Hallucinogens Overview - Trippy Toxins Taxonomy
- Definition: Psychoactive agents causing profound alterations in perception (hallucinations, illusions), mood, and cognition. Effects are highly variable.
- Key Classes & Examples:
- Indoleamines (Serotonergic):
- LSD (Lysergic acid diethylamide) - potent, synthetic.
- Psilocybin (from 'magic mushrooms') - natural.
- DMT (Dimethyltryptamine) - natural/synthetic.
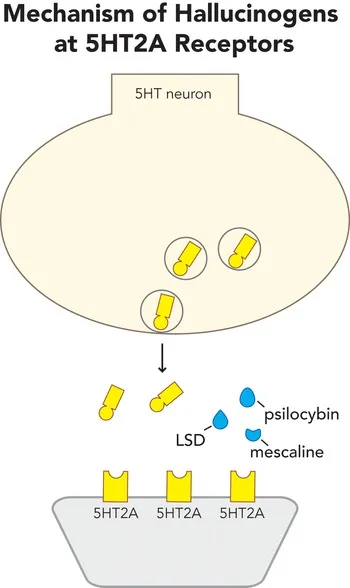
- Mechanism: Primarily 5-HT2A receptor agonists.
- Phenylethylamines:
- Mescaline (from peyote cactus) - natural.
- DOM (2,5-Dimethoxy-4-methylamphetamine) - synthetic.
- MDMA (Ecstasy) - synthetic, also stimulant.
- Dissociative Anesthetics:
- PCP (Phencyclidine) - synthetic.
- Ketamine - synthetic, medical use.
- Mechanism: NMDA receptor antagonists.
- Anticholinergics (Deliriants): Datura, Atropine (plant-derived).
 , and typical examples)
, and typical examples)
- Indoleamines (Serotonergic):
⭐ Examples: LSD, Psilocybin (mushrooms), Mescaline (peyote), DMT, PCP, Ketamine.
Mechanisms of Action - Brain's Serotonin Symphony
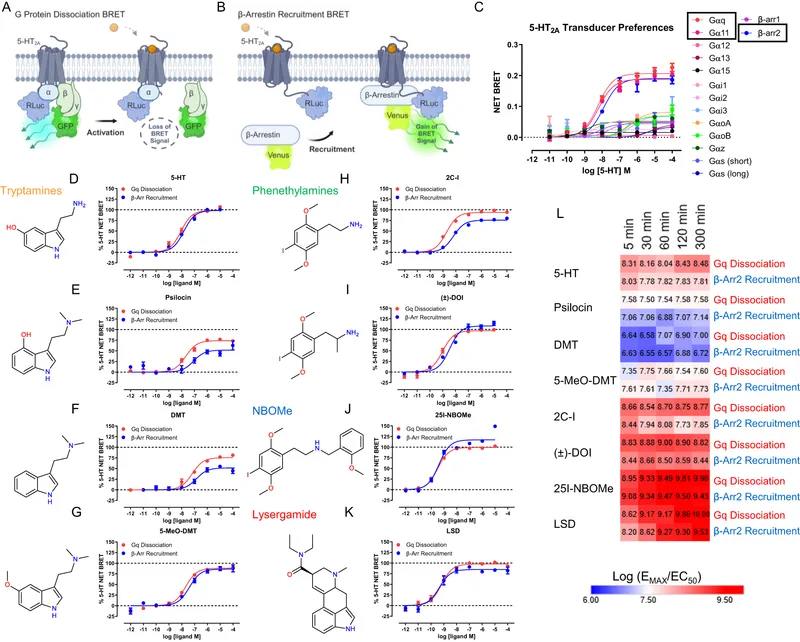
- Classical Hallucinogens (LSD, Psilocybin, Mescaline):
- Primarily act as agonists at serotonin 5-HT2A receptors.
- Also affect other 5-HT receptors (e.g., 5-HT1A, 5-HT2C).
