Parasomnias 101 - Sleep's Strange Acts
- Abnormal behaviors/experiences during sleep or sleep-wake transitions.
- Key Types:
- NREM-Related (Disorders of Arousal):
- Sleepwalking, Sleep Terrors, Confusional Arousals.
- Features: First 1/3 of night (N3 sleep), amnesia, hard to arouse.
- REM-Related:
- REM Sleep Behavior Disorder (RBD), Nightmare Disorder, Sleep Paralysis.
- Features: Latter half of night, dream recall.
- NREM-Related (Disorders of Arousal):
⭐ REM Sleep Behavior Disorder (RBD) often predates synucleinopathies (e.g., Parkinson's disease, Lewy body dementia).
NREM Parasomnias - Night's Unconscious Antics
- Arousal disorders from NREM stage N3 sleep (slow-wave); occur in the first ⅓ of the night.
- Key Features: Incomplete awakening, significant confusion, reduced responsiveness to stimuli, and subsequent amnesia for the event.
- Common Types:
- Confusional Arousals: Disorientation, slow speech, and impaired mentation upon partial awakening.
- Sleepwalking (Somnambulism): Complex motor behaviors (e.g., walking, eating) performed while asleep; risk of injury.
- Sleep Terrors (Pavor Nocturnus): Sudden arousal with intense fear, screaming, and autonomic hyperactivity (tachycardia, tachypnea, sweating); individual is typically inconsolable.
⭐ Adult-onset or persistent sleepwalking warrants investigation for underlying conditions like Obstructive Sleep Apnea (OSA) or psychiatric disorders.
- Common Triggers: Sleep deprivation, stress, fever, alcohol, certain medications (e.g., zolpidem, SSRIs, antipsychotics).
- Management: Primarily reassurance, ensuring a safe environment (e.g., removing hazards), and managing identifiable triggers. Clonazepam may be considered for severe, frequent, or dangerous episodes. )
REM Parasomnias - Dreamtime Disturbances
- REM Sleep Behavior Disorder (RBD)
- Complex motor behaviors during REM, enacting dreams (often violent).
- Due to loss of normal REM sleep atonia.
- Polysomnography (PSG) confirms: REM sleep without atonia (RSWA).
- Strong prodromal marker for α-synucleinopathies (Parkinson's, Lewy Body Dementia, MSA).
- Rx: Clonazepam (low dose), Melatonin.
- Nightmare Disorder
- Recurrent, extended, extremely dysphoric, well-recalled dreams.
- Usually occur during the second half of the sleep period.
- Rapidly alert and oriented upon awakening; causes significant distress/impairment.
- Recurrent Isolated Sleep Paralysis
- Inability to perform voluntary movements at sleep onset (hypnagogic) or upon awakening (hypnopompic).
- Consciousness and recall intact; often associated with vivid hallucinations (hypnagogic/hypnopompic).
⭐ RBD has a high conversion rate (over 80% in 10-15 years) to a defined neurodegenerative disease, primarily α-synucleinopathies.
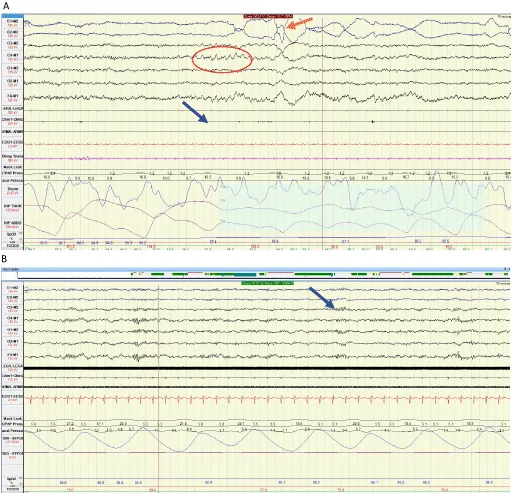
Other Parasomnias & Approach - Oddities & Order
-
Uncommon Parasomnias:
- Exploding Head Syndrome: Abrupt, loud imagined noise/flash on sleep-wake transitions; benign.
- Sleep Groaning (Catathrenia): Monotonous groaning during expiration, mainly in REM; partner reports.
- Sleep Paralysis: Transient atonia at sleep onset/offset; often with vivid hallucinations.
-
Nightmare Disorder: Recurrent, highly dysphoric, well-recalled dreams, typically in late REM. Tx: Imagery Rehearsal Therapy (IRT), Prazosin.
-
Diagnostic & Management Flow:
-
Core Management: Education, reassurance, robust sleep hygiene, ensuring environmental safety. Address comorbid conditions.
-
Pharmacotherapy (if severe/frequent):
- NREM Parasomnias/RBD: Clonazepam (0.5-2 mg hs).
- RBD: Melatonin.
⭐ Video-Polysomnography (V-PSG) is crucial for differentiating parasomnias from nocturnal seizures and confirming REM Sleep Behavior Disorder, especially with injury risk.
High‑Yield Points - ⚡ Biggest Takeaways
- NREM Parasomnias (Sleepwalking, Sleep Terrors): Occur in N3 sleep (first third of night), amnesia for event.
- REM Sleep Behavior Disorder (RBD): Dream-enacting behaviors during REM sleep (latter half), linked to α-synucleinopathies (e.g., Parkinson's).
- Nightmare Disorder: Frightening dreams during REM sleep (latter half), full recall on awakening.
- Key distinction: NREM disorders = amnesia; REM disorders (RBD, Nightmares) = dream recall.
- Clonazepam is effective for RBD; NREM disorders often require only safety measures and reassurance_._
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

