Interventional Breast Procedures - Needle Know-How
- Indications: Primarily for suspicious lesions (BI-RADS 4 & 5), some BI-RADS 3 (patient preference/high risk).
- Patient Preparation:
- Informed consent.
- Discontinue anticoagulants (Aspirin 5-7 days, Warfarin 3-5 days, check INR < 1.5).
- Local anesthesia (Lidocaine 1-2%).
- Contraindications:
- Absolute: Uncooperative patient, lesion inaccessible.
- Relative: Bleeding diathesis, severe thrombocytopenia (< 50,000/μL).
- Needle Types & Guidance:
- Fine Needle Aspiration Cytology (FNAC): 22-25G needle.
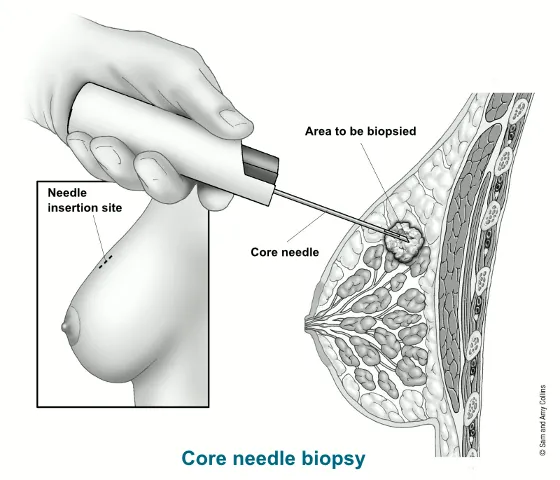
- Core Needle Biopsy (CNB): 14-18G needle; preferred for histology.
- Vacuum-Assisted Biopsy (VAB): 7-14G needle; larger samples.
- Guidance: Ultrasound (most common), Stereotactic (mammography), MRI.
⭐ Key BI-RADS categories mandating biopsy: BI-RADS 4 (Suspicious) and BI-RADS 5 (Highly Suggestive of Malignancy) almost always require tissue diagnosis. BI-RADS 0 requires further imaging, and may lead to biopsy if suspicion arises on further views/modalities. BI-RADS 6 is biopsy-proven malignancy, prior to definitive therapy.
📌 Mnemonic: "Before Procedure, Check Coags" (Bleeding hx, Platelets, INR, Consent, Cease anticoagulants).
Interventional Breast Procedures - Target Acquired
-
Core Principles: Obtain tissue/cells for diagnosis under image guidance.
-
Pre-procedure: Informed consent, check coagulation (INR <1.5, Platelets >50,000), review medications (stop anticoagulants as per guidelines).
-
Biopsy Guidance Algorithm:
-
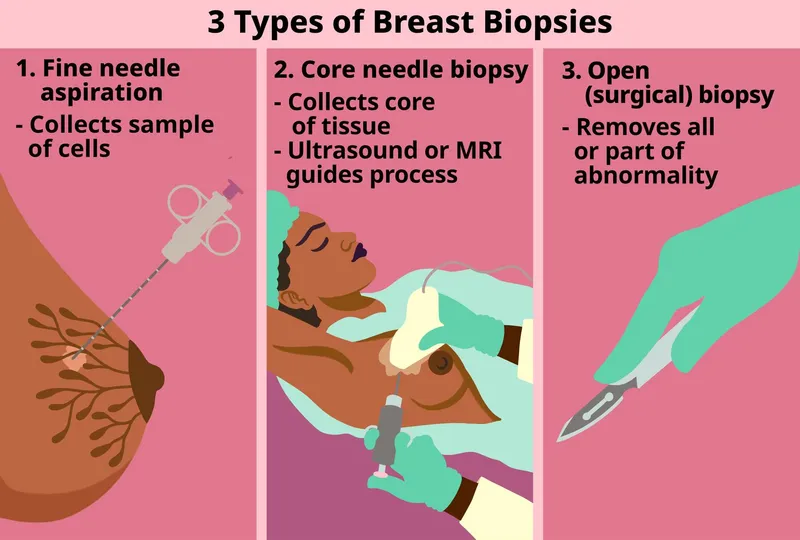
Procedure Types:
- FNAC (Fine Needle Aspiration Cytology):
- Needle: 22-25G.
