Psychiatric Formulation - Mind Map Making
- Definition: A dynamic, concise biopsychosocial hypothesis that seeks to explain why this particular patient developed this specific problem at this particular time. It integrates:
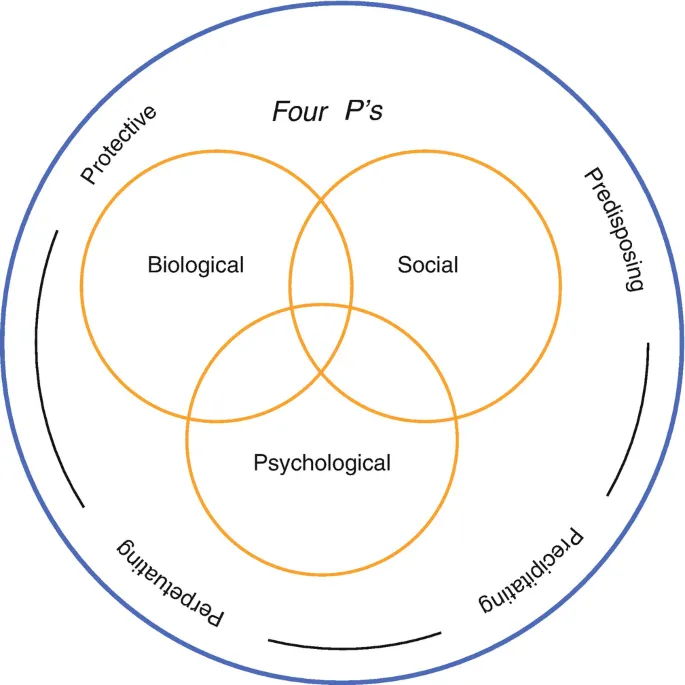
- Predisposing factors (e.g., genetics, early experiences)
- Precipitating factors (e.g., recent stressors, life events)
- Perpetuating factors (e.g., ongoing substance use, poor coping)
- Protective factors (e.g., social support, resilience)
- Purpose:
- Achieve a holistic, shared understanding of the patient's difficulties.
- Guide collaborative and individualized treatment planning.
- Inform prognosis and anticipate therapeutic challenges.
- Nature:
- Idiographic: Focuses on the unique narrative and context of the individual, beyond diagnostic labels.
⭐ A good formulation tells a story of the patient.
 oka
oka
Biopsychosocial Model & 4P's - The 4P Framework
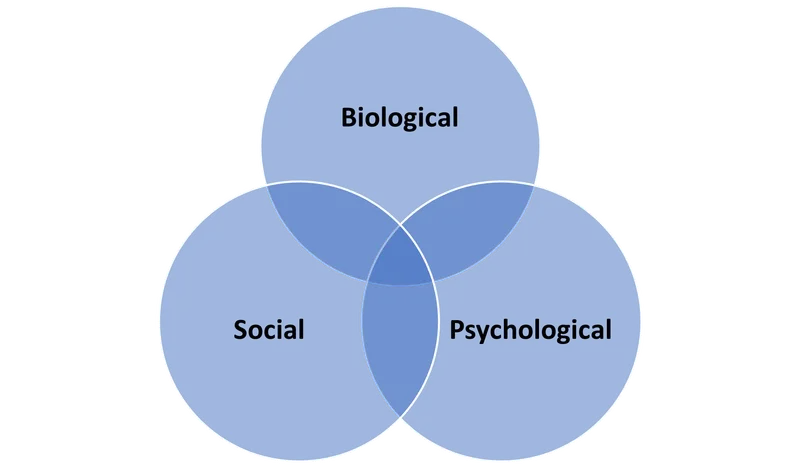
The Biopsychosocial (BPS) model views illness as an interplay of biological (e.g., genetics, neurochemistry), psychological (e.g., thoughts, coping styles), and social (e.g., family, culture, socioeconomic status) factors, promoting a holistic understanding.
The 4P framework structures case formulation: 📌 Psychiatry's Problem-solving Process Plan.
- Predisposing factors: Increase vulnerability (e.g., family history of mental illness, early life trauma, genetic predisposition).
- Precipitating factors: Triggers for the current episode (e.g., recent major life stressor, substance use initiation, acute medical illness).
- Perpetuating factors: Maintain the disorder (e.g., poor coping mechanisms, ongoing family conflict, lack of social support, medication non-adherence).
- Protective factors: Strengths/supports that reduce impact or aid recovery (e.g., good insight, strong social network, resilience, access to treatment).
