appearance: Eccentric, retroareolar, spiculated mass on mammogram; often presents late.
- Pseudogynecomastia: Due to fat deposition (lipomastia), not true glandular tissue; common in obesity.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