- Use: Cytology for cystic lesions, suspicious axillary nodes.
- CNB (Core Needle Biopsy):
- Needle: 14G (standard), 16G, 18G.
- Cores: 3-5 (target ~5 for calcifications).
- Provides histology.
- VAB (Vacuum-Assisted Biopsy):
- Needle: 7-11G.
- Use: More tissue, microcalcifications, small lesions.
- FNAC (Fine Needle Aspiration Cytology):
-
Post-procedure: Ensure hemostasis, marker clip placement (common for CNB/VAB, especially if lesion is small or may be removed).
-
Guidance Method Comparison:
Feature Ultrasound (USG) Guidance Stereotactic Guidance (Mammo) Principle Real-time imaging, any patient position X-ray imaging, 2 views for 3D localization Pros Real-time, no radiation, versatile, cheaper Best for calcifications, non-USG visible lesions Cons Operator dependent, some lesions not visible Radiation exposure, compression discomfort, longer procedure Typical Lesions Solid masses, cysts, axillary nodes Microcalcifications, architectural distortions
⭐ Ultrasound is the most common guidance modality for core needle biopsy (CNB) due to its real-time visualization, lack of ionizing radiation, and cost-effectiveness.
Interventional Breast Procedures - Precision Probes
-
Vacuum-Assisted Biopsy (VAB) / Mammotome
- Uses vacuum to pull tissue into the needle before cutting & collecting multiple samples with a single insertion.
- Larger tissue samples than core biopsy; can be image-guided (stereotactic, USG, MRI).
- Therapeutic for complete removal of some benign lesions (e.g., fibroadenomas < 1.5 cm).
-
Pre-operative Localization Techniques: For non-palpable lesions.
| Technique | Pros | Cons | Considerations |
|---|---|---|---|
| Wire Localization (WL) | Widely available, inexpensive | Wire migration/dislodgement, transection; patient discomfort; scheduling conflicts (same-day surgery) | Needs precise placement; difficult for deep lesions or multiple lesions. |
| Radioactive Seed Loc. (RSL) | No external wire, flexible scheduling; better cosmesis, ↓ re-excision rates | Radiation exposure (minimal); requires nuclear medicine expertise & gamma probe; seed migration (rare) | Iodine-125 ($I^{125}$) seed; long half-life allows placement days before surgery. |
| Magnetic Seed Loc. (Magseed) | No radiation, no external wire; flexible scheduling; MRI compatible (some) | Requires specific detector (Sentimag); potential for artifact on MRI; cost | Easier logistics than RSL; good for multiple lesions. |
⭐ VAB is preferred for complete excision of benign lesions or extensive suspicious microcalcifications, offering both diagnostic and therapeutic benefits in a single procedure.
Interventional Breast Procedures - Smooth Recovery
- Specimen Handling:
- Specimen radiograph: Confirms lesion retrieval & marker clip.
- Immediate formalin fixation for pathology.
- Post-Procedure Care:
- Firm pressure (~20 min), then compression dressing.
- Ice packs: Reduce hematoma/pain.
- Analgesia: Paracetamol (avoid aspirin/NSAIDs initially).
- Restrict strenuous activity for 24-48 hrs.
- Keep wound dry for 24 hrs.
- Common Complications:
- Hematoma: Most frequent. Apply prolonged pressure. Large/expanding needs urgent review.
- Pain: Usually mild; paracetamol.
- Infection: Rare. Signs: erythema, warmth, discharge, fever.
- Vasovagal episode: Supportive measures.
⭐ Hematoma is the most common complication following breast core biopsy.
)
High‑Yield Points - ⚡ Biggest Takeaways
- Core needle biopsy (CNB) is gold standard for diagnosing suspicious breast lesions, preferred over FNAC.
- Stereotactic biopsy targets non-palpable mammographic lesions, especially microcalcifications.
- Ultrasound-guided biopsy is for sonographically visible masses, being the most common image-guided technique.
- Wire/Seed localization guides surgical excision of non-palpable lesions.
- Vacuum-assisted biopsy (VAB) yields larger samples and can be therapeutic for benign lesions.
- Most common complication: hematoma; pneumothorax is a rare risk with deep chest wall lesions.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

