Psychotherapy Fundamentals - Mind Menders
- Goal: Modify maladaptive thoughts, feelings, behaviors; improve functioning & quality of life.
- Core Elements:
- Therapeutic Alliance: Collaborative, trusting relationship.
- Empathy & Active Listening: Understanding patient perspective.
- Goal Setting: Mutually agreed objectives.
- Key Principles: Confidentiality, non-judgmental stance, patient-centered approach.
- Role in Mood Disorders:
- Reduces symptom severity (depression, hypomania/mania).
- Enhances coping mechanisms & resilience.
- Aids in relapse prevention.
- Improves medication adherence & insight.
⭐ The therapeutic alliance is a robust predictor of positive outcomes across various psychotherapeutic modalities for mood disorders.
CBT & Behavioral Activation - Thought & Action Allies
Structured psychotherapies targeting thoughts and actions in mood disorders.
- Cognitive Behavioral Therapy (CBT):
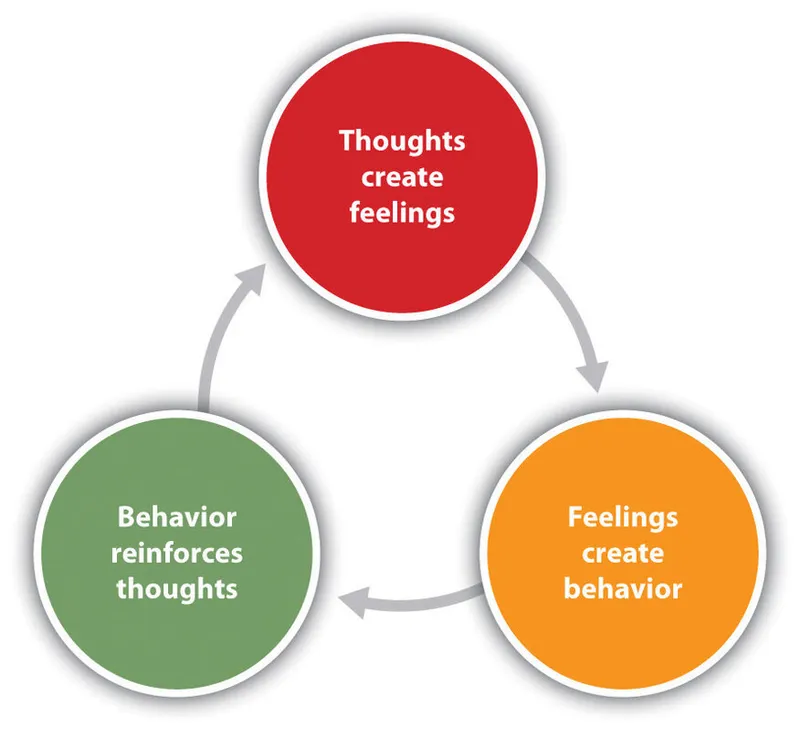
- Core: Thoughts, emotions, behaviors are interconnected. Aims to break negative cycles.
- Goal: Identify & modify maladaptive cognitions (e.g., cognitive distortions) & behaviors.
- Techniques: Socratic questioning, thought records, behavioral experiments.
- Duration: 12-20 sessions.
- Behavioral Activation (BA):
- Core: Depression linked to ↓ environmental positive reinforcement.
- Goal: Systematically ↑ engagement in rewarding activities.
- Techniques: Activity monitoring, scheduling, values-based selection.
⭐ Cognitive Behavioral Therapy (CBT) is highly effective for acute depression and also significantly reduces relapse rates, particularly when continued with maintenance sessions.
Interpersonal & Problem-Solving Therapies - Relationship & Resolve Routes
- Interpersonal Therapy (IPT):
- Time-limited; links mood to current interpersonal events & relationships.
- Aims: Improve interpersonal functioning & social support.
- Addresses 1-2 of 4 key problem areas:
- Grief (complicated bereavement)
- Interpersonal role disputes (conflicts with significant others)
- Role transitions (difficult life changes, e.g., new job, illness)
- Interpersonal deficits (social isolation, unfulfilling relationships)
⭐ Interpersonal Therapy (IPT) typically focuses on resolving one or two of four key interpersonal problem areas: grief, interpersonal role disputes, role transitions, and interpersonal deficits.
- Problem-Solving Therapy (PST):
- Structured; teaches skills to solve problems causing distress.
- Steps: Problem definition & formulation, generation of alternative solutions, decision-making, solution implementation & verification.
- Goal: Improve problem-solving abilities & reduce distress by tackling life difficulties systematically.
Diverse Therapeutic Approaches - Support & Systems
- Psychodynamic Therapy: Focuses on understanding unconscious conflicts and past experiences influencing current mood; aims for insight.
- Supportive Therapy: Provides emotional support, empathy, reassurance; aims to strengthen defenses, improve adaptive skills, and reduce anxiety.
- Psychoeducation: Essential for all mood disorders. Educates patients and families on illness, treatment options, adherence, and early warning signs of relapse.
⭐ Family-Focused Therapy (FFT), when combined with pharmacotherapy, is particularly effective in improving outcomes and reducing relapse in Bipolar Disorder by addressing family communication and problem-solving.
Treatment Selection & Application - Therapy Tailors
- Individualize: Disorder, severity, patient preference, chronicity.
- Therapy by Disorder:
- MDD: CBT, IPT, Behavioral Activation (BA).
- Bipolar: Psychoeducation, FFT, IPSRT (adjunctive).
- Dysthymia/Cyclothymia: CBT, IPT.
- Also consider: Comorbidities, resources.
For moderate to severe Major Depressive Disorder, a combination of psychotherapy (like CBT or IPT) and antidepressant medication is generally more effective than either treatment alone. ⭐
High‑Yield Points - ⚡ Biggest Takeaways
- CBT is first-line for mild-moderate MDD & Dysthymia, addressing negative thoughts/behaviors.
- IPT treats depression by improving interpersonal relationships and resolving conflicts.
- Behavioral Activation combats depression by scheduling and increasing engagement in pleasant activities.
- MBCT is highly effective for relapse prevention in recurrent MDD.
- IPSRT (stabilizing daily rhythms) & FFT (improving family communication) are key for Bipolar Disorder.
- Psychotherapy is an essential adjunct to medication for moderate-severe MDD and Bipolar Disorder.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

