Peritoneal & Retroperitoneal Anatomy - Mapping the Maze
- Peritoneal Cavity: Serous membrane-lined space, divided into Greater and Lesser Sacs.
- Greater Sac: Main, larger portion of the peritoneal cavity.
- Lesser Sac (Omental Bursa): Smaller sac posterior to the stomach. Communicates with Greater Sac via Foramen of Winslow (epiploic foramen).
- Key Fluid Collection Sites (Potential Spaces):
- Morison's Pouch (hepatorenal space): Most dependent part of upper abdomen when supine.
- Pouch of Douglas (rectovesical or rectouterine pouch): Most dependent part of peritoneal cavity in pelvis.
- Paracolic Gutters (right & left): Channels for fluid and spread of infection/malignancy.
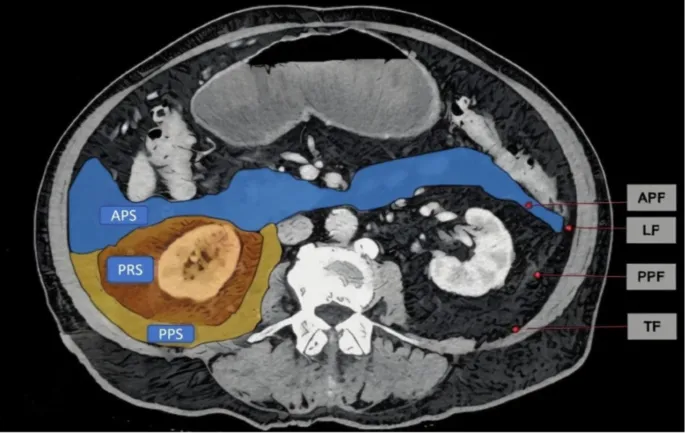
- Retroperitoneum: Space posterior to the parietal peritoneum.
- Anterior Pararenal Space: Contains pancreas, duodenum (2nd-4th parts), ascending & descending colon.
- Perirenal Space: Encases kidneys, adrenal glands, ureters, aorta, IVC, and perirenal fat.
- Posterior Pararenal Space: Contains fat and nerves.
⭐ The right paracolic gutter is typically wider and deeper than the left, providing a major pathway for fluid movement from the pelvis to the upper abdomen, particularly Morison's pouch.
Imaging Modalities - Picking Your Probe
- X-ray (KUB): Initial: gas, calcifications, foreign bodies. Limited soft tissue.
- Ultrasound (USG): First-line: free fluid, collections, biliary/renal. Real-time, no radiation. Guides interventions. Doppler.
- Computed Tomography (CT): Workhorse: trauma, acute abdomen, staging.
- NCCT: Calculi, hemorrhage.
- Arterial Phase (20-30s): Hypervascular lesions, CTA.
- Portal Venous Phase (60-70s): Standard, parenchymal organs.
- Delayed Phase (3-15 min): GU tract, cholangiocarcinoma, washout.
- 📌 Phases: No Apple Pie Daily (Non-contrast, Arterial, Portal, Delayed).
- Magnetic Resonance Imaging (MRI): Problem-solving, superior soft tissue (e.g., rectal Ca staging). No radiation.

⭐ CT is the primary modality for evaluating acute abdomen and is crucial for detecting and staging peritoneal carcinomatosis.
Peritoneal Pathologies - Cavity Conundrums
- Ascites: Fluid accumulation.
- Types: Transudative (cirrhosis), Exudative (infection, malignancy).
- Imaging: USG (anechoic/complex), CT (fluid density, displaced bowel loops).
- Sites: Morison's pouch, paracolic gutters, Pouch of Douglas.
- Peritonitis: Peritoneal inflammation.
- Causes: Infection (bacterial, TB), sterile.
- CT: Peritoneal thickening/enhancement, mesenteric stranding, abscess.
- TB Peritonitis:
- Types: Wet (ascites), Dry (adhesions), Fibrotic-fixed (masses).
- CT: Smooth peritoneal thickening, omental caking, low-density nodes.
- Peritoneal Carcinomatosis: Peritoneal metastases.
- Primaries: Ovarian, gastric, colorectal.
- CT: Nodular peritoneal/omental thickening (caking), malignant ascites.

- Hernias: Organ protrusion via defect.
- Types: Inguinal, femoral, umbilical, incisional, internal.
- CT: Defines hernia, contents, complications (strangulation).
⭐ Sister Mary Joseph Nodule: Umbilical metastasis, often from GI/gynecological cancers, indicating peritoneal spread.
Retroperitoneal Pathologies - Behind-the-Lining Lesions
- Key sign: Anterior displacement of bowel/pancreas. Spaces: Anterior pararenal, perirenal, posterior pararenal.
- Retroperitoneal Collections:
- Hematoma: Trauma, anticoagulation, AAA rupture. CT: Acute hyperdense, chronic hypodense. Sentinel clot sign.
- Abscess: Pancreatitis, pyelonephritis, IBD. CT: Rim-enhancing fluid, gas bubbles, inflammatory stranding.
- Retroperitoneal Tumors:
- Primary: Liposarcoma (most common, CT: fat attenuation), leiomyosarcoma.
- Secondary: Lymphoma (commonest), metastases (renal, adrenal, GI).
- Retroperitoneal Fibrosis (Ormond's Disease):
- Idiopathic (70%) or secondary (malignancy, drugs, infection).
- CT/MRI: Periaortic/peri-iliac enhancing soft tissue, encasing structures (e.g., ureters leading to hydronephrosis).
⭐ In idiopathic Retroperitoneal Fibrosis, ureters are typically drawn medially; lateral displacement suggests malignancy.

High‑Yield Points - ⚡ Biggest Takeaways
- CT is the primary modality for evaluating peritoneal and retroperitoneal pathology.
- Pneumoperitoneum: Upright CXR for initial detection; CT confirms and localizes source.
- Ascites: CT attenuation helps differentiate types (transudate, exudate, blood).
- Retroperitoneal spaces (anterior pararenal, perirenal, posterior pararenal) are key for localization.
- Mesenteric ischemia: CTA is crucial; look for vascular signs, bowel changes, pneumatosis.
- Peritoneal carcinomatosis: CT reveals omental caking, nodules, and malignant ascites.
- Retroperitoneal fibrosis: CT/MRI shows peri-aortic/ureteric soft tissue encasement.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

