Indications & Selection - Last Resort Options
- Neurosurgery is a last resort for adults with severe, chronic, disabling OCD.
- Strict Selection Criteria:
- Yale-Brown Obsessive Compulsive Scale (Y-BOCS) score > 28-32.
- Illness duration > 5 years with persistent severe symptoms.
- Marked functional impairment despite extensive treatments.
- Defining Treatment-Refractory OCD:
⭐ Neurosurgery is considered only after failure of at least 3 different SSRIs (including clomipramine) at maximum tolerated doses for adequate duration (e.g., ≥3 months each), AND failure of adequate CBT with ERP (e.g., ≥20 expert-led sessions).
- Essential Safeguards:
- Multidisciplinary team (MDT) approval (psychiatrist, neurosurgeon, psychologist).
- Independent ethics committee review and approval.
- Voluntary, comprehensive informed consent; patient must have capacity.
Ablative Techniques - Cutting Edge Cuts
- Ablative techniques create precise, irreversible lesions to modulate specific cortico-striato-thalamo-cortical (CSTC) pathways implicated in severe, treatment-refractory OCD.
- These procedures are reserved for the most severe, incapacitating, and treatment-resistant cases due to their irreversible nature.
📌 CALmS Mnemonic for major procedures:
- Capsulotomy (Anterior)
- Anterior Cingulotomy
- Limbic Leucotomy
- Subcaudate Tractotomy
| Procedure | Key Anatomical Target | Mechanism Snippet |
|---|---|---|
| Anterior Capsulotomy | Anterior limb of internal capsule | Disrupts fronto-striatal connections |
| Anterior Cingulotomy | Anterior cingulate gyrus (Brodmann area 24) | Modulates affective component of OCD |
| Subcaudate Tractotomy | Substantia innominata (orbital frontal-striatal pathways) | Affects orbitofrontal circuits |
| Limbic Leucotomy | Combines Cingulotomy & Subcaudate Tractotomy targets | Broader impact on limbic circuitry |
⭐ Anterior capsulotomy is one of the most studied ablative procedures for OCD, targeting the connection between the thalamus and prefrontal cortex, and the striatum and prefrontal cortex.
Deep Brain Stimulation - Zapping the Circuits
- Principle: Neuromodulation, not lesioning. Modulates abnormal brain circuit activity.
- Mechanism: Delivers electrical impulses to specific brain targets.
- Common Targets for OCD (FDA-approved/investigational): 📌 Mnemonic: OCD needs VAN
- Ventral Capsule/Ventral Striatum (VC/VS)
- Anterior Limb of Internal Capsule (ALIC)
- Nucleus Accumbens (NAcc)
- Components:
- Electrodes (leads) implanted in the brain.
- Extension wires connecting electrodes to IPG.
- Implantable Pulse Generator (IPG) - battery-powered, like a pacemaker.
- Advantages:
- Reversibility: Effects can be stopped.
- Adjustability: Stimulation parameters can be fine-tuned.
- Non-ablative: Preserves brain tissue.
⭐ DBS for OCD is FDA-approved under a Humanitarian Device Exemption (HDE) for severe, treatment-refractory cases.
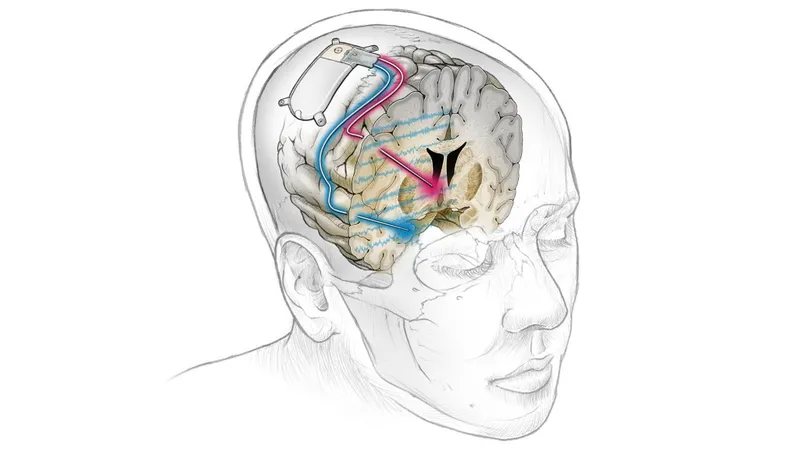 system with electrode placement in Ventral Capsule/Ventral Striatum for OCD treatment)
system with electrode placement in Ventral Capsule/Ventral Striatum for OCD treatment)
Efficacy & Adverse Effects - The Good, Bad, & Brainy
- General Efficacy:
- Response rate: ~50-70% in well-selected, treatment-refractory OCD patients.
- Response defined as ≥35% reduction in Y-BOCS score.
- Adverse Effects (Ablative Surgery):
- Personality changes (apathy, disinhibition).
- Cognitive deficits (memory, executive function).
- Seizures (rare).
- Weight gain, urinary incontinence (procedure-dependent).
- Adverse Effects (Deep Brain Stimulation - DBS):
- Surgical risks: hemorrhage, infection.
- Hardware issues: lead migration, breakage.
- Stimulation-induced (often reversible): paresthesias, dysarthria, mood changes (hypomania, anxiety).
- Long-term follow-up: Essential for monitoring efficacy and adverse effects.
⭐ While potentially effective, neurosurgery for OCD carries risks of significant and sometimes irreversible adverse effects.
High‑Yield Points - ⚡ Biggest Takeaways
- Neurosurgery is a last resort for severe, treatment-refractory OCD, after all other treatments fail.
- Targets dysfunctional Cortico-Striato-Thalamo-Cortical (CSTC) circuits implicated in OCD.
- Key ablative surgeries include Anterior Cingulotomy, Anterior Capsulotomy, and Limbic Leucotomy.
- Deep Brain Stimulation (DBS) is a newer, reversible, and adjustable option targeting the Ventral Capsule/Ventral Striatum (VC/VS) or Nucleus Accumbens (NAc).
- Significant adverse effects can occur, including personality changes, cognitive deficits, or seizures.
- Strict patient selection criteria are paramount before considering any neurosurgical intervention.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

