BI-RADS Basics - System Snapshot
BI-RADS (Breast Imaging Reporting and Data System) is a quality assurance tool.
- Primary Goals:
- Standardize breast imaging reporting.
- Facilitate communication among healthcare providers.
- Enable risk assessment.
- Guide patient management.
- Aid in data collection and research.
- Imaging Modalities Covered:
- Mammography
- Breast Ultrasound
- Breast MRI
⭐ The primary purpose of BI-RADS is to standardize breast imaging reporting and to facilitate communication among healthcare providers, thereby improving patient care and outcomes.
BI-RADS Categories - Score & Action
The Breast Imaging Reporting and Data System (BI-RADS) standardizes reporting and guides management based on the likelihood of malignancy.
| Category | Description | LoM (%) | Management |
|---|---|---|---|
| BI-RADS 0 | Incomplete Assessment; further imaging needed for final evaluation. | N/A | Additional imaging (e.g., spot compression, magnification, ultrasound) |
| BI-RADS 1 | Negative; symmetrical, no masses, architectural distortion, or suspicious calcifications. | 0 | Routine screening |
| BI-RADS 2 | Benign Finding(s); e.g., involuting calcified fibroadenoma, simple cysts. | 0 | Routine screening |
| BI-RADS 3 | Probably Benign; finding with <2% risk of malignancy, short-term follow-up. | <2 | Short-interval follow-up (typically 6, 12, 24 months) |
| BI-RADS 4 | Suspicious; requires biopsy. Subcategories stratify risk. | Tissue diagnosis (biopsy) | |
| - 4A | Low suspicion for malignancy. | >2-10 | Biopsy |
| - 4B | Moderate suspicion for malignancy. | >10-50 | Biopsy |
| - 4C | High suspicion, not classic for BI-RADS 5. | >50-95 | Biopsy |
| BI-RADS 5 | Highly Suggestive of Malignancy; classic malignant features. | >95 | Appropriate action (Biopsy then treatment) |
| BI-RADS 6 | Known Biopsy-Proven Malignancy; prior to definitive therapy. | 100 | Treatment as planned (e.g., surgical excision). |
Mammography Lexicon - Finding Clues
Key descriptors:
-
Masses:
- Shape: Round, Oval (often benign); Irregular (suspicious).
- Margin: Circumscribed (benign); Obscured, Microlobulated, Indistinct, Spiculated (suspicious).
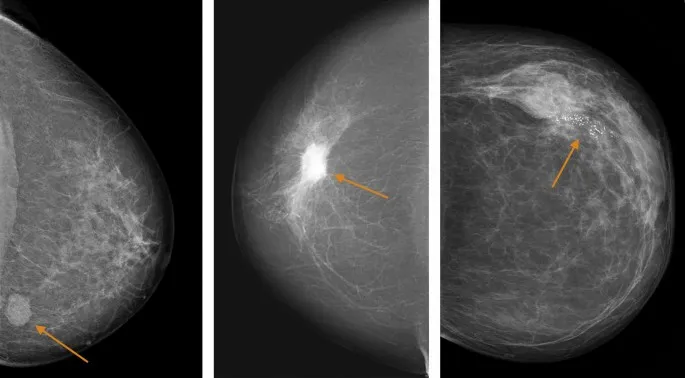
- Density: Fat-containing, Low, Equal, High (vs. fibroglandular tissue).
⭐ Spiculated margins on a mammographic mass are highly suspicious for malignancy.
-
Calcifications: Morphology & Distribution:
Type Benign Examples Suspicious Examples Morphology Round, Popcorn, Vascular, Large rod-like, Rim Pleomorphic, Fine linear/branching, Amorphous, Coarse heterogeneous - Distribution: Diffuse, Regional, Grouped (>5 calcs in <1 cm area), Linear, Segmental.
-
Architectural Distortion: Parenchymal distortion (radiating lines) without definite mass.
-
Asymmetries:
- Focal: <1 quadrant, seen on 2 views.
- Global: ≥1 quadrant.
- Developing: New, ↑size, or ↑conspicuousness.
High‑Yield Points - ⚡ Biggest Takeaways
- BI-RADS 0 signifies an incomplete assessment requiring further imaging.
- BI-RADS 1 (Negative) and BI-RADS 2 (Benign) indicate routine screening.
- BI-RADS 3 (Probably Benign) implies a <2% malignancy risk; short-interval follow-up is key.
- BI-RADS 4 (Suspicious) warrants biopsy; subcategories 4A, 4B, 4C reflect increasing likelihood of malignancy.
- BI-RADS 5 (Highly Suggestive of Malignancy) carries a >95% risk; action is mandatory.
- BI-RADS 6 denotes known biopsy-proven malignancy undergoing treatment.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

