PK vs PD Fundamentals - Drug's Journey & Impact
- Pharmacokinetics (PK): Body's action on drug. "What the body does to the drug."
- 📌 ADME: Absorption, Distribution, Metabolism, Excretion.
- Key parameters: Bioavailability (F), Volume of distribution ($V_d$), Clearance (CL), Half-life ($t_{1/2}$).
- Pharmacodynamics (PD): Drug's action on body. "What the drug does to the body."
- Receptor interactions: Agonists, antagonists.
- Dose-Response: Efficacy ($E_{max}$), Potency ($ED_{50}$).

⭐ First-pass metabolism significantly reduces the bioavailability of orally administered drugs like lignocaine or propranolol.
Pharmacokinetics (ADME) - Body's Drug Maze
📌 ADME: Absorption, Distribution, Metabolism, Excretion.
- Absorption: Drug movement from administration site to bloodstream.
- Bioavailability (F): Fraction reaching circulation. $F = \text{AUC}\text{oral} / \text{AUC}\text{IV}$. IV $F = \mathbf{100}%$.
- First-pass metabolism (liver) ↓ F for oral drugs.
- Distribution: Reversible transfer of drug from blood to tissues/organs.
- Volume of Distribution ($V_d$): $V_d = \text{Dose} / C_0$.
- Influenced by lipid solubility, protein binding.
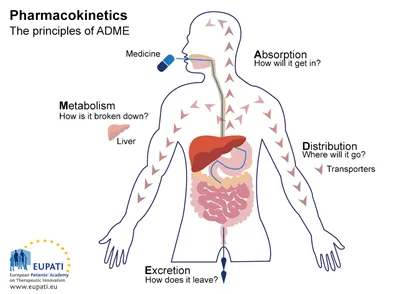
- Metabolism: Chemical alteration of drug, primarily by liver enzymes (CYP450).
- Phase I (oxidation, etc.), Phase II (conjugation).
- Enzyme induction/inhibition → drug interactions.
- Excretion: Elimination of drug/metabolites, mainly via kidneys.
- Clearance (CL): $CL = k \cdot V_d$.
- Half-life ($t_{1/2}$): $t_{1/2} = 0.693 / k$. Steady state in 4-5 $t_{1/2}$.
⭐ Most psychotropic drugs are lipid-soluble, leading to a large volume of distribution ($V_d$) and ability to cross the blood-brain barrier.
Pharmacodynamics (Mechanisms) - Drug's Power Play
- What drug does to body; mechanism of action (MoA).
- Receptor Interactions:
- Agonist: Activates receptor.
- Full: Max response.
- Partial: Submaximal; can act as antagonist with full agonist.
- Inverse: Opposite effect to agonist (e.g., some antihistamines on H1 receptors).
- Antagonist: Blocks receptor action; no intrinsic activity.
- Competitive: Reversible; shifts Dose-Response (DR) curve right (↓Potency, $E_{max}$ same). Overcome by ↑agonist.
- Non-competitive: Irreversible or allosteric; ↓$E_{max}$. Cannot be overcome.
- Agonist: Activates receptor.
- Dose-Response Relationship:
- Potency: Drug amount for a given effect ($ED_{50}$ or $EC_{50}$); ↓$ED_{50}$ = ↑Potency.
- Efficacy: Max effect a drug can produce ($E_{max}$).
- Therapeutic Index (TI): Measure of drug safety. $TI = TD_{50}/ED_{50}$. Higher TI = safer drug.
- 📌 Lithium, Warfarin, Digoxin, Theophylline (Low TI Drugs - "Low Warning Dose Threshold").
- Receptor Regulation:
- Downregulation (Desensitization/Tachyphylaxis): ↓Receptor number/sensitivity with chronic agonist use.
- Upregulation (Supersensitivity): ↑Receptor number/sensitivity with chronic antagonist use.
⭐ Most antipsychotics exert their primary therapeutic effect by blocking Dopamine D2 receptors.

Clinical Applications & TDM - Minds & Meds
- Therapeutic Drug Monitoring (TDM): Optimizes dosing, ↑ efficacy, ↓ toxicity.
- Indications: Narrow therapeutic index (NTI), non-response, toxicity, interactions.
- Key Drugs (Trough Levels):
- Lithium: 0.6-1.2 mEq/L (Acute: up to 1.5). Toxic >1.5 mEq/L.
- Clozapine: >350 ng/mL (efficacy).
- Nortriptyline: 50-150 ng/mL.
- Valproate: 50-100 µg/mL.
- Carbamazepine: 4-12 µg/mL.
- Drug Interactions (CYP450):
- Inducers: Carbamazepine, Phenytoin, Rifampicin, Smoking, St. John's Wort → ↓ drug levels.
- Inhibitors: Valproate, Fluoxetine, Paroxetine, Cimetidine, Erythromycin → ↑ drug levels.
- Special Populations:
- Elderly: ↓ clearance. "Start low, go slow."
- Pregnancy: Risk-benefit (e.g., Valproate - NTDs).
⭐ Carbamazepine is a potent auto-inducer, accelerating its own metabolism, often requiring upward dose titration.
High‑Yield Points - ⚡ Biggest Takeaways
- CYP450 enzymes (e.g., 2D6, 3A4) critically mediate psychotropic metabolism; inducers ↓ levels, inhibitors ↑ levels.
- TDM is essential for drugs like lithium and TCAs due to narrow therapeutic windows.
- Drug half-life (t½) determines dosing interval and time to steady state (approx. 4-5 half-lives).
- Antipsychotic D2 receptor occupancy target: >65% for efficacy, >80% increases EPS risk.
- Pharmacodynamic mechanisms: agonism, antagonism, partial agonism define drug actions.
- First-pass metabolism significantly impacts oral drug bioavailability.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

