Neuroimaging in Clinical Assessment - Brain Blueprints
Structural neuroimaging visualizes brain anatomy; key for ruling out organic causes.
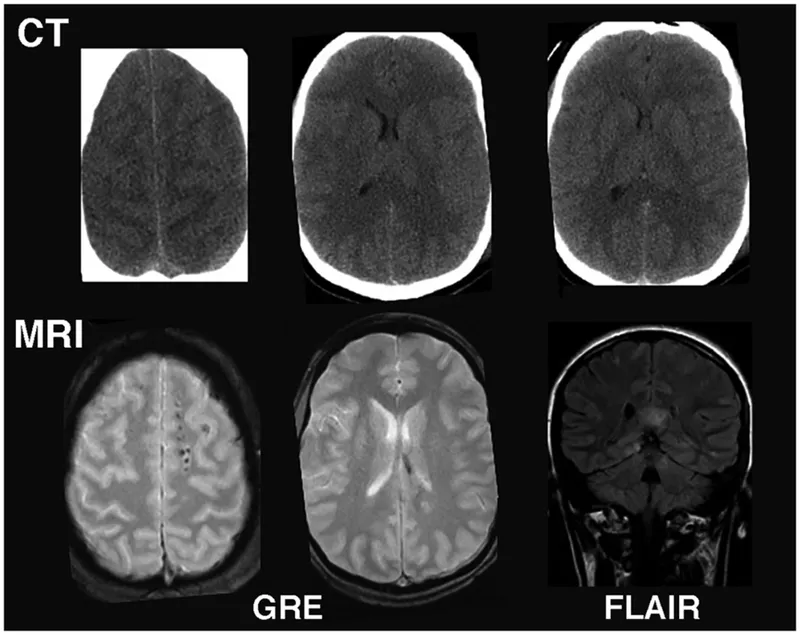
- Computed Tomography (CT)
- Principle: X-ray based; measures tissue density.
- Indications: Acute head trauma, suspected intracranial bleed, stroke.
- Pros: Fast, accessible.
- Cons: Radiation, less soft tissue detail than MRI.
- Magnetic Resonance Imaging (MRI)
- Principle: Magnetic fields & radio waves.
- Indications: Detailed soft tissue, white/gray matter lesions.
- Pros: Superior detail, no radiation.
- Cons: Slower, costlier, metal contraindications.
- Key Sequences:
- T1-weighted: Anatomy (CSF dark). 📌 T1: Anatomy.
- T2-weighted: Pathology (CSF bright). 📌 T2: H2O bright.
- FLAIR: T2-like, CSF dark; highlights periventricular lesions (e.g., MS).
⭐ MRI is superior to CT for detecting subtle structural brain abnormalities, white matter lesions (e.g., multiple sclerosis), and early ischemic changes.
 oka
oka
Neuroimaging in Clinical Assessment - Mind at Work
Functional neuroimaging provides dynamic insights into brain activity, blood flow, and neurochemistry.
- Functional MRI (fMRI):
- Measures brain activity by detecting changes in blood oxygenation (BOLD signal).
- Non-invasive, no radiation. High spatial, moderate temporal resolution.
- Uses: Cognitive research, mapping eloquent cortex pre-surgery.
- Positron Emission Tomography (PET):
- Visualizes metabolic processes (e.g., FDG for glucose metabolism) or receptor binding using radiolabeled tracers.
- Involves ionizing radiation.
- Uses: Alzheimer's (hypometabolism), Parkinson's (dopamine), oncology.
⭐ PET with 18F-FDG often reveals characteristic bilateral temporoparietal hypometabolism in Alzheimer's disease.
- Single Photon Emission CT (SPECT):
- Measures regional cerebral blood flow (rCBF) or neurotransmitter receptor availability.
- Uses gamma-emitting radiotracers; less resolution and sensitivity than PET.
- Uses: Dementia (perfusion), epilepsy (ictal vs. interictal), cerebrovascular disease.
- Magnetic Resonance Spectroscopy (MRS):
- Detects and quantifies brain metabolites (e.g., N-acetylaspartate (NAA), choline, creatine, lactate).
- Non-invasive; provides biochemical information.
- Uses: Differentiating tumor types, metabolic encephalopathies, research in mood disorders.

Neuroimaging in Clinical Assessment - Disorder Snapshots
- Schizophrenia: ↑ Ventricular size (lateral, third); ↓ cortical volume (frontal, temporal); hypofrontality (DLPFC).
- Major Depressive Disorder (MDD): ↓ Hippocampal volume; ↑ amygdala activity (negative stimuli); ↓ DLPFC activity (cognitive tasks).
- Bipolar Disorder: ↑ White matter hyperintensities; ↓ prefrontal cortex volume; altered amygdala-prefrontal connectivity.
- Obsessive-Compulsive Disorder (OCD): Orbitofrontal cortex (OFC), anterior cingulate cortex (ACC), striatal (caudate) abnormalities; functional: ↑ Cortico-Striato-Thalamo-Cortical (CSTC) loop hyperactivity.
- Post-Traumatic Stress Disorder (PTSD): ↓ Hippocampal & ACC volume; ↑ amygdala reactivity (trauma cues); ↓ medial prefrontal cortex (mPFC) activation.
- Alzheimer's Disease: Medial temporal lobe atrophy (hippocampus, entorhinal cortex); ↓ temporoparietal glucose metabolism (FDG-PET).
- ADHD: ↓ Volume: prefrontal cortex, basal ganglia, cerebellum; hypoactivation in frontostriatal networks.
⭐ Ventricular enlargement (lateral ventricles) is a consistent structural MRI finding in schizophrenia.
Neuroimaging in Clinical Assessment - Lens Limitations
- Supportive, Not Definitive: Rules out organic causes; not diagnostic for most psychiatric disorders.
- Low Specificity/Sensitivity: For primary psychiatric conditions, limiting individual diagnostic use.
- Incidental Findings: Can create anxiety, necessitate further costly investigations.
- Cost & Access: Significant barriers to routine clinical application.
- Research-Clinical Gap: Group findings often not applicable to individual patients.
⭐ Key role: Exclude organic mimics (e.g., tumor, stroke) in atypical psychiatric symptoms via CT/MRI.
- Interpretation Variability: Subjectivity can impact reliability.
High‑Yield Points - ⚡ Biggest Takeaways
- Structural neuroimaging (CT, MRI) primarily rules out organic causes of psychiatric symptoms.
- MRI offers superior soft-tissue contrast over CT for detecting subtle brain changes.
- Functional neuroimaging (fMRI, PET, SPECT) remains largely a research tool, not for routine psychiatric diagnosis.
- SPECT/PET can visualize cerebral blood flow, metabolism, or neuroreceptor occupancy.
- No pathognomonic neuroimaging findings exist for most primary psychiatric illnesses like schizophrenia or bipolar disorder.
- Hippocampal atrophy on MRI may be associated with chronic depression or Alzheimer's disease.
- Ventricular enlargement and cortical atrophy are non-specific findings sometimes observed in schizophrenia cases.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

