Male Pelvic Anatomy & Modalities - Pixel Perfect Pelvis
- Key Structures & Zones:
- Prostate: Peripheral (PZ - commonest cancer site), Central (CZ), Transitional (TZ - BPH site).
- Seminal Vesicles (SVs), Vas Deferens, Ejaculatory Ducts.
- Bladder, Urethra, Rectum.

- Primary Imaging Modalities:
- USG: TRUS for prostate (biopsy, volume); TAUS for bladder.
- MRI: Best soft tissue. Multiplanar.
- Prostate: T2WI (zonal anatomy), DWI (malignancy), DCE (vascularity). PI-RADS (1-5).
- Local staging: prostate, rectal, bladder cancers.
- CT: Trauma, bony pelvis, calcifications, gross nodal/distant mets.
- Fluoroscopy: RGU/VCUG for urethral strictures, VUR.
⭐ On T2-MRI, prostate cancer in PZ often appears as a low signal intensity focus.
Prostate Gland Imaging - Gland Central Station
- Modalities:
- Transrectal Ultrasound (TRUS): Biopsy guidance, initial assessment.
- Multiparametric MRI (mpMRI): Gold standard for detection, staging, and active surveillance of prostate cancer. Sequences: T2W, DWI, DCE.
- CT: Limited for primary tumor; useful for nodal/metastatic disease.
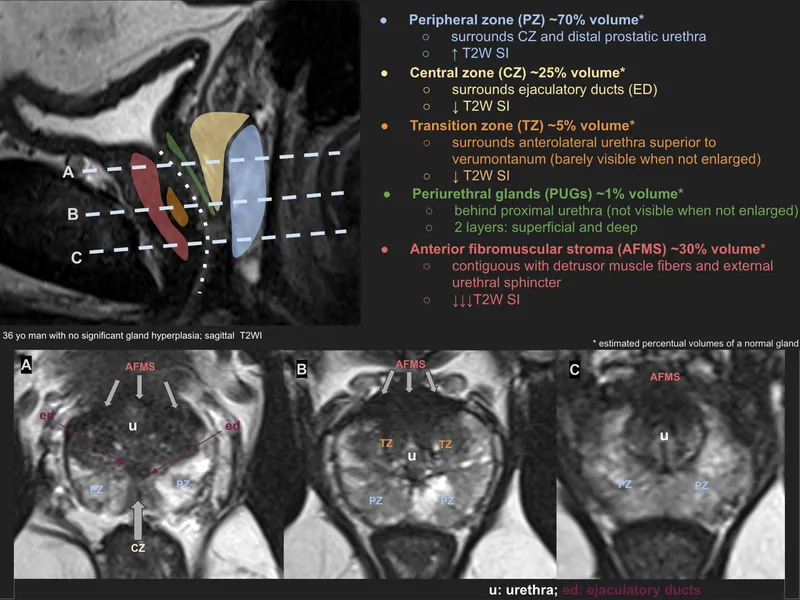
- Zonal Anatomy (T2W MRI):
- Peripheral Zone (PZ): ~70% cancers. High T2 signal.
- Transition Zone (TZ): BPH origin. Heterogeneous T2 signal.
- Central Zone (CZ): Low T2 signal.
- Anterior Fibromuscular Stroma (AFMS): Very low T2 signal.
- Prostate Cancer on mpMRI:
- PZ: T2 hypointense, restricted diffusion (low ADC), early enhancement.
- TZ: More challenging; ill-defined, homogenous, T2 hypointense, lenticular.
- PI-RADS (Prostate Imaging Reporting and Data System):
- Standardized reporting for cancer risk (Score 1-5).
- Dominant sequence: PZ (DWI), TZ (T2W).
⭐ Most prostate cancers (~70-80%) arise in the Peripheral Zone (PZ).
Testicular & Scrotal Imaging - Testicular Tales
- Ultrasound (USG): Primary modality. High-frequency linear probe (7.5-12 MHz).
- Normal Testis: Homogeneous, mid-grey. Size: 3-5 cm (L). Volume: ~20 ml.
- Color Doppler: Crucial for vascularity.
- Key Conditions:
- Testicular Torsion:
- Acute pain.
- USG: Enlarged, hypoechoic testis. ↓/absent Doppler flow. Whirlpool sign of cord.
- ⚠️ Surgical emergency: salvage ↓ after 6 hrs.
- Epididymo-orchitis:
- Pain, fever.
- USG: Enlarged epididymis &/or testis. ↑ Doppler flow. Reactive hydrocele.
- Varicocele:
- Dilated pampiniform veins (>2-3 mm), ↑ with Valsalva. Usually left.
- Hydrocele:
- Anechoic fluid in tunica vaginalis.
- Testicular Tumors:
- Seminoma: Hypoechoic, homogeneous.
- NSGCT: Heterogeneous.
- Markers: AFP, β-hCG.
- Testicular Torsion:

⭐ "Bell-clapper" deformity, where the tunica vaginalis has an abnormally high attachment to the spermatic cord, is a major predisposing factor for testicular torsion.
Penile & Urethral Pathologies - Pointing Out Problems
- Penile Pathologies:
- Peyronie's Disease: Fibrous plaques (tunica albuginea) → penile curvature. USG: calcified plaques.
- Priapism: Erection >4 hrs. Doppler USG: Ischemic (low flow) vs. Non-ischemic (high flow).
- Penile Fracture: Tunica albuginea rupture. "Eggplant deformity". USG/MRI. RGU if urethral injury suspected.
- Penile Cancer (SCC): MRI for local staging, inguinal node assessment.

- Urethral Pathologies:
- Urethral Strictures: Fibrotic narrowing. RGU/VCUG (MCU) for diagnosis, location, length.
- Urethral Trauma:
- Anterior: Straddle injury. RGU.
- Posterior: Pelvic fracture. 📌 "High-riding prostate".
- Urethral Diverticula: Outpouching. VCUG/RGU, MRI.
- Urethral Cancer (SCC): Rare. RGU, MRI for staging.
⭐ Posterior urethral injury (pelvic fracture): "High-riding prostate" on imaging due to hematoma. RGU often deferred or performed with caution after initial stabilization (e.g., suprapubic catheter).
High‑Yield Points - ⚡ Biggest Takeaways
- MRI is gold standard for prostate cancer staging (TNM) and local recurrence detection.
- TRUS is key for prostate biopsy guidance and evaluating male infertility (e.g., ejaculatory duct obstruction).
- Testicular torsion: Color Doppler US shows absent testicular blood flow - a surgical emergency.
- Varicocele: Ultrasound with Valsalva identifies dilated pampiniform plexus veins (>2-3mm).
- Zinner syndrome: Triad of seminal vesicle cyst, ejaculatory duct obstruction, ipsilateral renal agenesis.
- RGU/MCU are crucial for evaluating urethral injuries, especially post-trauma.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

