PDD Basics - The Long Gloom
- A chronic, low-grade depression: depressed mood for most of the day, more days than not, for at least 2 years (adults) or 1 year (children/adolescents).
- Represents a consolidation of DSM-IV chronic Major Depressive Disorder (MDD) and Dysthymic Disorder.
- Lifetime prevalence: ~1.5% to 6%. Indian data aligns with global figures.
- Age of Onset: Early (<21 years, often insidious) or Late (≥21 years, may follow stressors).
- Gender Ratio: Women > Men (2-3:1).
⭐ PDD was formerly known as Dysthymic Disorder or Dysthymia.
PDD Symptoms - Chronic Blues Clues
- Depressed mood (most days, more often than not) for at least:
- 2 years in adults.
- 1 year in children/adolescents.
- During this period, the individual has never been without the above symptoms for more than 2 months at a time.
- Plus ≥2 of the following symptoms (📌 HE'S 2 SAD):
- Hopelessness (feelings of)
- Energy loss or fatigue
- Low Self-esteem
- Sleep problems (insomnia/hypersomnia)
- Appetite changes (poor appetite/overeating)
- Difficulty concentrating or making decisions
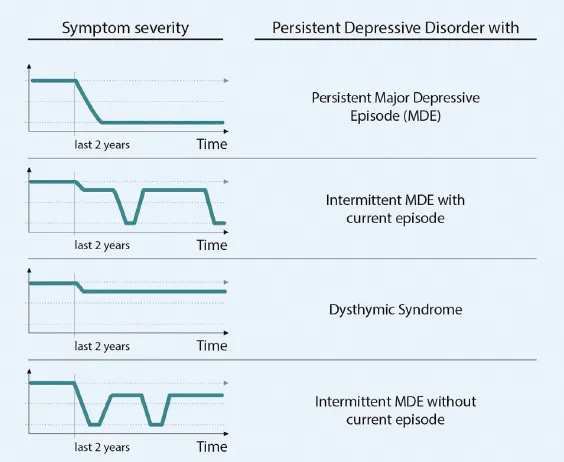
- Specifiers include:
- With pure dysthymic syndrome
- With persistent major depressive episode
- With intermittent major depressive episodes (with/without current episode)
⭐ Early onset PDD (before age 21) is associated with an ↑ likelihood of comorbid personality disorders and a more chronic course.
PDD Diagnosis - Spotting the Shadow
DSM-5 Criteria (A-H):
- A: Depressed mood (child: irritable) >50% days; ≥2 yrs (child/adol: ≥1 yr).
- B: While depressed, ≥2 of:
- Appetite/sleep changes
- Low energy
- Low self-esteem
- Poor concentration/indecision
- Hopelessness
- C: Symptoms A+B not absent >2 months in 2-yr (1-yr) period.
- D: MDD criteria may be continuous for 2 yrs (PDD with persistent MDE). Else, no MDE in initial 2 yrs.
- E: No mania/hypomania/cyclothymia.
- F: Not other psychotic disorder.
- G: Not substance/medical.
- H: Distress/impairment.
⭐ MDD criteria continuously present for 2 years can be PDD with persistent MDE specifier.
Key Differentials:
- MDD (chronic)
- Cyclothymic, Bipolar II
- Personality Disorders
- Substance/Medical induced
PDD Treatment - Road to Relief
- Pharmacotherapy:
- First-line: SSRIs (e.g., fluoxetine, sertraline), SNRIs (e.g., venlafaxine, duloxetine).
- Second-line: TCAs (e.g., imipramine, amitriptyline) - use with caution (side effects, cardiotoxicity).
- MAOIs (e.g., phenelzine) - rarely used due to dietary (tyramine) restrictions, drug interactions.
- Psychotherapy:
- Evidence-based: Cognitive Behavioral Therapy (CBT), Interpersonal Therapy (IPT), psychodynamic psychotherapy, problem-solving therapy.
- Combination Therapy:
⭐ Combination of psychotherapy (e.g., CBT, IPT) and pharmacotherapy (e.g., SSRIs) is generally considered the most effective treatment for PDD.
- Duration: Often requires longer treatment (≥ 2 years) than acute MDD.
- ECT: Consider for severe, treatment-resistant PDD, especially with superimposed Major Depressive Episode (MDE).
PDD Outlook - Future Forecast
- Course: Chronic; insidious onset (childhood/adolescence/early adult).
- Prognosis: Poorer than episodic MDD if untreated; ↑ relapse rates.
- Complications/Comorbidities:
- 'Double depression' (PDD + MDE)
- Anxiety Disorders (GAD, panic, social)
- Substance Use Disorders
- Personality Disorders (Cluster B & C)
- Impact: Significant psychosocial & quality of life impairment.
⭐ PDD often has an early and insidious onset, and by definition, a chronic course; 'double depression' (PDD + MDE) carries a worse prognosis.
High‑Yield Points - ⚡ Biggest Takeaways
- Chronic depressed mood for at least 2 years (1 year in children/adolescents).
- Requires ≥2 of: appetite/sleep changes, low energy, low self-esteem, poor concentration, hopelessness.
- Symptoms not absent for more than 2 months at a time.
- No Major Depressive Episode during the initial 2 years of the disturbance.
- "Double depression" refers to PDD with superimposed Major Depressive Episodes.
- Often has an earlier, insidious onset compared to Major Depressive Disorder.
- Treatment: Psychotherapy (CBT, IPT) and/or SSRIs are first-line options.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

