Definition & Core Concepts - The Hybrid Puzzle
- Chronic illness: Combines schizophrenia & mood disorder symptoms.
- "Hybrid": Psychotic (hallucinations, delusions) + Mood (mania, depression) features.
- Crucial: Psychosis for ≥2 weeks without major mood episode.
- Mood symptoms prominent for substantial illness duration.
- Subtypes: Bipolar type (mania); Depressive type (depression only).
⭐ Delusions or hallucinations for 2 or more weeks in the absence of a major mood episode is crucial for differentiating from mood disorder with psychotic features.
Clinical Features & Types - Mood Meets Psychosis
- Core: Major mood episode (depressive/manic) concurrent with Schizophrenia's Criterion A symptoms.
- Key: Delusions or hallucinations for ≥2 weeks without major mood symptoms during lifetime illness.
- Differentiates from mood disorder with psychotic features.
- Types (based on mood component):
- Bipolar Type: Manic episode present (MDEs may occur).
- Depressive Type: Only MDEs feature.
- Symptoms:
- Mood: Depressive (anhedonia, low energy) or Manic (grandiosity, pressured speech).
- Psychotic: Delusions, hallucinations, disorganized speech, negative symptoms.
- Causes significant functional impairment.
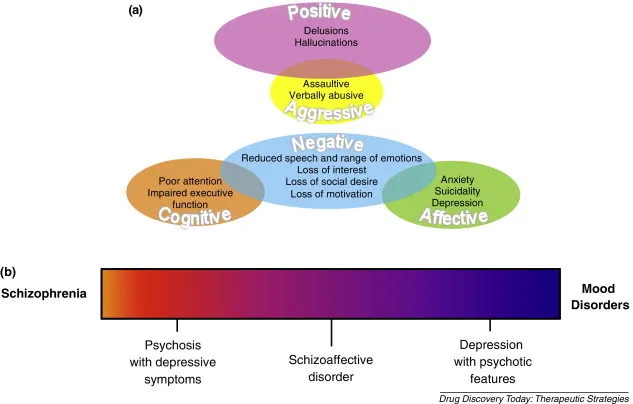
⭐ Delusions/hallucinations for ≥2 weeks without a major mood episode is diagnostically vital.
Diagnostic Criteria (DSM-5) - The DSM-5 Blueprint
- A: Uninterrupted illness: Major Mood Episode (MME: depressive/manic) concurrent with Schizophrenia's Criterion A symptoms (e.g., delusions, hallucinations).
- B: Delusions or hallucinations for ≥2 weeks without MME symptoms during illness lifetime. Key differentiator.
- C: MME symptoms present for majority of total illness duration (active & residual phases).
- D: Not due to substance effects or another medical condition.
- Types:
- Bipolar Type: Manic episode present (depressive episodes may also occur).
- Depressive Type: Only major depressive episodes present.
⭐ Criterion B: Psychosis for ≥2 weeks without mood symptoms is essential to distinguish from Mood Disorder with Psychotic Features.
Differential Diagnosis - Similar Yet Distinct
| Feature | Schizoaffective Disorder | Schizophrenia | Mood Disorder w/ Psychotic Features |
|---|---|---|---|
| Psychosis & Mood | Psychosis with & without mood episodes | Psychosis primary; mood sx brief/absent | Psychosis only during mood episodes |
| Mood Duration | Substantial part of illness | Brief relative to psychosis | Defines illness episodes |
| Psychosis sans Mood | Yes (delusions/hallucinations ≥2 wks) | Yes (core feature) | No |
Management & Prognosis - Charting The Course
- Pharmacotherapy (Tailor to symptoms):
- Antipsychotics: Second-Generation Antipsychotics (SGAs) (e.g., paliperidone) are first-line. Clozapine for treatment-resistance.
- Mood Stabilizers: Valproate, lithium, lamotrigine (especially for bipolar type).
- Antidepressants: SSRIs with an antipsychotic for depressive episodes (use cautiously).
- Non-Pharmacological:
- Psychotherapy: Individual, group, family therapy.
- Social skills training; vocational rehabilitation.
- ECT: Effective for severe mood symptoms or catatonia.
- Prognosis:
- Course is variable.
- Generally better than schizophrenia, worse than primary mood disorders.
- Good factors: Acute onset, good premorbid function, prominent mood symptoms.
⭐ Prognosis is generally intermediate: better than schizophrenia, worse than mood disorders.
High-Yield Points - ⚡ Biggest Takeaways
- Schizoaffective disorder: A hybrid of schizophrenia and mood disorder (depressive/bipolar).
- Key criterion: Psychotic symptoms (delusions/hallucinations) for ≥2 weeks without prominent mood symptoms.
- Mood symptoms are present for a significant portion of the total illness duration.
- Two subtypes: Bipolar type (mania or mixed episodes present) and Depressive type (only major depression).
- Prognosis: Generally intermediate between schizophrenia and pure mood disorders.
- Treatment: Antipsychotics are core; add mood stabilizers (bipolar type) or antidepressants (depressive type).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

