Body Dysmorphic Disorder - Flawed Reflections
- Preoccupation with ≥1 perceived defects/flaws in physical appearance, not observable or appearing slight to others.
- Repetitive behaviors (e.g., mirror checking, excessive grooming, skin picking, reassurance seeking) or mental acts (e.g., comparing appearance to others).
- Causes clinically significant distress/impairment.
- Specify: muscle dysmorphia, insight level (good/fair, poor, absent/delusional).
⭐ BDD has high rates of suicidal ideation (~80%) and attempts (~25-30%).
Body Dysmorphic Disorder - Unmasking BDD Roots
- Epidemiology:
- Prevalence: ~2.4% (general population); higher in cosmetic surgery settings (~15%) and dermatology clinics.
- Age of Onset: Typically adolescence (mean 16-17 years); often insidious.
- Gender: Slightly more common in females; males may present with muscle dysmorphia.
- Etiology: Multifactorial model
- Genetic: Increased risk in first-degree relatives.
- Neurobiological: Serotonin pathway dysregulation; abnormalities in visual processing (bias towards details over holistic view).
- Psychological: Childhood trauma (e.g., teasing, abuse), perfectionism, low self-esteem.
- Sociocultural: Societal emphasis on appearance, media influence.
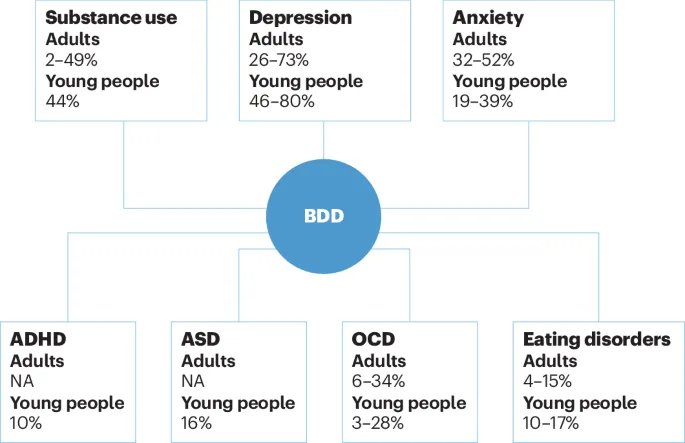
⭐ BDD has high comorbidity with major depressive disorder (MDD), social anxiety disorder, and obsessive-compulsive disorder (OCD). Suicidal ideation is notably high in BDD patients.
Body Dysmorphic Disorder - Symptom Spotlight
- Preoccupations: Focus on perceived flaws in appearance (e.g., skin, hair, nose, teeth, weight, muscles).
- Flaws are slight or not observable to others.
- Common areas: face (acne, scars, asymmetry), hair (thinning, excessive), nose shape/size.
- Repetitive Behaviors (Compulsions): In response to appearance concerns.
- Mirror checking (excessive).
- Excessive grooming.
- Skin picking.
- Reassurance seeking.
- Comparing appearance with others.
- Camouflaging (e.g., with makeup, clothing, hats).
⭐ Insight specifier: BDD can occur with good/fair insight, poor insight, or absent insight/delusional beliefs (most severe).
Body Dysmorphic Disorder - Diagnosis Decoded
- Insight: Good/fair, poor, absent/delusional.
- Muscle dysmorphia: Variant, focus on muscularity.
- DDx: OCD, Eating Disorders, Social Anxiety.
⭐ High suicide risk (~25-28% attempts); often seeks cosmetic procedures, usually with poor satisfaction.
Body Dysmorphic Disorder - Treatment & Outlook
- Pharmacotherapy:
⭐ SSRIs (e.g., Fluoxetine) are first-line, needing higher doses (Fluoxetine 60-80 mg/day) & longer trials (10-12 wks) than for depression.
- Clomipramine (TCA): Potent serotonergic; effective second-line.
- Augmentation: Antipsychotics (e.g., Aripiprazole) for delusional insight or refractory BDD.
- Psychotherapy:
- Cognitive Behavioral Therapy (CBT) with Exposure and Response Prevention (ERP): Gold standard. Targets cognitive distortions, compulsive behaviors/rituals.
- Psychoeducation for patient & family is vital.
- Outlook & Prognosis:
- Chronic, fluctuating course if untreated.
- High comorbidity: Depression, anxiety, social phobia, OCD.
- ↑↑ Suicidal ideation (~80%) & attempts (~25-30%).
- Combined treatment offers significant improvement; complete remission less common. Relapse risk if treatment stopped.
High-Yield Points - ⚡ Biggest Takeaways
- Preoccupation with one or more perceived flaws in physical appearance, not observable or appearing slight to others.
- Engages in repetitive behaviors (e.g., mirror checking, skin picking, reassurance seeking) or mental acts (e.g., comparing appearance) due to appearance concerns.
- Causes clinically significant distress or functional impairment.
- Insight varies: good/fair, poor, to absent/delusional (BDD with delusional beliefs).
- High comorbidity with depression, anxiety disorders, OCD; significant suicide risk.
- Treatment: SSRIs (often high doses, e.g., fluoxetine) and CBT (Exposure and Response Prevention).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

