Classification & Fibrocystic Changes - The Usual Suspects
- Benign Lesion Classification (Risk):
- Non-proliferative: No ↑ cancer risk (e.g., cysts, mild hyperplasia).
- Proliferative without atypia: Slight ↑ risk (1.5-2x) (e.g., fibroadenoma, sclerosing adenosis, papilloma).
- Atypical hyperplasia (ADH, ALH): Moderate ↑ risk (4-5x).
- Fibrocystic Changes (FCC):
- Most common benign disorder; peak age 20-50 yrs.
- Hormonally mediated; spectrum: cysts, adenosis, fibrosis.
- Clinical: Cyclical bilateral breast pain (mastalgia), lumpiness.
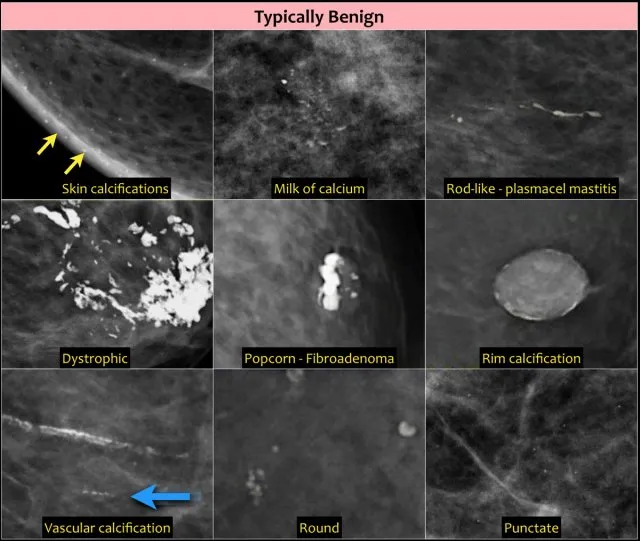
- Mammography: Dense tissue, cysts, "milk of calcium" (layering calcification in cysts).

- Ultrasound: Cysts (anechoic, posterior enhancement), prominent fibroglandular tissue.
⭐ Most FCC (non-proliferative) = no significant cancer risk. Proliferative changes without atypia (e.g., sclerosing adenosis) = slight ↑ risk (1.5-2x).
Fibroadenomas & Hamartomas - Smooth Solid Friends
- Fibroadenoma (FA): Most common benign tumor (15-35 yrs). Estrogen-sensitive.
- Clinical: Painless, firm, mobile "breast mouse".
- Mammography: Well-defined, oval/lobulated mass. "Popcorn" calcifications (older).
- USG: Hypoechoic, wider-than-tall, homogeneous, posterior enhancement. BI-RADS 3.
- Variants: Juvenile, Giant (>5 cm), Complex (cysts >3mm, SA; slight ↑ Ca risk).
- Management: Observe, cryoablation, or excise.
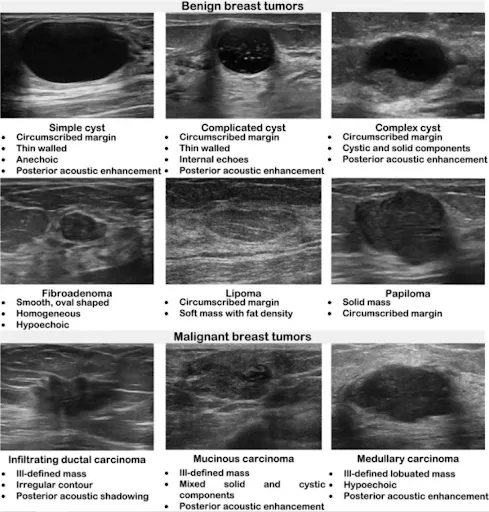
- Hamartoma (Fibroadenolipoma): "Breast within a breast"; contains fat, glandular, fibrous tissue.
- Mammography: Encapsulated, mixed-density (fat & stroma). "Sliced sausage" look.
- USG: Well-defined, heterogeneous (hyperechoic fat, hypoechoic stroma), compressible.
- Management: Reassurance; excise if atypical.
⭐ "Popcorn" calcification in a well-defined mass is highly suggestive of an involuting fibroadenoma.
Ductal & Inflammatory Lesions - Ducts Under Duress
- Duct Ectasia:
- Dilated major subareolar ducts; peri/postmenopausal.
- Nipple discharge (multicolored, sticky), non-cyclical mastalgia, nipple retraction.
