Definition & Core Features - Piles of Problems
- Hoarding Disorder (HD): Persistent difficulty discarding possessions, regardless of actual value.
- Underlying Factors: Driven by a perceived need to save items and distress associated with discarding.
- Result: Accumulation of possessions clutters active living areas, compromising their intended use.
- Impact: Causes significant distress or impairment in social, occupational, or other important areas, including maintaining a safe environment.
- 📌 Mnemonic (SAVE):
- Saving items (persistent)
- Anxiety when discarding
- Value (perceived, not actual)
- Environmental clutter
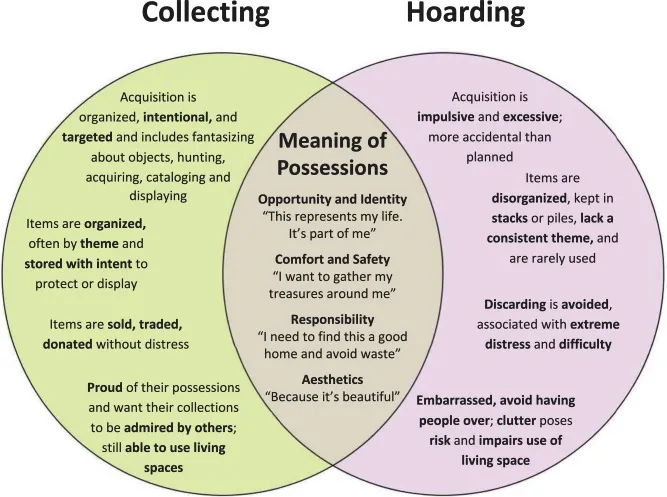
⭐ Hoarding Disorder is distinct from normal collecting, which is organized and doesn't cause significant distress or impairment.
Epidemiology & Etiology - Clutter's Causes
- Prevalence: 2-6% in general population.
- Age of Onset:
- Often childhood/adolescence (e.g., 11-15 years).
- Clinically significant impairment usually in adulthood.
⭐ Symptoms often begin in early adolescence but may not cause significant impairment until middle age or later.
- Course: Chronic, often progressive; severity typically ↑ with age.
- Etiological Factors:
- Genetic: Strong familial clustering; heritability approx. 50%.
- Neurobiological:
- Frontal lobe dysfunction (e.g., anterior cingulate cortex, insula).
- Deficits in decision-making, categorization, attention.
- Cognitive-Behavioral:
- Information processing deficits (e.g., difficulty organizing).
- Erroneous beliefs about possessions' utility/value.
- Strong emotional attachment to objects.
Diagnosis & DDx - Spotting the Stash Pile
- DSM-5 Criteria (Summarized):
- A: Persistent difficulty discarding possessions, regardless of value.
- B: Perceived need to save items; distress with discarding.
- C: Possessions accumulate, cluttering active living areas, compromising use.
- D: Causes clinically significant distress or impairment (social, occupational, etc.).
- E: Not due to another medical condition (e.g., brain injury, CVA).
- F: Not better explained by another mental disorder (e.g., OCD, depression, schizophrenia).
- Specifiers:
- With excessive acquisition: Common (approx. 80-90% of individuals).
- Insight: Good/fair, poor, or absent/delusional beliefs.
- Assessment:
- Clinical interview.
- Clutter Image Rating (CIR).
- Differential Diagnosis (DDx):
- OCD: Hoarding of specific, unwanted/intrusive items; ego-dystonic.
- OCPD: Perfectionism, indecisiveness, but not true hoarding of valueless items.
- Other Medical/Neurodevelopmental/Psychotic Disorders: (e.g., Prader-Willi, Schizophrenia, Dementia, Brain Injury) - hoarding is secondary.
- Normal Collecting: Organized, does not cause significant distress/impairment.
⭐ The 'with excessive acquisition' specifier is crucial as it highlights a common and problematic aspect of the disorder.
Management & Complications - Tackling the Trove
- Psychotherapy (Primary): Specialized CBT for Hoarding Disorder (HD). Key elements:
- Pharmacotherapy (Adjunctive):
- SSRIs (e.g., paroxetine, venlafaxine) may be used; evidence less robust than for OCD. Often augments CBT.
⭐ Multi-component CBT tailored for hoarding, often including home visits and skills training (organizing, decision-making, discarding), shows strongest evidence.
-
Complications:
- Health hazards: Falls, fire, poor sanitation, pests.
- Social: Isolation, family conflict, work issues.
- Functional: Eviction risk, ↓ quality of life, unusable living spaces.
-
Prognosis:
- Often chronic; treatment challenging.
- Motivation is a key factor.
- Long-term support usually needed for sustained improvement.
High‑Yield Points - ⚡ Biggest Takeaways
- Persistent difficulty discarding possessions, regardless of actual value, leading to significant clutter.
- Strong perceived need to save items and notable distress upon discarding.
- Clutter compromises living spaces' intended use and can affect safety.
- Causes clinically significant distress or functional impairment.
- Specifiers: With excessive acquisition (very common); insight varies (good/fair to absent/delusional).
- Often ego-syntonic; specialized CBT for hoarding is primary treatment; SSRIs are less effective.
- Prevalence approx. 2-6%; typically chronic course, worsening with age if untreated.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

