Antipsychotics: The Basics - Brain Balancers
-
Cornerstone of schizophrenia treatment.
-
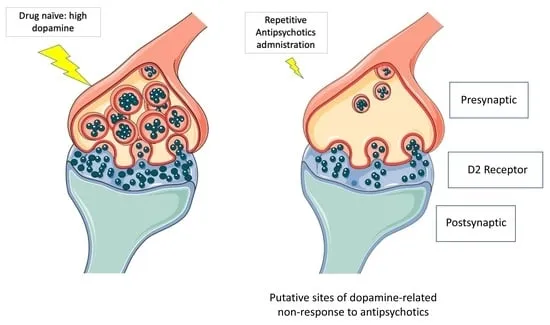
Mechanism: Primarily modulate dopamine pathways; most are $D_2$ receptor antagonists.
-
Classification:
-
FGAs (1st Gen): Effective for positive symptoms (hallucinations, delusions). Risk of Extrapyramidal Symptoms (EPS).
-
SGAs (2nd Gen): Broader efficacy, including some negative symptoms. Lower EPS risk, but higher risk of metabolic side effects (weight gain, diabetes).
-
-
⭐ All antipsychotics require 60-80% $D_2$ receptor occupancy for optimal efficacy; higher occupancy increases EPS risk without improving efficacy.
FGAs: Side Effect Profiles - Classic Dopamine Blockers
- Mechanism: $D_2$ receptor blockade.
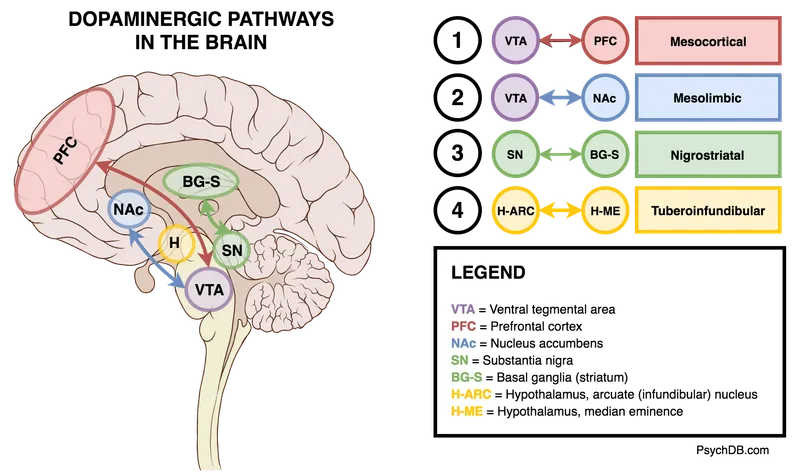
- Extrapyramidal Symptoms (EPS): Nigrostriatal $D_2$ block.
- Acute Dystonia: Spasms, torticollis. Tx: Anticholinergics.
- Akathisia: Restlessness. Tx: $\beta$-blockers, Benzodiazepines (BZDs).
- Parkinsonism: Tremor, rigidity, bradykinesia. Tx: Anticholinergics.
- Tardive Dyskinesia (TD): Orofacial dyskinesia. Often irreversible. 📌 TD: Time Dependent.
- Neuroleptic Malignant Syndrome (NMS):
- FEVER: Fever, Encephalopathy, Vitals unstable, Enzymes $\uparrow$ (CK), Rigidity.
- Tx: Stop FGA, Dantrolene, Bromocriptine.
- Hyperprolactinemia: Tuberoinfundibular $D_2$ block.
- Galactorrhea, amenorrhea, gynecomastia, sexual dysfunction.
- Other Side Effects (Potency-dependent):
- Low Potency (e.g., Chlorpromazine): $\uparrow$Anticholinergic, $\uparrow$Sedation (H1 block), $\uparrow$Orthostatic Hypotension ($\alpha_1$ block).
- High Potency (e.g., Haloperidol): $\uparrow$EPS, $\downarrow$Sedation/Hypotension/Anticholinergic effects.
⭐ NMS is a medical emergency: fever, muscle rigidity, autonomic dysfunction, altered mental status; requires immediate FGA discontinuation and supportive care.
 oka
oka
SGAs: Metabolic Concerns - Modern Mind Menders
- SGAs (Atypical Antipsychotics): D2 & 5-HT2A antagonists.
- Benefits: ↓EPS, better for negative symptoms vs FGAs.
- Key Issue: Metabolic Syndrome (MetS) - ↑Weight/BMI, ↑Waist, Dyslipidemia (↑TG, ↓HDL), ↑BP, ↑FBG.