- Mammography: Dilated ducts, benign rod-like/secretory calcifications.
- USG: Anechoic/hypoechoic tubular structures, debris, wall thickening.
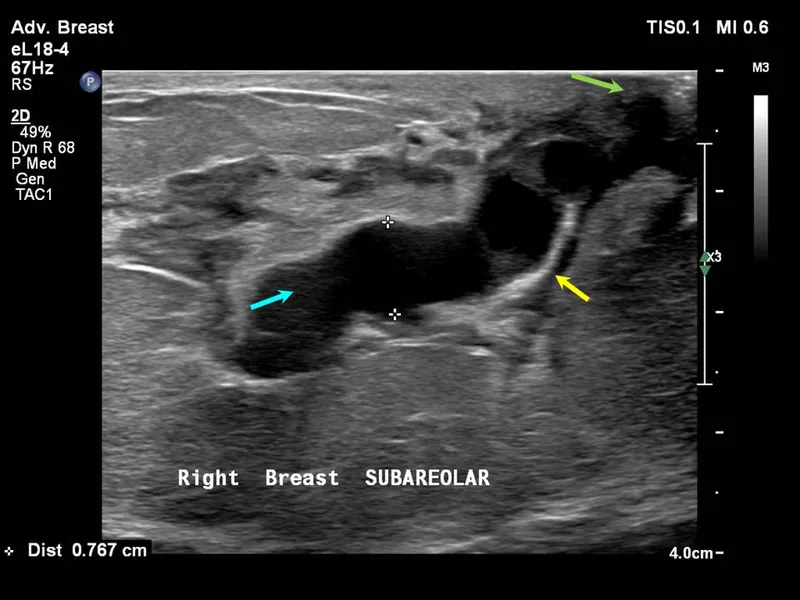
- Periductal Mastitis (Plasma Cell Mastitis):
- Chronic inflammation around ducts, often with ectasia. Lymphoplasmacytic infiltrate.
- Clinical: Pain, erythema; recurrent subareolar abscess/fistula.
- Imaging: Ill-defined retroareolar density (Mammo); USG: hypoechoic collection, duct wall thickening, ↑vascularity.
- Idiopathic Granulomatous Mastitis (IGM):
- Rare, chronic inflammation; diagnosis of exclusion; young parous women. Mimics carcinoma.
- Firm, tender mass; skin changes (erythema, ulceration, fistula).
- USG: Ill-defined hypoechoic mass/collection, tubular extensions, ↑vascularity. Histology: non-caseating granulomas.
⭐ IGM is often associated with Corynebacterium kroppenstedtii.
- Mammary Duct Fistula (Zuska's Disease):
- Recurrent retroareolar abscess/fistula.
- Patho: Squamous metaplasia of lactiferous ducts. 📌 Strongly linked to smoking.
- USG: Delineates fistulous tract, collection.
Benign Mimics & BI-RADS - Spotting the Safes
- Common Benign Mimics of Malignancy:
- Radial Scar/Complex Sclerosing Lesion: Stellate, mimics invasive cancer.
- Fat Necrosis: Post-trauma/surgery; variable (oil cysts, spiculated).
- Diabetic Mastopathy: Hard, ill-defined masses in Type 1 DM.
- Granulomatous Mastitis: Inflammatory changes, can mimic IBC.
- BI-RADS Categories for Benign/Likely Benign:
- BI-RADS 1: Negative. Routine screening.
- BI-RADS 2: Benign (e.g., simple cysts, stable fibroadenomas, secretory calcifications). Routine screening.
- BI-RADS 3: Probably Benign. Requires short-interval follow-up (typically 6 months).
⭐ A classic BI-RADS 3 lesion has a <2% likelihood of malignancy; short-term follow-up is key to confirm stability.
High‑Yield Points - ⚡ Biggest Takeaways
- Fibroadenoma: Most common benign solid tumor in young women; well-defined, may show "popcorn" calcification.
- Fibrocystic changes: Most common overall breast lesion; characterized by cyclical pain, cysts, adenosis, and fibrosis.
- Intraductal papilloma: Leading cause of pathological nipple discharge (often bloody); typically solitary and subareolar.
- Galactocele: Milk-filled cyst occurring during or after lactation; classically demonstrates a fat-fluid level.
- Fat necrosis: Post-trauma/surgery, mimics malignancy; oil cysts and dystrophic calcifications are key features.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

