Definition & Epidemiology - Counting Sheep No More
- Insomnia: Difficulty initiating/maintaining sleep (DIS/DMS), early morning awakening (EMA), or non-restorative sleep, despite adequate opportunity.
- Causes clinically significant distress/impairment.
- Key Criteria:
- Frequency: ≥3 nights/week.
- Duration: ≥3 months (Chronic).
- Episodic: ≥1 to <3 months.
- Epidemiology:
- Prevalence: Symptoms 10-30%; Disorder 6-10%.
- ↑ women, older adults, comorbid conditions.
⭐ Insomnia is a significant risk factor for depression & anxiety disorders.
Etiology & Pathophysiology - Why So Awake?
- Spielman's 3-P Model:
- Predisposing factors: Hyperarousal (cognitive/physiological), genetic predisposition, anxious personality traits.
- Precipitating factors: Acute stressors (medical/psychiatric illness, life events), substances (caffeine, alcohol), medications (e.g., steroids).
- Perpetuating factors: Poor sleep hygiene, maladaptive behaviors (e.g., napping, ↑ time in bed), conditioned arousal to bedroom.
- Neurobiological Factors:
- ↑ Wake-promoting systems: Orexin/hypocretin, glutamate, cortisol (HPA axis dysregulation).
- ↓ Sleep-promoting systems: GABAergic inhibition, altered melatonin secretion rhythm.
- Brain: Hyperactivity in arousal circuits (e.g., Reticular Activating System, amygdala, prefrontal cortex).
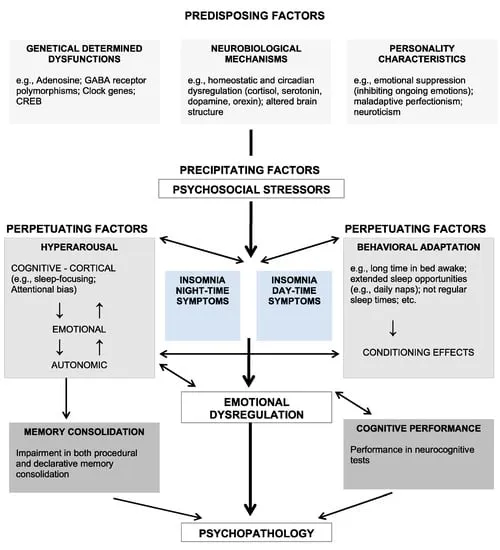
⭐ Insomnia is characterized by physiological and cognitive hyperarousal, not just at night but often persisting during the day, increasing comorbidity risks with mood and anxiety disorders.
Clinical Features & Diagnosis - Pinpointing the Problem
-
Core Features: Difficulty initiating/maintaining sleep, or early morning awakening with inability to return to sleep.
-
Occurs despite adequate opportunity for sleep.
-
Causes clinically significant distress/impairment (social, occupational).
-
Diagnostic Criteria (DSM-5 Summary):
- Sleep difficulty ≥ 3 nights/week for ≥ 3 months.
- Not better explained by another sleep-wake disorder.
- Not attributable to substance effects (drug of abuse, medication).
- Coexisting mental/medical conditions don't adequately explain predominant complaint of insomnia.
⭐ Key Diagnostic Tool: Sleep diary (at least 2 weeks) is crucial for assessing sleep patterns and variability before polysomnography consideration if diagnosis is uncertain or comorbid sleep disorders suspected (e.g., OSA, PLMD).
Non-Pharmacological Management - Mind Over Mattress
- Cognitive Behavioral Therapy for Insomnia (CBT-I): First-line treatment.
- Sleep Hygiene: Consistent sleep-wake schedule; avoid stimulants (caffeine, nicotine) & alcohol near bedtime; cool, dark, quiet room; limit naps (≤ 30 min).
- Stimulus Control: Bed for sleep/sex only; leave bed if not asleep in 20 min, return when sleepy; fixed wake time.
- Sleep Restriction: Limit time in bed to actual sleep time, then gradually increase as sleep efficiency improves (> 85%).
- Relaxation Training: Progressive muscle relaxation, deep breathing, mindfulness.
- Cognitive Therapy: Challenge dysfunctional beliefs about sleep.

⭐ CBT-I is considered the gold standard and first-line treatment for chronic insomnia, often demonstrating superior long-term efficacy compared to pharmacotherapy alone.
Pharmacological Management - Pills for Peace
- Indication: Short-term for moderate-severe insomnia; ideally alongside CBT-I.
- Benzodiazepines (BZDs): e.g., Lorazepam. Rapid onset. Risks: tolerance, dependence, withdrawal. Use for <4 weeks.
- Non-BZDs (Z-drugs): Zolpidem, Zaleplon, Eszopiclone. Better safety than BZDs but risk of complex sleep behaviors.
- Melatonin Receptor Agonists: Ramelteon. Good for sleep-onset insomnia; no abuse potential.
- Orexin Receptor Antagonists: Suvorexant, Lemborexant. Target wakefulness system.
- Low-dose Sedating Antidepressants: Doxepin, Trazodone, Mirtazapine.
⭐ Z-drugs (Zolpidem, Zaleplon, Eszopiclone) selectively bind to α1 subunit of GABA-A receptor, leading to fewer anxiolytic/myorelaxant effects than BZDs.
High‑Yield Points - ⚡ Biggest Takeaways
- Diagnosis: Sleep difficulty (initiation/maintenance/early awakening) ≥3 nights/week for ≥3 months, causing distress/impairment.
- First-line Treatment: Cognitive Behavioral Therapy for Insomnia (CBT-I) is superior.
- Pharmacotherapy: Short-term Z-drugs (Zolpidem) or short-acting BZDs; consider DORAs.
- Sleep Hygiene: Key in CBT-I, but often insufficient alone.
- Polysomnography (PSG): Not routine; for suspected comorbid sleep disorders.
- Comorbidities: High with psychiatric (depression, anxiety) and medical conditions.
- Risks: ↑ accidents, mood disorders, cardiovascular disease.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