⭐ The 4 P's model is crucial for a comprehensive case understanding and treatment planning in psychiatry, guiding tailored interventions.
Psychiatric Diagnosis & Classification - Decoding Disorder Codes
- Psychiatric Diagnosis: The process of identifying a mental disorder by evaluating an individual's signs and symptoms against established criteria.
- Purpose:
- Ensures reliable communication among clinicians.
- Guides treatment selection and prognosis.
- Facilitates research by defining comparable patient groups.
- Nature: Nomothetic - aims to classify individuals into general categories based on shared characteristics.
- Purpose:
- Major Classification Systems:
- DSM-5 (Diagnostic and Statistical Manual of Mental Disorders, 5th Ed.):
- Published by American Psychiatric Association (APA).
- Widely used in US; influential for global research.
- Features detailed diagnostic criteria; non-axial system.
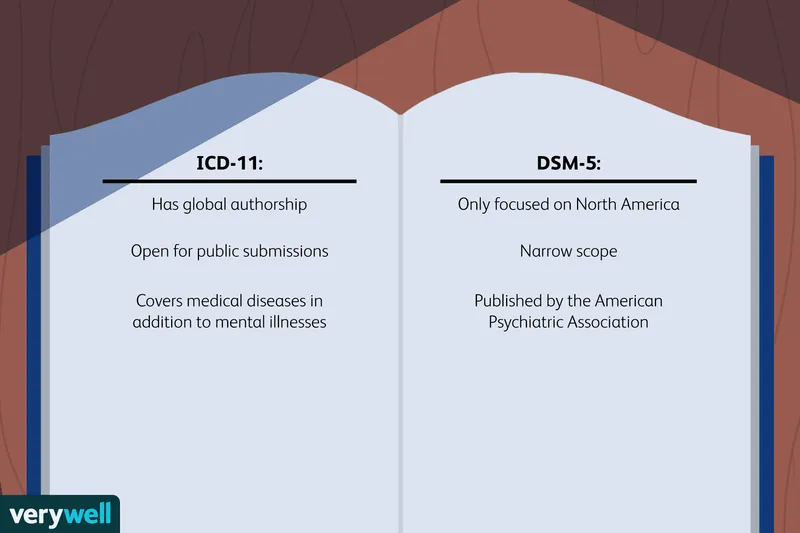
- ICD-11 (International Classification of Diseases, 11th Rev.):
- Published by World Health Organization (WHO).
- Global standard for all health conditions, including mental disorders.
- Used for official health statistics and clinical coding in India; free access.
⭐ ICD is produced by WHO, while DSM is by APA; ICD is more commonly used for official reporting in India.
- DSM-5 (Diagnostic and Statistical Manual of Mental Disorders, 5th Ed.):
Formulation vs. Diagnosis - Two Sides Coin
| Aspect | Formulation | Diagnosis |
|---|---|---|
| Approach | Idiographic: Focuses on the individual's unique story & context. | Nomothetic: Applies general laws or categories. |
| Goal | Understanding: "Why this person, this problem, at this time?" | Categorizing: "What recognized disorder does this person have?" |
| Nature | A process of developing an explanatory hypothesis; dynamic. | A label or classification based on established criteria (e.g., DSM, ICD). |
| Output | A narrative summary integrating biopsychosocial factors (4P model: Predisposing, Precipitating, Perpetuating, Protective). | A specific diagnostic code (e.g., F32.2 Major Depressive Disorder). |
⭐ Formulation guides individualized treatment, while diagnosis aids in standardized care and research.
- Complementary Roles: Not mutually exclusive; both are vital for comprehensive psychiatric care.
- Formulation provides a holistic understanding of the patient; diagnosis offers a standardized framework for communication and research.
- Think: Formulation = the story & explanation; Diagnosis = the chapter title or label.
High‑Yield Points - ⚡ Biggest Takeaways
- The Biopsychosocial model is fundamental for holistic psychiatric formulation.
- Diagnosis adheres to DSM-5/ICD-11 criteria for standardization.
- Formulation is a personalized hypothesis integrating 4P factors (Predisposing, Precipitating, Perpetuating, Protective).
- Mental Status Examination (MSE) is a cornerstone of clinical assessment of current functioning.
- Differentiate symptoms (patient-reported) from signs (clinician-observed).
- Reliability and validity are critical for diagnostic classifications.
- Cultural factors significantly influence illness presentation and diagnosis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

