Cannabis Use Disorder: Basics - Ganja Genesis
- Source: Cannabis sativa/indica plants.
- Active Compounds:
- $\Delta^9$-Tetrahydrocannabinol (THC): Psychoactive ("high").
- Cannabidiol (CBD): Non-psychoactive, therapeutic potential.
- Routes: Inhalation (smoking, vaping - rapid onset); Oral (bhang, edibles - slower onset, longer effect).
- Indian Context: Forms: ganja (flowers), charas (resin), bhang (leaves/seeds). High prevalence in young adults.
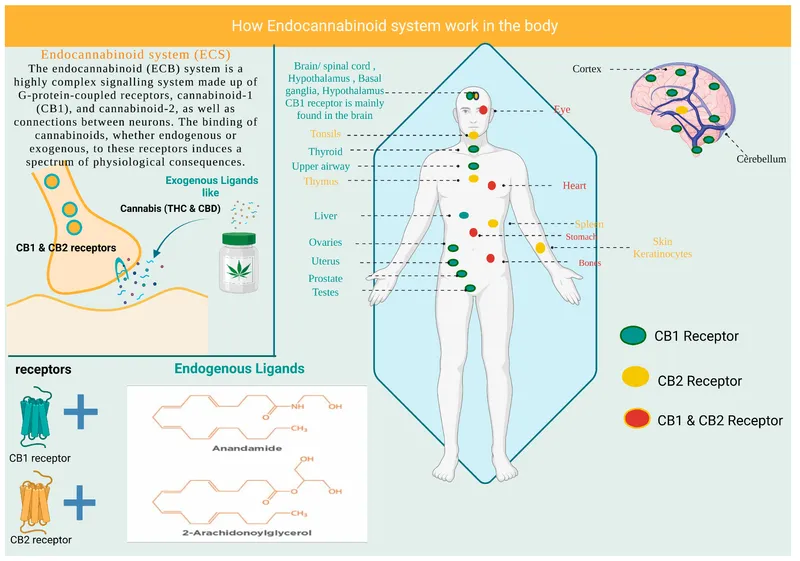
⭐ Key endocannabinoid system components include CB1 receptors (primarily in CNS) and CB2 receptors (periphery, immune cells), and endogenous ligands like anandamide and 2-arachidonoylglycerol (2-AG).
Cannabis Use Disorder: Neurobiology & Clinical Dx - High Times & Lows
- Neurobiology:
- THC (Δ⁹-tetrahydrocannabinol) binds CB1 (brain) & CB2 receptors; mimics endocannabinoid anandamide.
- Acute Intoxication ("High"):
- Euphoria, relaxation, altered perception (time, senses), ↑ appetite.
- Physical: Conjunctival injection, dry mouth, tachycardia.
- Adverse: Anxiety, paranoia, impaired coordination/memory.
- Withdrawal:
- (See ⭐ below for DSM-5 criteria details).
- Cannabis Use Disorder (CUD) - DSM-5:
- Problematic pattern: ≥2 criteria in 12 months.
- Categories: Impaired control, social impairment, risky use, pharmacological (tolerance, withdrawal).
- Severity: Mild (2-3), Moderate (4-5), Severe (≥6 symptoms).
⭐ Cannabis withdrawal (DSM-5 criteria: irritability, anxiety, sleep difficulty, decreased appetite, restlessness, depressed mood, plus physical symptoms like abdominal pain, shakiness/tremors, sweating, fever, chills, or headache) is a recognized syndrome that can significantly impair functioning.
Cannabis Use Disorder: Complications - Reefer Risks
- Respiratory System:
- Chronic bronchitis, cough, wheezing.
- ↑ Tar & carcinogens vs. tobacco (📌 "Tar Wars").
- Potential ↑ risk of lung cancer with long-term heavy use.
- Cardiovascular System:
- Acute: Tachycardia, ↑BP, orthostatic hypotension.
- Chronic: Possible ↑ risk of MI, stroke in susceptible individuals.
- Mental Health:
- ↑ Risk of anxiety, depression.
- Cannabis-induced psychotic disorder.
- Amotivational syndrome: Apathy, ↓ drive (debated).
- ⭐ > Early and heavy cannabis use in adolescence is associated with an increased risk of developing psychotic disorders, such as schizophrenia, and persistent cognitive deficits.
- Cognitive Impairment:
- Deficits in attention, memory, executive functions.
- Persistent effects possible, especially with early, heavy use.
- Other Complications:
- Cannabinoid Hyperemesis Syndrome (CHS): Cyclical nausea, vomiting, abdominal pain; relieved by hot showers.
- Dependence and withdrawal symptoms.
oka
Cannabis Use Disorder: Management - Kicking the Habit
- Goal: Abstinence or harm reduction.
- Initial Approach: Screening (e.g., ASSIST, CUDIT-R) & Brief Intervention (BI).
-
Psychosocial Therapies (First-line):
- Motivational Enhancement Therapy (MET): Explores ambivalence, enhances motivation to change.
- Cognitive Behavioral Therapy (CBT): Identifies triggers, develops coping skills.
- Contingency Management (CM): Reinforces abstinence with tangible rewards.
⭐ Psychosocial interventions, particularly Motivational Enhancement Therapy (MET), Cognitive Behavioral Therapy (CBT), and Contingency Management (CM), are the cornerstones of Cannabis Use Disorder treatment.
-
Pharmacotherapy:
- No FDA-approved medications specifically for CUD.
- Focus on treating co-occurring psychiatric disorders (e.g., depression, anxiety).
- Short-term anxiolytics/hypnotics for severe withdrawal (cautiously).
- N-acetylcysteine (NAC) & Gabapentin: Emerging evidence, not standard.
-
Special Populations:
- Adolescents: Family-based therapies, MET/CBT.
- Pregnant women: Psychosocial interventions are primary; avoid cannabis due to risks to fetus.
-
Relapse Prevention: Crucial component; ongoing support, coping strategies. 📌 HALT (Hungry, Angry, Lonely, Tired) as relapse triggers awareness.
High‑Yield Points - ⚡ Biggest Takeaways
- Cannabis Use Disorder (CUD): Problematic cannabis use causing significant impairment/distress.
- Key features: Tolerance, withdrawal, craving, and impaired control over use.
- Cannabis withdrawal: Irritability, anxiety, sleep issues, ↓appetite, restlessness.
- Amotivational syndrome: Associated with chronic heavy use, characterized by apathy and ↓ drive.
- Synthetic cannabinoids ("Spice", "K2"): Risk of severe, unpredictable effects, including psychosis.
- Treatment: Primarily psychosocial interventions (CBT, MET); limited role for pharmacotherapy.
- Risks: Respiratory issues (if smoked), potential trigger/worsening of psychotic disorders.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

