Overview & ER Approach - Tox Triage Tactics
- Intoxication: Reversible syndrome due to substance. Withdrawal: Symptoms on cessation/reduction.
- ER Approach:
- Prioritize ABCDE (Airway, Breathing, Circulation, Disability [GCS, pupils, glucose!], Exposure).
- History (📌 SAMPLE), exam (vitals, neuro, toxidromes).
- Investigations: Bedside glucose (critical!), ECG, consider tox screen.
- Tox Triage:
- Identify toxidromes (e.g., Opioid, Sympathomimetic).
- Management: Supportive care, decontamination (activated charcoal if <1 hr, specific criteria), antidotes.
⭐ Always consider and rule out hypoglycemia in any patient presenting with altered mental status, especially in suspected intoxication. oka
Alcohol: Intoxication & Withdrawal - The Ethanol Enigma
- Intoxication: Slurred speech, ataxia, nystagmus, impaired judgment, ↓LOC. Supportive care.
- Withdrawal (AWS):
- Early (6-12h): Tremor, anxiety, insomnia, GI upset, palpitations.
- Seizures: Generalized tonic-clonic (12-48h).
- Hallucinosis: Auditory/visual (12-48h), clear sensorium.
- Delirium Tremens (DTs): (48-96h). Confusion, agitation, fever, tachycardia, HTN. Mortality up to 5%.
- Assessment: 📌 CIWA-Ar scale (>8-10 needs meds).
- Treatment: Benzodiazepines (Lorazepam, Diazepam). Thiamine 100mg IV/IM.
⭐ Administer IV Thiamine before glucose in suspected Wernicke's encephalopathy to prevent precipitation or worsening of the condition.
- Wernicke's Encephalopathy (WE): Triad: Confusion, ophthalmoplegia (nystagmus, CN VI palsy), ataxia. Thiamine deficiency.
Opioids & Sedatives: Intox & Withdrawal - Nod & Numbness
Opioids:
- Intoxication: 📌 Triad: Miosis (pinpoint pupils), respiratory depression, coma. Other: ↓BP, ↓HR, euphoria. Rx: Naloxone (0.4-2mg IV, repeat PRN).
- Withdrawal: Flu-like symptoms (lacrimation, rhinorrhea, myalgia, N/V/D), mydriasis, piloerection, yawning. Rx: COWS scale, symptomatic (clonidine), buprenorphine/methadone.
Sedative-Hypnotics (Benzodiazepines - BZD, Barbiturates - BARB):
- Intoxication: Drowsiness, slurred speech, ataxia, nystagmus, ↓respiration (esp. BARB or BZD + alcohol).
- BZD Rx: Flumazenil (0.2mg IV q1min, max 3mg).
⭐
Flumazenil is generally contraindicated in chronic benzodiazepine users or suspected co-ingestion of tricyclic antidepressants due to the high risk of precipitating intractable seizures.
- BARB Rx: Supportive, alkalinize urine (phenobarbital), hemodialysis.
- BZD Rx: Flumazenil (0.2mg IV q1min, max 3mg).
⭐
- Withdrawal: ⚠️ Life-threatening: Anxiety, insomnia, tremors, ↑HR, ↑BP, sweating, seizures, delirium. Rx: CIWA-B scale, long-acting BZD taper (e.g., diazepam).
Stimulants, Hallucinogens & Toxidromes - Mind-Altering Mayhem
- Stimulants (Cocaine, Amphetamines): Agitation, psychosis, mydriasis, diaphoresis, ↑HR, ↑BP. Manage: Benzodiazepines.
- Hallucinogens:
- LSD: Visual hallucinations, synesthesia.
- PCP: Aggression, rotatory nystagmus, ataxia.
⭐ Rotatory nystagmus is a pathognomonic sign highly suggestive of Phencyclidine (PCP) intoxication.
- Cannabis: Euphoria, conjunctival injection.

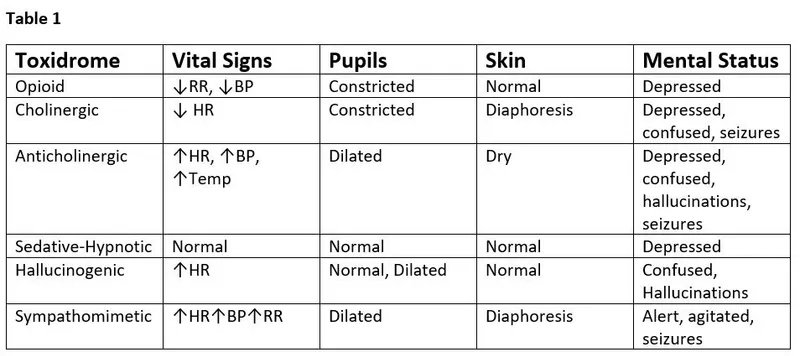
Key Toxidromes:
| Toxidrome | Mental Status | Pupils | HR | BP | Temp | Skin | Bowel Sounds | Other |
|---|---|---|---|---|---|---|---|---|
| Opioid | Depressed | Miosis | ↓ | ↓ | ↓ | Cool | ↓ | Resp. depression |
| Sympathomimetic | Agitated | Mydriasis | ↑ | ↑ | ↑ | Diaphoretic | ↑ | Seizures |
| Anticholinergic | Agitated/Deli | Mydriasis | ↑ | ↑ | ↑ | Dry, flushed | ↓ | Urinary retention 📌 Mad hatter, blind bat, red beet, hot hare, dry bone |
| Cholinergic | Confused/Coma | Miosis | ↓/↑ | ↓/↑ | N/↑ | Diaphoretic | ↑ | DUMBELS/SLUDGE |
| Sedative-Hypnotic | Depressed | N/Miosis | ↓ | ↓ | ↓ | Cool | ↓ | Slurred speech |
High‑Yield Points - ⚡ Biggest Takeaways
- Alcohol withdrawal: Delirium Tremens (DTs) is life-threatening; treat with benzodiazepines (e.g., chlordiazepoxide, lorazepam).
- Opioid withdrawal: Presents with lacrimation, rhinorrhea, yawning, myalgia; naloxone for acute overdose.
- Cocaine/Amphetamine intoxication: Sympathetic overdrive (tachycardia, hypertension, agitation); manage with benzodiazepines.
- Benzodiazepine withdrawal: High risk of seizures; flumazenil for overdose (use with extreme caution).
- Cannabis intoxication: Conjunctival injection, increased appetite, altered perception; withdrawal causes irritability.
- LSD intoxication: Characterized by perceptual distortions, hallucinations, and potential flashbacks; primarily supportive care.
- Methanol poisoning: Causes visual disturbances and anion gap metabolic acidosis; treat with fomepizole or ethanol.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

