AI Applications in Abdominal Imaging - AI's Abdominal Debut
- Core AI Concepts:
- Machine Learning (ML): Algorithms learn from data to make predictions.
- Deep Learning (DL): Advanced ML using neural networks; excels in image analysis.
- Key Application Areas:
- Detection: Identifying abnormalities (e.g., liver lesions, polyps).
- Segmentation: Outlining organs/lesions precisely (e.g., kidney volume, tumor boundaries).
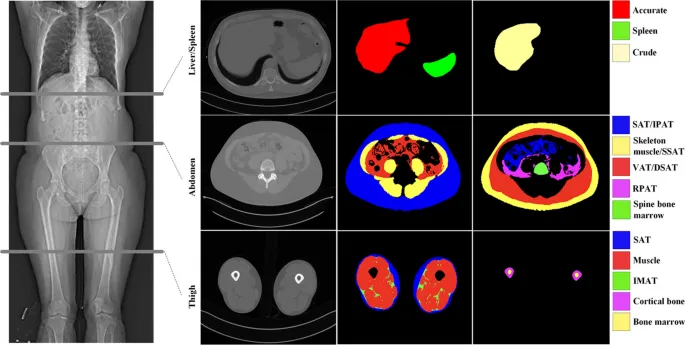
- Characterization: Differentiating benign vs. malignant lesions (e.g., adrenal nodules).
- Workflow Optimization: Prioritizing urgent cases, automating measurements.
⭐ AI algorithms show high accuracy in detecting colorectal polyps during colonoscopy, potentially improving early cancer diagnosis rates.
- Impact: ↑Diagnostic accuracy, ↓Workload, personalized medicine potential in abdominal radiology (CT, MRI, USG).
AI Applications in Abdominal Imaging - Smart Scan Sorcery
AI enhances abdominal CT, MRI, & US interpretation, boosting diagnostic precision & workflow efficiency.
- Liver Applications (Hepato-AI):
- Lesion Management:
- Automated detection & characterization of HCC, metastases.
- Supports LI-RADS scoring consistency.
- Diffuse Liver Disease:
- Precise steatosis quantification (NAFLD/NASH monitoring).
- Non-invasive fibrosis assessment (e.g., AI with MRE/elastography).
- Lesion Management:
- Pancreatic Applications (Pancreatico-AI):
- Cancer Detection:
- Early, subtle PDAC identification on CT/MRI.
- Aids differentiating malignant tumors from focal pancreatitis.
- Cystic Lesion Analysis:
- Characterizes IPMNs, MCNs; aids risk stratification.
- Cancer Detection:
- Overall Impact:
- ↑ Diagnostic accuracy, ↓ inter-observer variability.
- Optimized workflows, potentially faster report turnaround.
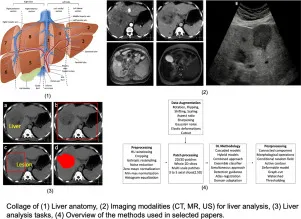
⭐ AI algorithms can quantify liver steatosis on unenhanced CT with high accuracy (often >0.90 AUC), aiding opportunistic NAFLD screening.
AI Applications in Abdominal Imaging - Organ Intelligence Ops
- Kidneys:
- AI for early detection & characterization of renal masses (e.g., differentiating cysts vs. solid tumors, RCC subtyping).
- Automated segmentation for precise kidney volumetry (monitoring CKD, transplant assessment).
- Enhanced detection, localization, and sizing of urolithiasis (renal stones) on CT/ultrasound.
- Spleen:
- Accurate splenic volumetry using AI for assessing splenomegaly in portal hypertension or hematological disorders.
- Improved detection and characterization of focal splenic lesions (e.g., infarcts, metastases).
- Bowel (Small & Large Intestine):
- Computer-Aided Detection (CADe) & Diagnosis (CADx) for colonic polyps during virtual or optical colonoscopy.
- AI-driven assessment of Inflammatory Bowel Disease (IBD) activity and severity from CT/MR enterography.
- Detection of critical findings like bowel obstruction, ischemia, and perforation.
⭐ AI tools can significantly increase the adenoma detection rate (ADR) during colonoscopy, particularly for subtle or flat polyps, which are often missed.
AI Applications in Abdominal Imaging - AI's Next Chapter
- Current Challenges:
- Data heterogeneity, ensuring quality.
- Generalizability across diverse populations & scanners.
- Navigating complex regulatory approvals (e.g., FDA).
- Addressing ethical concerns: algorithmic bias, data privacy.
- Future Directions:
- Radiomics: Extracting high-dimensional quantitative data.
- Integrated diagnostics: Fusing AI insights with clinical & genomic data.
- Workflow optimization: Automating tasks, improving reporting efficiency.
- AI-driven personalized treatment planning.
- Federated learning for secure multi-center data analysis.
⭐ AI facilitates opportunistic screening (e.g., osteoporosis, sarcopenia, vascular calcification) on abdominal CTs performed for other primary indications.
High‑Yield Points - ⚡ Biggest Takeaways
- AI excels in detecting & characterizing liver lesions (HCC, metastases) and pancreatic cancer on CT/MRI.
- Automated organ segmentation (liver, spleen) enables precise volumetric analysis for pre-operative planning.
- AI algorithms aid diagnosis of acute appendicitis, bowel obstruction, and kidney stones on CT.
- CAD significantly improves colorectal polyp detection during CT colonography (virtual colonoscopy).
- AI-driven quantitative imaging biomarkers provide insights into tumor grading and predicting therapy response.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

