Definition & Diagnosis - Spotting Stubborn Sadness
- Treatment-Resistant Depression (TRD): Defined as Major Depressive Disorder (MDD) that fails to achieve satisfactory improvement despite ≥2 adequate trials of different antidepressant medications.
- "Adequate trial": Sufficient dose (optimal range) for sufficient duration (typically 6-8 weeks).
- Antidepressants should ideally be from different pharmacological classes, or include an augmentation strategy.
- Critical Diagnostic Steps:
- Confirm the primary diagnosis of MDD (using DSM-5 or ICD-11 criteria).
- Thoroughly rule out pseudo-resistance:
- Inadequate antidepressant dose or duration.
- Poor patient adherence to treatment.
- Presence of unaddressed comorbid medical conditions (e.g., hypothyroidism, anemia) or psychiatric conditions (e.g., anxiety disorders, substance use).
- Misdiagnosis (e.g., Bipolar depression, personality disorder).
- Assess overall illness severity and functional impairment.
⭐ Approximately 30-40% of individuals with MDD may not respond adequately to initial standard antidepressant treatments, potentially meeting criteria for TRD.
Evaluation & Workup - Digging Deeper Doc
- 1. Confirm MDD & Severity:
- Exclude Bipolar Disorder (e.g., MDQ).
- Standardized scales (e.g., HAM-D, MADRS).
- 2. Review Treatment History (📌 "2 D's & A"):
- Duration: ≥ 6-8 weeks per trial.
- Different Classes: ≥ 2 failed adequate trials.
- Adherence & Adequate Dose.
- 3. Screen for Confounders:
- Medical: CBC, TSH, Vit B12/D.
- Substance use.
- Comorbid psychiatric conditions (anxiety, personality disorders).
- 4. Psychosocial Assessment:
- Stressors, social support.
⭐ A key criterion for TRD is failure to respond to at least two different antidepressant trials of adequate dose and duration (typically 6-8 weeks each).
Pharmacological Strategies - Pill Power-Ups
- Optimization: Optimize current AD: Maximize dose & ensure adequate trial duration (4-6 weeks).
- Switching: Switch AD: To another agent, intra-class or different class (e.g., SSRI to SNRI/TCA).
- Augmentation Strategies:
- Lithium: Target 0.6-1.2 mEq/L.
- AAPs: e.g., Aripiprazole, Quetiapine XR, Olanzapine, Risperidone.
- Thyroid Hormone (T3 - Liothyronine): 25-50 mcg/day.
- Buspirone.
- Combination Therapy: Combine ADs: Different mechanisms (e.g., SSRI + Mirtazapine/Bupropion). ⚠️ Serotonin Syndrome.
- Novel Rapid-Acting Agents: Esketamine (intranasal)/Ketamine (IV): Rapid-acting agents for severe TRD or acute suicidal ideation.
- MAOIs (e.g., Phenelzine, Tranylcypromine): Potent, but last-line. Strict dietary (tyramine) & drug interaction precautions. ⚠️ Hypertensive Crisis.
⭐ Lithium augmentation is a gold-standard TRD strategy; response often in 2-4 weeks at therapeutic levels (0.6-1.2 mEq/L).
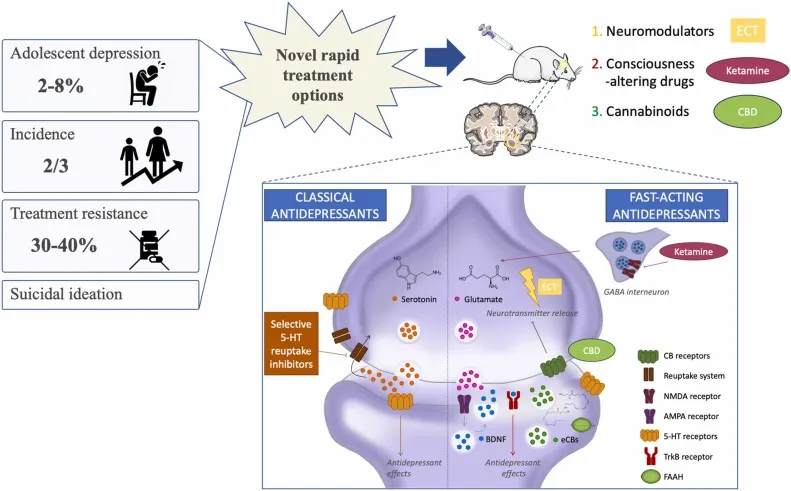
Non-Pharmacological Tx - Brain Boost & Banter
- Electroconvulsive Therapy (ECT)
- Indications: Severe TRD, psychotic features, catatonia, high suicide risk.
- Procedure: 2-3 sessions/week for 6-12 total. Bilateral or RUL (Right Unilateral) placement.
- Key SE: Transient memory loss (anterograde > retrograde), headache.
⭐ ECT has the most rapid antidepressant effect; often life-saving in severe cases with acute suicidality.
- Psychotherapy ("Banter")
- Cognitive Behavioural Therapy (CBT): Addresses negative thought patterns & maladaptive behaviours.
- Interpersonal Psychotherapy (IPT): Focuses on relationship difficulties impacting mood.
- Often adjunctive; improves coping, adherence & relapse prevention.
- Other Neurostimulation
- Repetitive Transcranial Magnetic Stimulation (rTMS): Non-invasive; targets Dorsolateral Prefrontal Cortex (DLPFC). Daily sessions for 4-6 weeks. Fewer cognitive SE than ECT.
- Vagus Nerve Stimulation (VNS): Implanted device for chronic TRD; adjunctive.
- Deep Brain Stimulation (DBS): Investigational; for highly refractory TRD.
High‑Yield Points - ⚡ Biggest Takeaways
- TRD: Failure of ≥2 adequate antidepressant trials from different classes.
- Augmentation strategies: Lithium, atypical antipsychotics (e.g., aripiprazole, quetiapine), thyroid hormone (T3).
- Esketamine nasal spray: Rapid-acting NMDA antagonist for TRD.
- ECT: Most effective for severe TRD, especially with psychotic features or suicidality.
- rTMS: Non-invasive brain stimulation option.
- Consider VNS for chronic TRD.
- Always exclude pseudo-resistance (e.g., non-adherence, inadequate dose/duration).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

