Definition & Epidemiology - Hair Havoc
- Definition: Recurrent pulling out of one's own hair, leading to hair loss.
- Accompanied by repeated attempts to ↓ or stop hair pulling.
- Causes clinically significant distress or impairment.
- Not attributable to another medical condition (e.g., dermatological).
- Not better explained by another mental disorder (e.g., body dysmorphic disorder).
- Prevalence: 12-month prevalence in adults & adolescents is 1-2%.
- Age of Onset: Commonly coincides with or follows puberty.
- Gender: Females are more frequently affected than males (approx. 10:1 ratio).
⭐ Exam Favourite: Trichotillomania is classified under Obsessive-Compulsive and Related Disorders in DSM-5, not as an impulse control disorder as in ICD-10 (F63.3).
Clinical Features - Telltale Tufts
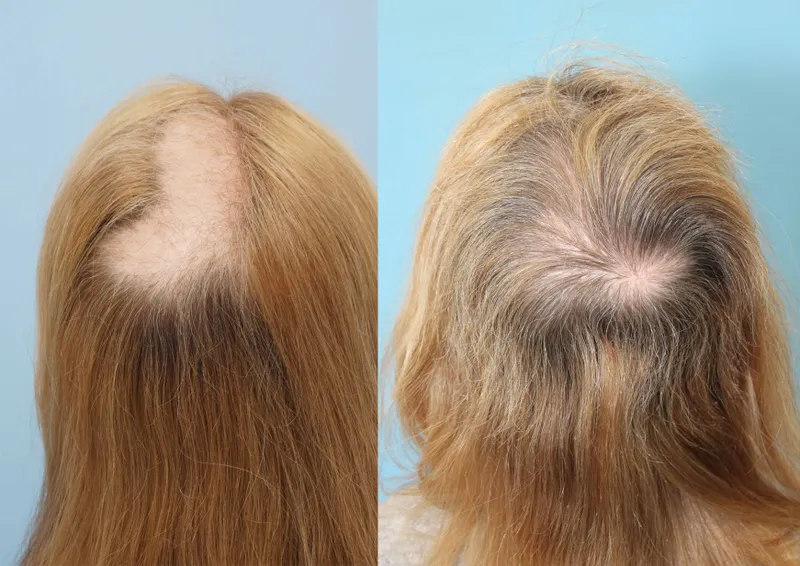
- Hair Loss Pattern:
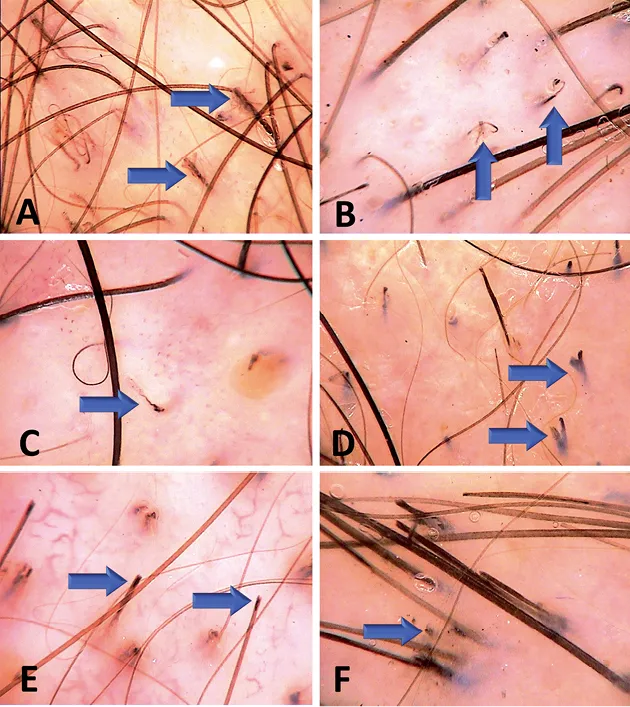
- Irregular, patchy alopecia; hairs of varying lengths (key diagnostic feature).