- Metabolic Risk Profile:
- High: Clozapine, Olanzapine (📌 Old Clothes = fat & sleepy)
- Moderate: Risperidone, Quetiapine, Paliperidone
- Low/Neutral: Aripiprazole, Ziprasidone, Lurasidone (📌 A Zippy Lura = Atypical & Lean)
- Monitoring: Essential!
- Baseline & regular: Weight, BMI, Waist, BP, FPG, Lipids.
- ⚠️ FPG ≥ 126 mg/dL (Diabetes), TG ≥ 150 mg/dL.
- Management: Lifestyle modification, switch SGA, consider Metformin.
⭐ Clozapine and Olanzapine have the highest propensity for inducing significant weight gain and new-onset diabetes.
TRS & Clozapine - Strategy & Special Ops
- TRS Definition: Failure of ≥2 antipsychotics (≥1 atypical) at adequate dose & duration (e.g., 6-8 weeks).
- Clozapine Strategy:
- The ONLY proven drug for TRS; also for persistent suicidality, severe TD.
- Dosing: Start 12.5-25 mg/day, titrate slowly to 300-600 mg/day (max 900 mg).
- ⚠️ Critical Monitoring "AMC-S":
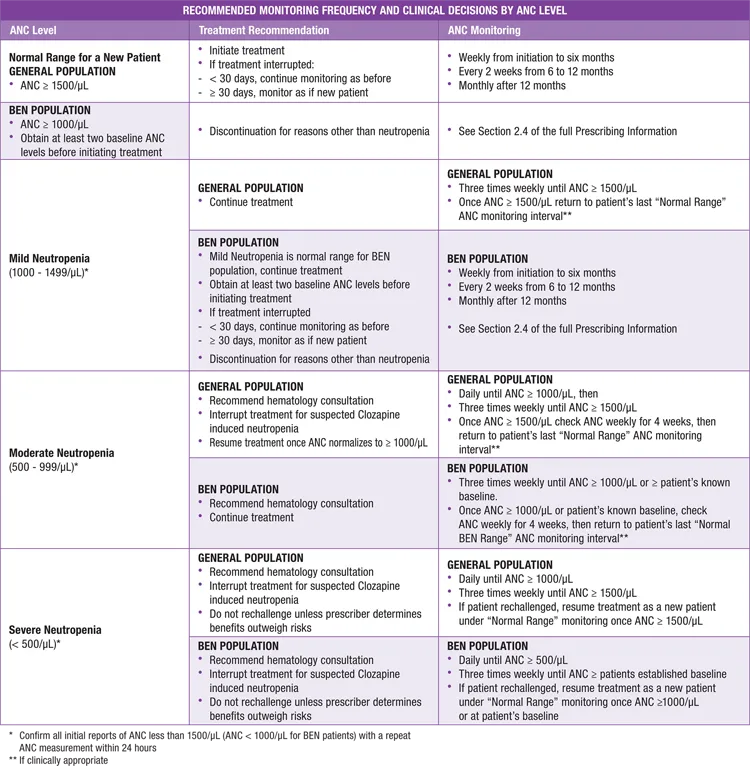
- Agranulocytosis: ANC weekly (18wks) → bi-weekly (18wks) → monthly.
- Stop: ANC < 1000/µL (or < 500/µL in BEN).
- Interrupt: ANC 1000-1500/µL.
- Myocarditis/Cardiomyopathy: Baseline & monitor ECG, troponin, CRP.
- Constipation (severe).
- Seizures (dose-dependent).
- Agranulocytosis: ANC weekly (18wks) → bi-weekly (18wks) → monthly.
- Other SEs: Hypersalivation, weight gain, sedation.
- Augmentation (if Clozapine partial response): ECT, lamotrigine, another AP (cautiously).
- Long-Term Strategy:
- LAIs: Consider for adherence post-stabilization.
- Psychosocial therapies (CBTp, family therapy): Essential adjunct.
⭐ Clozapine requires mandatory blood monitoring (ANC) due to potentially fatal agranulocytosis risk.
High‑Yield Points - ⚡ Biggest Takeaways
- Antipsychotics are the cornerstone of schizophrenia management.
- Second-Generation Antipsychotics (SGAs) are typically first-line due to better tolerability (fewer EPS).
- Clozapine is uniquely effective for Treatment-Resistant Schizophrenia (TRS).
- Regular WBC monitoring is mandatory with Clozapine due to agranulocytosis risk.
- Long-Acting Injectable (LAI) antipsychotics significantly improve treatment adherence.
- Psychosocial interventions, like CBT and family therapy, are crucial adjuncts.
- ECT is a valuable option for catatonia, severe suicidality, or resistant cases.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

