Risk Factors & Screening - Early Bird Catches
- Key Risks: ↑Age, BRCA1/2 genes, 1st-degree relative with breast Ca, dense breasts, prior chest RT (Radiation Therapy).
- Hormonal/Lifestyle: Early menarche (<12y), late menopause (>55y), nulliparity, prolonged HRT, obesity, alcohol.
- Screening (Mammography - Average Risk):
- Age 50-74 yrs: Biennial.
- Age 40-49 yrs: Individualized decision; consider annually/biennially.
- High Risk: Earlier screening (e.g., from age 25-30), often + annual MRI.

⭐ Women with BRCA1 mutation have a ~55-72% lifetime risk of breast cancer; BRCA2 mutation carriers have a ~45-69% risk by age 80.
Mammography Magic - X‑ray Vision Quest
- Low-dose X-ray imaging for breast cancer screening & diagnosis.
- Standard Views:
- Craniocaudal (CC): Superior-inferior compression.
- Mediolateral Oblique (MLO): Medial-lateral compression, angled for axillary tail; shows most tissue.

- Key Malignancy Signs:
- Masses: Irregular shape, spiculated margins, high density.
- Calcifications: Pleomorphic, fine linear/branching, clustered/segmental distribution.
- Architectural Distortion: Parenchyma distortion without a visible mass.
- Asymmetry: Focal, developing.
- Digital Breast Tomosynthesis (DBT/3D): Improves cancer detection, reduces recall rates.
- Findings reported using BI-RADS (Breast Imaging Reporting and Data System).
⭐ Spiculated margins of a mass are highly suggestive of malignancy (PPV ~90%).
Ultrasound & MRI - Probing Deeper
- Ultrasound (USG):
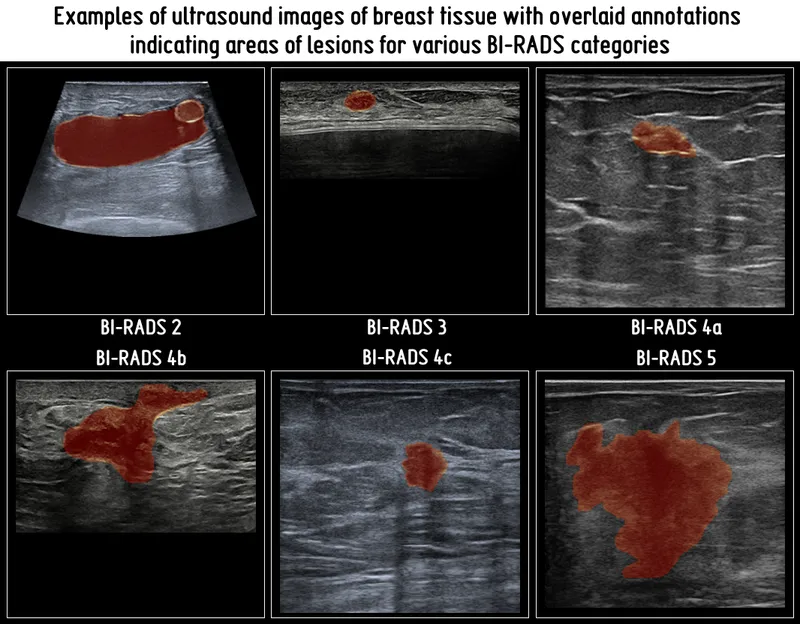
- Role: Differentiates cystic/solid lesions; guides biopsy; adjunct in dense breasts. Key for BI-RADS assessment.
- Malignant signs: Irregular shape, non-circumscribed (spiculated, angular, microlobulated) margins, hypoechoic, posterior shadowing, taller-than-wide.
- Benign signs: Oval/round, circumscribed margins, anechoic (simple cysts), posterior enhancement.
- Doppler: Assesses vascularity, often ↑ in malignancy.
- Breast MRI:
- Indications: High-risk screening (BRCA, >20% lifetime risk), staging (disease extent), problem-solving (occult cancer), NACT response.
- Technique: Pre/post-contrast T1W (fat-sat), T2W, DWI. Gadolinium crucial for DCE-MRI.
- DCE kinetics (BI-RADS MRI):
- Type I (Progressive): Usually benign.
- Type II (Plateau): Suspicious.
- Type III (Washout): Highly suspicious for malignancy.
⭐ MRI is the most sensitive modality for detecting invasive breast cancer, especially in dense breasts and for lobular carcinoma.
BI‑RADS Blueprint - Code Red or Green?
- BI-RADS (Breast Imaging Reporting and Data System) provides a universal language for breast imaging, standardizing mammography, ultrasound, and MRI report conclusions and recommendations.
- Its 7 assessment categories (0-6) are pivotal, directly dictating patient management: from additional evaluation or routine screening to biopsy and confirmed malignancy treatment.
⭐ BI-RADS 3 (Probably Benign) lesions have a <2% risk of malignancy; typically managed with short-term (e.g., 6-month) follow-up, avoiding unnecessary immediate biopsies.
Tissue Tells Tales - Biopsy Truths
- Definitive diagnosis: BI-RADS 4, 5 lesions.
- Core Needle Biopsy (CNB): Gold standard. 14G needle, 3-5 cores. Image-guided (USG, Stereo, MRI).
- Histology: invasive vs. in-situ.
- FNAC (Fine Needle Aspiration Cytology): Limited (axillary nodes, cysts). Cannot differentiate DCIS/IDC.
- VAB (Vacuum-Assisted Biopsy): Microcalcifications, small lesions. Larger samples.
- Specimen: Formalin. Test ER/PR/HER2.

⭐ CNB is preferred over FNAC for initial diagnosis of suspicious breast masses for accuracy and invasiveness assessment.
High‑Yield Points - ⚡ Biggest Takeaways
- Mammography is the primary screening tool, detecting microcalcifications (esp. pleomorphic for DCIS) and masses.
- BI-RADS standardizes reporting, guiding management from benign (BI-RADS 2) to malignant (BI-RADS 5).
- Ultrasound differentiates cystic vs. solid masses, assesses axillary nodes, and guides biopsies.
- Breast MRI is superior for high-risk screening, implant assessment, and occult primary detection.
- IDC, the most common invasive cancer, often presents as a spiculated mass; Triple Assessment is crucial for diagnosis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