- Broken hairs (blunt/tapered ends); "telltale tufts" of short, stubbly hair.
- 📌 "Friar Tuck" sign: characteristic peripheral scalp sparing.
- Common Sites: Scalp (vertex/crown), eyebrows, eyelashes. Less frequent: axillary, pubic, beard.
- Associated Behaviors:
- Rituals: inspecting root, twirling, mouthing; trichophagia (~20%), risk of trichobezoar.
- Pulling: focused (tension relief) or automatic (unaware, e.g., reading).
- Skin Findings: Typically non-scarring. Erythema, excoriations, black dots (broken hairs).
⭐ Hairs of varying lengths in alopecia patches distinguish TTM from alopecia areata (smooth patches, exclamation mark hairs).
Diagnosis & DDx - Spotting Signs
DSM-5 Based Diagnosis (📌 H.A.I.R.S.):
- Hair pulling: Recurrent, resulting in hair loss.
- Attempts: Repeated efforts to decrease/stop pulling.
- Impairment: Clinically significant distress or functional impairment.
- Ruled out: Not due to other medical conditions (e.g., dermatological).
- Separate: Not better explained by another mental disorder (e.g., BDD, OCD).
Key Differentiators (DDx):
- Alopecia Areata: Autoimmune; smooth patches; "!" hairs.
- Tinea Capitis: Fungal; scaling, black dots, broken hairs; +KOH.
- OCD: Pulling ritualistic, secondary to unrelated obsession/symmetry; not for tension relief.
- BDD: Hair removal to "fix" perceived appearance defect.
⭐ Trichobezoars (hairballs) from ingesting pulled hair can cause serious GI complications like obstruction.
Treatment Approaches - Taming Urges
- Primary Goal: Reduce hair pulling, manage urges, improve psychosocial functioning.
- First-line Therapy: Behavioral Interventions
- Habit Reversal Training (HRT): Core component; involves awareness training & competing response.
- Cognitive Behavioral Therapy (CBT): Addresses dysfunctional thoughts & beliefs.
- Acceptance and Commitment Therapy (ACT).
- Pharmacotherapy: Adjunctive or for severe/refractory cases.
- SSRIs (e.g., Fluoxetine, Sertraline): Often initial choice, variable efficacy.
- Clomipramine (TCA): Strongest evidence; dose 25-250 mg/day. Monitor side effects.
- N-acetylcysteine (NAC): Glutamate modulator; dose 1200-2400 mg/day.
- Atypical Antipsychotics (e.g., Olanzapine, Risperidone): Low dose for refractory cases.
⭐ Clomipramine has demonstrated the most robust efficacy among pharmacological agents for trichotillomania in clinical trials, though often reserved due to its side effect profile compared to SSRIs or NAC.
Comorbidities & Complications - Tangled Troubles
- Psychiatric:
- MDD (Major Depressive Disorder)
- Anxiety disorders (esp. GAD, Social Anxiety)
- OCD
- Excoriation (skin-picking) disorder
- Substance use disorders
- Physical:
- Trichobezoars (hairballs) → GI obstruction, malnutrition
- Skin irritation, infection
- Dental damage (from biting hair)
- Carpal tunnel syndrome (repetitive motion)
⭐ Trichobezoars are a serious, potentially life-threatening complication requiring surgical intervention in some cases of trichotillomania with trichophagia (hair eating).
High‑Yield Points - ⚡ Biggest Takeaways
- Recurrent hair pulling causes significant hair loss, despite repeated unsuccessful attempts to stop.
- Preceded by increasing tension, followed by relief, pleasure, or gratification.
- Common sites: scalp, eyebrows, eyelashes; rarely involves trichophagia (hair eating).
- High comorbidity with anxiety disorders, MDD, and excoriation (skin-picking) disorder.
- Treatment options include SSRIs (fluoxetine, clomipramine) and N-acetylcysteine.
- Cognitive Behavioral Therapy (CBT), especially Habit Reversal Training (HRT), is the mainstay.
- Typical onset is childhood or early adolescence; can be chronic if untreated.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

