Bipolar Depressive Episodes - The Downward Spiral
- Core symptoms mirror Major Depressive Disorder (MDD):
- Persistent low mood, anhedonia.
- Changes in sleep (insomnia/hypersomnia), appetite (↓/↑).
- Fatigue, psychomotor retardation/agitation.
- Difficulty concentrating, feelings of worthlessness, suicidal ideation.
- Duration: Symptoms present for at least 2 weeks.
- Key differentiator from unipolar depression: History of at least one manic or hypomanic episode.
- Often more severe, with ↑ risk of psychosis & suicide attempts than unipolar depression.
- Treatment challenges: Antidepressant monotherapy can precipitate mania/hypomania.
⭐ Atypical features (e.g., hypersomnia, hyperphagia, leaden paralysis, mood reactivity) are more common in bipolar depression compared to unipolar depression.
Bipolar Mixed Episodes - The Emotional Storm
- Co-occurrence of manic/hypomanic AND depressive symptoms nearly every day during a mood episode.
- DSM-5: Specifier "with mixed features" for manic, hypomanic, or depressive episodes.
- Presents as emotional turmoil: e.g., high energy with despair, racing thoughts with guilt.
- Key features:
- Manic/Hypomanic: Agitation, irritability, distractibility, flight of ideas.
- Depressive: Depressed mood, anhedonia, worthlessness, suicidal ideation.
- High risk: ↑ suicide attempts, ↑ substance abuse, poorer prognosis.
- Treatment: Mood stabilizers (e.g., valproate), atypical antipsychotics. Avoid antidepressant monotherapy.
⭐ Episodes with mixed features (simultaneous manic/hypomanic and depressive symptoms) are associated with a higher risk of suicide attempts, substance abuse, and poorer treatment response.
Diagnosis & DDx - Spotting the Switch
- Primary Goal: Differentiate Bipolar Depression from Unipolar Major Depressive Disorder (MDD).
- Key: Meticulous history for any past manic or hypomanic episodes.
- Family history of bipolar disorder also informative.
- Screening: Mood Disorder Questionnaire (MDQ) useful.
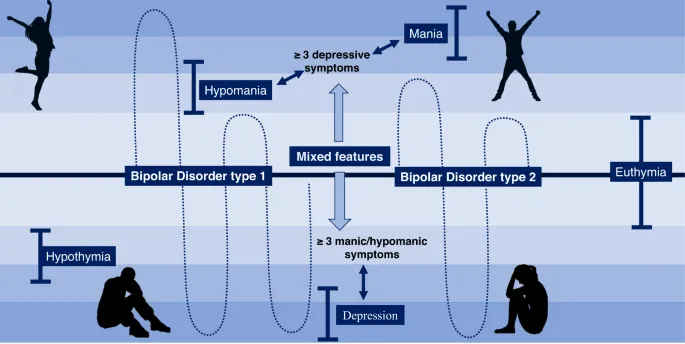
- Mixed Features: Major Depressive Episode (MDE) + ≥3 (hypo)manic symptoms OR Mania/Hypomania + ≥3 depressive symptoms.
- DDx: Unipolar MDD, Cyclothymia, Schizoaffective disorder, Substance-induced mood disorder, Mood disorder due to another medical condition.
⭐ A thorough history for past (hypo)manic episodes is crucial in any patient presenting with depression to differentiate bipolar disorder from unipolar depression; tools like the Mood Disorder Questionnaire (MDQ) can aid screening.
Management Principles - Calming the Waves
- Goals: Remission, relapse prevention, improved function.
- Prioritize mood stabilization when addressing depressive symptoms.
Bipolar Depression:
- First-line Pharmacotherapy:
- Quetiapine (monotherapy or adjunct)
- Lurasidone (monotherapy or adjunct with Lithium/Valproate)
- Olanzapine-Fluoxetine Combination (OFC)
- Lamotrigine (slower onset, good for prevention)
- Lithium (less robust for acute depression vs. mania)
- Adjunctive: Psychotherapy (CBT, IPSRT, FFT).
- Severe/Resistant: ECT.
⭐ Antidepressant monotherapy is generally contraindicated in bipolar depression due to the risk of inducing mania or rapid cycling; if used, it should be in combination with an effective mood stabilizer or atypical antipsychotic.
Mixed Episodes:
- Goal: Target both manic & depressive symptoms.
- First-line Pharmacotherapy:
- Atypical Antipsychotics (e.g., Olanzapine, Risperidone, Asenapine, Cariprazine)
- Valproate
- Avoid: Antidepressant monotherapy (risk: worsens mania/agitation).
- Adjunctive: Benzodiazepines (short-term for agitation).
- Severe/Resistant: ECT.
High‑Yield Points - ⚡ Biggest Takeaways
- Bipolar depression resembles MDD; past mania/hypomania is the key differentiator.
- Mixed episodes: concurrent manic and depressive symptoms for at least 1 week, causing marked impairment.
- Both states carry a significantly elevated suicide risk.
- Antidepressant monotherapy risks inducing mania/hypomania; use with mood stabilizers.
- Lamotrigine is effective for bipolar depression; Valproate or atypical antipsychotics (e.g., olanzapine) for mixed episodes.
- Lurasidone, Quetiapine, Cariprazine are specific atypical antipsychotics for bipolar I depression.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