- Leads to ↑glutamate release in prefrontal cortex (PFC).
⭐ Classical hallucinogens (LSD, psilocybin, mescaline) primarily act as agonists at serotonin 5-HT2A receptors.
- Dissociative Anesthetics (PCP, Ketamine):
- Non-competitive antagonists at NMDA glutamate receptors.
- Block glutamate action, leading to dissociative effects.
- May also interact with dopamine, opioid, and sigma receptors.
- Atypical Hallucinogens (e.g., Salvinorin A):
- Potent and selective agonist at kappa-opioid receptors.
- Unique mechanism, distinct from classical or dissociative types.
Clinical Features & Intoxication - Perceptual Kaleidoscope
-
General Intoxication Features:
- Perceptual Distortions: Vivid visual, auditory, tactile hallucinations; illusions; synesthesia (e.g., "seeing sounds"); distorted time/space perception.
- Mood & Thought: Marked anxiety or depression, panic ("bad trip"), euphoria, paranoia, grandiosity, depersonalization, derealization, impaired judgment.
- Somatic (Sympathomimetic): Mydriasis (dilated pupils), tachycardia, hypertension, hyperthermia, sweating, palpitations, tremors, incoordination, nausea.
-
Classic Hallucinogens (e.g., LSD, Psilocybin, Mescaline):
- Key: Predominantly perceptual changes, mood alteration.
- Physical: Significant mydriasis, ↑HR, ↑BP.
- "Good trip" (euphoria, mystical experiences) vs. "Bad trip" (intense anxiety, fear, psychosis-like state).
-
Dissociative Anesthetics (e.g., Phencyclidine [PCP], Ketamine):
- Key: Dissociation, analgesia, amnesia.
- Behavioral: Agitation, aggression, impulsivity, unpredictable violence, bizarre behavior, psychosis.
- Neurological: Nystagmus (vertical, horizontal, or rotatory - classic for PCP), ataxia, dysarthria, muscle rigidity, hyperacusis.
- Severe: Seizures, coma, rhabdomyolysis, respiratory depression.
⭐ Phencyclidine (PCP) intoxication is uniquely associated with nystagmus (rotatory, horizontal, or vertical) and aggressive, violent behavior.
Management & Specific Syndromes - Navigating the Trip
- General Mgmt:
- Supportive: Reassurance, "talk-down" technique, quiet, low-stimulus environment.
- Agitation/Anxiety: Benzodiazepines (e.g., Lorazepam, Diazepam).
- Severe Psychosis: If Benzodiazepines fail, consider antipsychotics (e.g., Haloperidol) cautiously.
- PCP Specifics:
- Key: Manage hyperthermia, rhabdomyolysis, seizures.
- Benzodiazepines for agitation/seizures. Avoid phenothiazines (↓seizure threshold).
- HPPD & Flashbacks:
- HPPD: Persistent perceptual disturbances post-cessation.
- Flashbacks: Episodic recurrences.
- Tx: Reassurance; Benzodiazepines, SSRIs if distressing.
⭐ Hallucinogen Persisting Perception Disorder (HPPD) involves re-experiencing perceptual distortions after cessation of use, without current intoxication.
High‑Yield Points - ⚡ Biggest Takeaways
- Hallucinogens (LSD, psilocybin) cause perceptual distortions, visual hallucinations, and synesthesia.
- PCP intoxication features nystagmus (rotatory/vertical), aggression, ataxia, and muscle rigidity.
- Hallucinogen Persisting Perception Disorder (HPPD) involves recurrent flashbacks of perceptual disturbances.
- Management is mainly supportive care; benzodiazepines for agitation or PCP-induced symptoms.
- Classic hallucinogens (LSD) typically lack a significant withdrawal syndrome; PCP may have one.
- PCP can cause severe complications like hypertension, hyperthermia, and rhabdomyolysis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

