Spleen: Anatomy & Imaging - Spleen Scene Setter
- Location & Size: LUQ, intraperitoneal. Avg. 12x7x4 cm. Wt: ~150g.
- 📌 Mnemonic "1,3,5,7,9,11": 1x3x5 inches, 7 oz, deep to ribs 9-11.
- Vasculature: Splenic artery (from celiac trunk); Splenic vein (joins SMV → portal vein).
- Imaging:
- USG: Homogeneous, echogenic cf. liver.
- CECT: Gold standard. Homogeneous enhancement. NECT: 40-60 HU.
- MRI: T1 hypointense, T2 hyperintense.

⭐ Accessory spleen (splenunculus): Most common congenital anomaly, often at hilum; found in up to 30% of cases at autopsy/CT.
Splenomegaly & Diffuse Disease - The Swollen Spleen
- Definition: Spleen length > 12-13 cm or weight > 200g.
- Common Causes:
- Congestive: Portal hypertension (cirrhosis), heart failure.
- Infective: Malaria, Kala-azar, EBV, TB.
- Hematological: Leukemias, lymphomas, hemolytic anemias, myeloproliferative disorders.
- Storage: Gaucher's, Niemann-Pick.
- Inflammatory: Sarcoidosis, SLE.
- Imaging:
- USG: Measures size, assesses echotexture. Doppler for portal flow.
- CT/MRI: Confirms size, evaluates density/signal, aids in identifying cause.
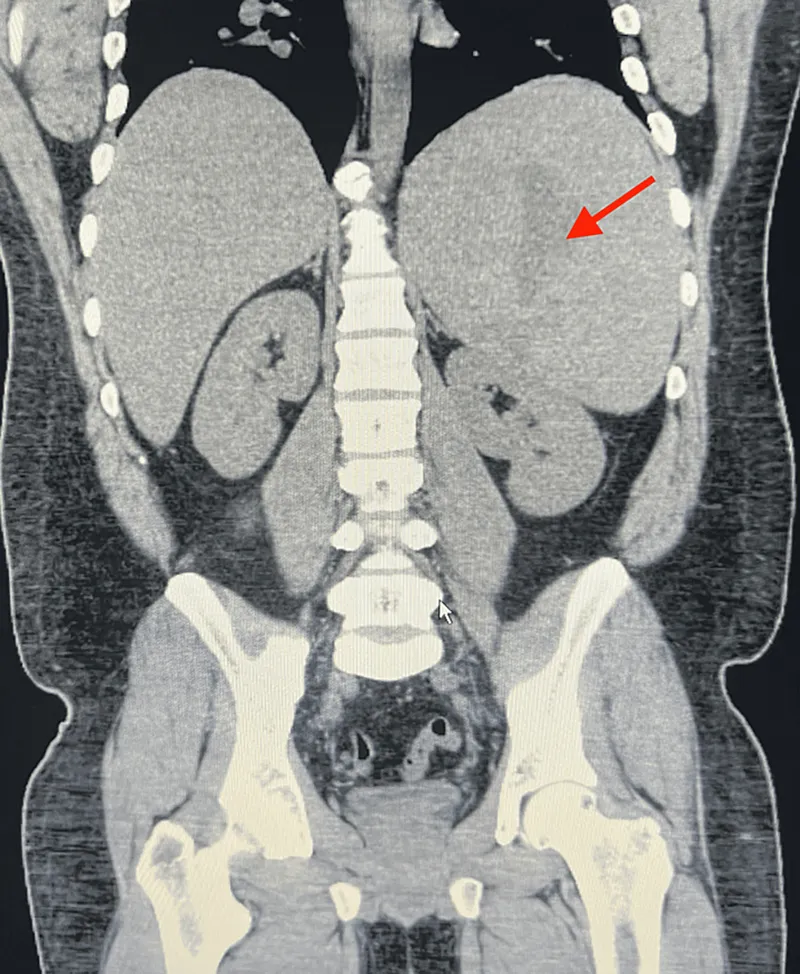
⭐ In portal hypertension, USG may show dilated portal vein (>13mm), splenic vein (>10mm), collaterals, and ascites.
Focal Splenic Lesions - Spleen Spotting
- Common Benign: Simple cyst, Hemangioma, Hamartoma.
- Common Malignant: Lymphoma, Metastases (melanoma, lung, breast, ovary).
- Infectious/Inflammatory: Abscess, Granulomas (TB, sarcoidosis).
| Lesion | CECT Appearance | Key Differentiator(s) |
|---|---|---|
| Simple Cyst | Water density (<20 HU), non-enhancing | Sharply marginated, anechoic on USG |
| Hemangioma | Peripheral nodular enhancement, centripetal fill | Often hyperechoic on USG |
| Lymphoma | Hypodense, homogeneous, poor enhancement | Often multiple, splenomegaly |
| Metastases | Variable, often hypovascular | History of primary malignancy |
| Abscess | Rim-enhancing, central low attenuation, +/- gas | Clinical signs of infection (fever) |
⭐ Splenic lymphoma is the most common malignant tumor of the spleen, often presenting as diffuse infiltration or multiple nodules rather than a single discrete mass.
Splenic Trauma - Spleen Under Siege
- Most common: blunt trauma. CT is gold standard. Non-operative management (NOM) for stable patients.
- AAST Splenic Injury Grading:
| Grade | Description |
|-------|-----------------------------------------------------------------------------|
| I | Subcapsular hematoma <10%; Capsular tear <1cm |
| II | Hematoma 10-50% or intraparenchymal <5cm; Laceration 1-3cm |
| III | Hematoma >50% or ruptured; Intraparenchymal >5cm; Laceration >3cm |
| IV | Laceration involving segmental/hilar vessels (>25% devascularization) |
| V | Shattered spleen; Hilar vascular injury devascularizing spleen |

⭐ Kehr's sign: referred left shoulder pain, may indicate splenic rupture due to diaphragmatic irritation.
Lymph Nodes & Lymphoma - Node Network News
- Normal Nodes: Oval, fatty hilum. Short axis: Abdomen/Pelvis <10mm; Mesentery <5mm.
- Benign vs. Malignant Node Features:
Feature Benign Malignant Shape Oval, reniform Round Hilum Fatty, preserved Lost, effaced Calcification Granulomatous (TB) Treated lymphoma, some mets Necrosis TB, suppurative Common, esp. high-grade - Lymphoma:
- Bulky, homogeneous adenopathy; splenomegaly common.
- NHL: Commoner, often extranodal. HL: Contiguous spread.

- Ann Arbor Staging (Simplified):
Stage Involvement I Single LN region or single extralymphatic (IE) II ≥2 LN regions, same side diaphragm III Both sides diaphragm; +/- Spleen (S) IV Diffuse extralymphatic disease - B-symptoms: Fever, night sweats, wt loss >10%. E: Extranodal.
⭐ "Floating aorta sign" or "Sandwich sign": Mesenteric/retroperitoneal nodes encasing vessels, characteristic of lymphoma.
High‑Yield Points - ⚡ Biggest Takeaways
- Splenomegaly (>12 cm length): common, due to portal hypertension, hematological disorders.
- Splenic trauma: most common in blunt injury; note Kehr's sign, use AAST grading.
- Splenic infarcts: wedge-shaped peripheral defects; causes include embolic, hematologic.
- Accessory spleen (splenunculus): common congenital variant, usually near splenic hilum.
- Lymphadenopathy (>1 cm short axis): suggests malignancy/infection; PET-CT for lymphoma staging.
- Splenic calcifications: often from old granulomatous disease (TB) or healed infarcts.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

