Foundations of AI in Chest Imaging - Pixels to Predictions
⭐ Deep learning, particularly Convolutional Neural Networks (CNNs), has revolutionized image recognition tasks in radiology.
- Core Concepts:
- Artificial Intelligence (AI): Machines mimicking human intelligence.
- Machine Learning (ML): AI subset; systems learn from data.
- Supervised: Learns from labeled data (e.g., "nodule" vs "no nodule"). Requires large, annotated datasets.
- Unsupervised: Identifies patterns in unlabeled data.
- Deep Learning (DL): ML using complex, multi-layered neural networks.
- Convolutional Neural Networks (CNNs): Specialized for image recognition; vital for chest imaging.
- Data is Key: AI performance heavily relies on quality and quantity of imaging data.
AI for Lung Nodule & Cancer Dx - Spotting Shadows
- AI significantly augments radiologist capabilities in lung nodule and cancer management using CT imaging.
- Core AI Functions:
- Detection (CADe):
- Boosts sensitivity for subtle/small nodules (e.g., < 6mm), including ground-glass opacities (GGOs).
- Reduces missed diagnoses in high-volume Low-Dose CT (LDCT) screening.
- Characterization (CADx):
- Analyzes nodule features: size, volume, density (solid/subsolid), morphology (spiculation, margins).
- Aids standardized risk stratification (e.g., Lung-RADS).
- Predicts malignancy likelihood, guiding workup.
- Monitoring:
- Precise volumetric tracking of nodule growth or treatment response over serial scans.
- Detection (CADe):
- Impact: ↑ Accuracy, earlier cancer detection, enhanced workflow efficiency.
- Considerations: Managing false positives, algorithm robustness & generalizability.
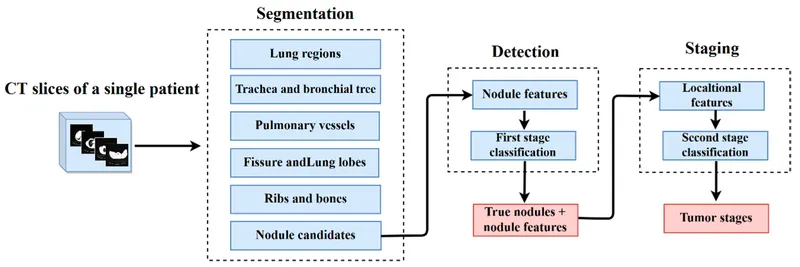
⭐ AI algorithms significantly improve detection rates for small pulmonary nodules (e.g., < 5mm) in low-dose CT lung cancer screening.
AI in Lung Infections & ILD - Clearing the Haze
- Lung Infections (e.g., Pneumonia, COVID-19, TB):
- Automated detection & segmentation of opacities, consolidations.
- Supports differentiation (e.g., bacterial vs. viral patterns).
- AI-driven severity scores (e.g., >30% lung involvement in COVID-19).
- TB: Nodule/cavity detection, monitoring treatment efficacy.
- Interstitial Lung Diseases (ILD):
- Early detection of subtle interstitial changes (reticulation, ground-glass, honeycombing).
- Assists in classifying complex ILD patterns (e.g., UIP vs. NSIP).
- Quantifies extent of fibrosis, monitors disease progression.
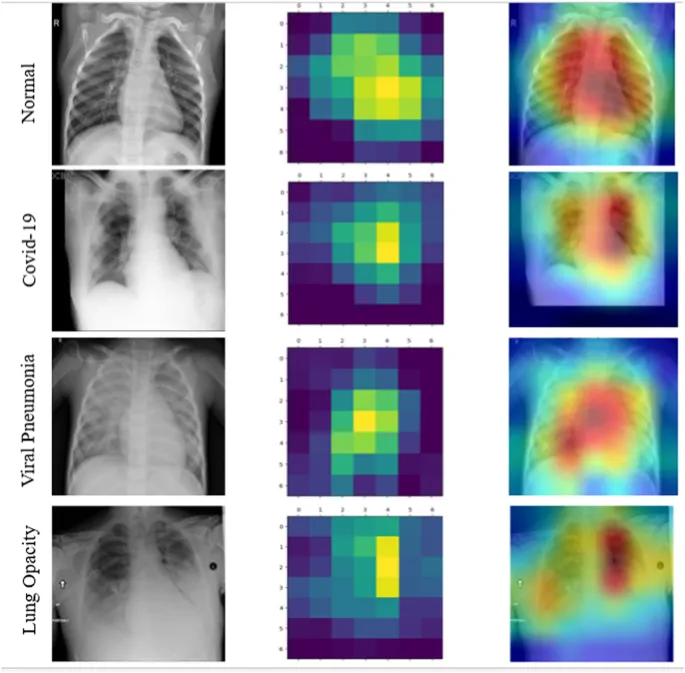
⭐ AI tools can rapidly quantify lung opacities in COVID-19 pneumonia, aiding in severity assessment and triage.
AI for Other Thoracic Findings & Challenges - Wider View & Hurdles
- Broader AI Applications:
- Pleural Effusion: Detection, characterization, volume estimation.
- Pneumothorax: Rapid CXR identification, critical in emergencies.
- Interstitial Lung Disease (ILD): Aids pattern recognition, classification.
- Cardiomegaly: Automated cardiothoracic ratio (CTR) for heart size.
- Rib Fractures: Improved detection on CXR & CT.
- Key Hurdles & Outlook:
- Data: Quality, quantity, diversity, annotation challenges.
- Generalizability: Performance consistency across new data/settings.
- Interpretability: "Black box" issue; need for explainable AI (XAI).
- Integration: Smooth workflow adoption, user acceptance.
- Regulatory: Standardized validation, ethical guidelines.
⭐ Key challenges for AI in radiology include data heterogeneity, generalizability to new populations, and the "black box" nature of some algorithms.
High‑Yield Points - ⚡ Biggest Takeaways
- AI (CAD) aids nodule detection (CXR/CT) for early lung cancer screening.
- Key for quantifying opacities in pneumonia, COVID-19, and ARDS.
- Effective for TB screening on CXRs, especially in high-burden areas.
- Enables rapid pneumothorax detection on chest X-rays, improving triage.
- Growing use in ILD pattern recognition and disease quantification.
- AI can reduce workload and potentially enhance diagnostic accuracy.
- Understand AI limitations: bias and need for robust validation.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more


