Sedatives, Hypnotics, Anxiolytics - The Chill Pill Problem
SHAs are psychoactive drugs that depress Central Nervous System (CNS) function, widely used for therapeutic purposes but with high abuse potential.
- Sedatives: Reduce excitement, induce calmness.
- Hypnotics: Primarily induce or maintain sleep.
- Anxiolytics: Specifically reduce anxiety.
| Class | Key Examples |
|---|---|
| Benzodiazepines | Diazepam, Lorazepam, Alprazolam |
| Barbiturates | Phenobarbital, Secobarbital |
| Z-drugs (Non-BZD hypnotics) | Zolpidem, Zopiclone, Eszopiclone |
 |
⭐ Benzodiazepines are the most commonly abused prescription drugs in this class, often initiated for legitimate medical reasons.
SHA Pharmacology - Brain on Brakes
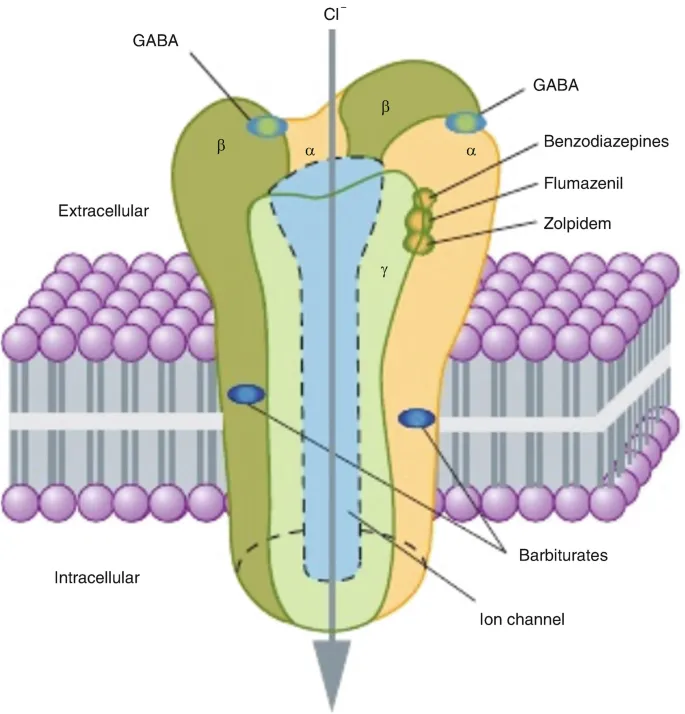
- Mechanism: Enhance GABA at GABA-A receptors → ↑ Cl- influx → hyperpolarization.
- BZDs: ↑ FREquenZy of Cl- channel opening (GABA-dependent). 📌 BenZos!
- Barbiturates: ↑ DURATion of Cl- channel opening. High doses: direct opening. 📌 BarbiDURATes!
- Kinetics:
- Lipid solubility: ↑ solubility → faster onset.
- Half-life: Short (↑ abuse/withdrawal severity), intermediate, long (smoother withdrawal).
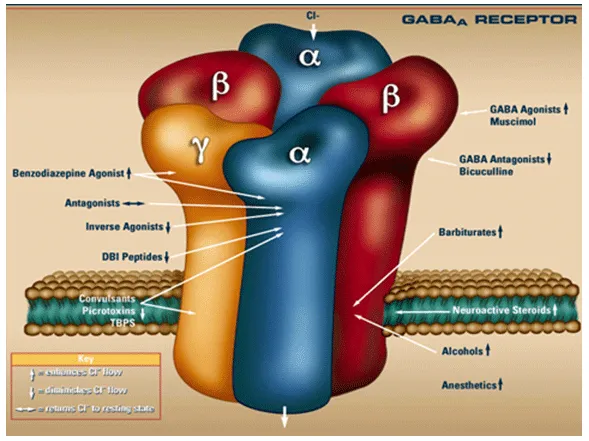
⭐ Barbiturates increase GABA-A Cl- channel opening duration (direct at high doses); BZDs increase frequency (GABA needed).
SHA Intoxication - Too Much Calm
- Clinical Features: Slurred speech, incoordination, ataxia, nystagmus, ↓cognition, stupor/coma, respiratory depression.
- Diagnosis: Clinical; urine toxicology.
- Overdose Comparison:
Feature Benzodiazepines (BZD) Barbiturates Resp. Depression Mild (severe if +others) Severe CVS Effects Minimal Hypotension, shock Flumazenil Yes (cautious) No
⭐ Flumazenil: precipitates seizures in chronic BZD users/TCA co-ingestion. Not for resp. depression if other depressants involved.
SHA Withdrawal - Rebound Storm
CNS hyperexcitability due to abrupt cessation/reduction. Onset/duration varies:
| Agent Type | Onset | Peak | Duration | Notes |
|---|---|---|---|---|
| Short-acting | 12-24 hrs | 24-72 hrs | 5-10 days | Higher seizure risk |
| Long-acting | 2-7 days | 5-8 days | 10-16+ days | Milder, protracted symptoms |
- Barbiturate Withdrawal: Generally more dangerous than BZD withdrawal; higher risk of hyperthermia, cardiovascular collapse, status epilepticus.
- Assessment: CIWA-B (Benzodiazepines). Score >10 may need medication.
- Management:
- Principle: Gradual taper (10-25% every 1-2 weeks).
- Substitution: Convert to equivalent long-acting BZD (Diazepam, Chlordiazepoxide). Phenobarbital for barbiturate or severe/refractory BZD withdrawal.
⭐ Withdrawal from high-dose, short-acting BZDs or barbiturates can be life-threatening, with seizures (typically 2-8 days after cessation for BZDs) and delirium being major concerns.
SHA Dependence Treatment - Breaking Free
- Diagnosis: Based on DSM-5 criteria for SHA Use Disorder.
- Detoxification: Cornerstone is a slow, gradual taper.
⭐ A slow, gradual taper (e.g., reducing equivalent daily diazepam dose by 10-25% every 1-2 weeks, or slower for long-term high-dose users) is crucial for managing benzodiazepine dependence to minimize withdrawal severity and improve success rates.
- Pharmacological: Limited role; anticonvulsants for protracted withdrawal.
- Psychosocial Interventions: CBT, motivational interviewing, group & family therapy.
- Relapse Prevention: Key for sustained recovery.
High‑Yield Points - ⚡ Biggest Takeaways
- Benzodiazepines (BZDs) and Barbiturates are primary sedative-hypnotics.
- BZDs ↑ GABA-A channel opening frequency; Barbiturates ↑ duration of opening.
- Intoxication features CNS depression, slurred speech, ataxia; respiratory depression risk ↑ with alcohol.
- Withdrawal syndrome: anxiety, insomnia, tremors, autonomic hyperactivity, seizures (life-threatening).
- Flumazenil is the antidote for BZD overdose; supportive care for barbiturates.
- Barbiturate withdrawal is generally more severe than BZD withdrawal.
- Significant cross-tolerance exists with alcohol and other CNS depressants.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

