Medical Clearance: Purpose & Goals - Gatekeeper's Duty
- Purpose: Identify & stabilize acute medical conditions mimicking or worsening psychiatric symptoms.
- Goals:
- Rule out organic causes for psychiatric presentation.
- Ensure medical stability for safe psychiatric assessment/transfer.
- Prevent misdiagnosis & inappropriate psychiatric treatment.
- Avoid harm from untreated medical conditions.
- Gatekeeper's Duty:
- ED physicians/psychiatrists ensure medical stability before psychiatric disposition.
- Prioritizes patient safety; addresses medical issues first.
⭐ Up to 20-50% of patients presenting to the ED with acute psychiatric symptoms may have an underlying or contributing medical condition.
Clinical Assessment in Clearance - Detective's Toolkit
- History:
- Presenting complaint, timeline; psychiatric Hx (episodes, Rx).
- Medical Hx (comorbidities, meds); substance use (type, last use).
- 📌 AMPLE: Allergies, Medications, Past medical Hx, Last meal, Events.
- Collateral information is key.
- Physical Examination:
- Full vitals (HR, BP, RR, Temp, SpO2) for instability.
- Systemic exam: focus neuro (pupils, reflexes), CVS, respiratory.
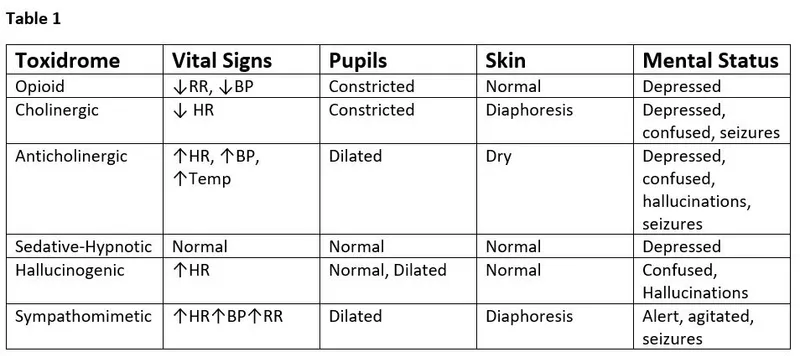
- Check for trauma, infection, toxidromes.
- Mental Status Examination (MSE):
- Appearance, behavior, psychomotor activity.
- Speech, mood, affect.
- Thought process/content (delusions, SI/HI).
- Perception (hallucinations); cognition (orientation, attention).
- Insight, judgment.
- Risk Assessment: Harm to self/others.
⭐ A comprehensive neurological exam, including assessment for subtle signs like nystagmus or ataxia, is vital in differentiating organic from functional psychiatric presentations.
Investigations for Clearance - Test Quest
⭐ Routine laboratory screening for all psychiatric patients is generally not recommended; tests should be guided by history, physical exam, and risk factors.
- Goal: Rule out medical conditions mimicking/exacerbating psychiatric symptoms.
- Basic Screen (consider if clinically indicated):
- CBC, electrolytes (Na$^+$, K$^+$, Ca$^{2+}$, Mg$^{2+}$), glucose, RFTs, LFTs, urinalysis.
- Specific Indications (tailor to presentation):
- AMS/New Psychosis: TSH, Vit B12/folate, syphilis serology, HIV; CT/MRI (focal deficits, trauma, atypical).
- Suspected Substance Use: Urine drug screen (UDS), BAL.
- Suspected Overdose: Specific drug levels (e.g., paracetamol, salicylates, lithium), ECG (cardiotoxicity).
- Fever/Suspected Infection: Blood cultures; LP (if CNS infection signs).
Organic Mimics & Red Flags - Impostor Syndromes
- Crucial: Exclude medical conditions mimicking psychiatric illness before diagnosing primary psychiatric disorder.
- Red Flags (Organic > Psychiatric):
- Acute onset, especially age >40 yrs, no prior psychiatric Hx or family Hx of psychiatric illness.
- Fluctuating level of consciousness, disorientation (time, place, person).
- Abnormal vital signs (fever, tachycardia ↑, BP ↑/↓), focal neurological signs (e.g., new weakness, reflex changes).
- Predominance of visual, tactile, or olfactory hallucinations (auditory more common in primary psychosis).
- Recent illness, head trauma, substance intoxication/withdrawal, or new medication/dosage change.
- 📌 Delirium Mnemonic: I WATCH DEATH
- Infection (UTI, pneumonia, sepsis, encephalitis)
- Withdrawal (alcohol, benzodiazepines, barbiturates)
- Acute metabolic (electrolytes ↓↑, glucose ↓↑, acidosis, alkalosis, hepatic/renal failure)
- Trauma (head injury, burns, post-operative)
- CNS pathology (stroke, seizure, tumor, hemorrhage, hydrocephalus)
- Hypoxia (anemia, CO poisoning, PE, CHF, respiratory failure)
- Deficiencies (thiamine B1, B12, niacin)
- Endocrinopathies (thyroid, adrenal, parathyroid, pituitary)
- Acute vascular (shock, hypertensive encephalopathy)
- Toxins/Drugs (anticholinergics, opioids, steroids, sedatives, illicit drugs, polypharmacy)
- Heavy metals (lead, mercury)

⭐ Visual hallucinations, especially if complex or Lilliputian (seeing small people/animals), are more strongly associated with organic brain syndromes (e.g., delirium, dementia with Lewy bodies) than with primary psychiatric disorders like schizophrenia.
High‑Yield Points - ⚡ Biggest Takeaways
- Primary goal: Exclude organic etiologies before any psychiatric diagnosis.
- Always assume underlying medical illness until proven otherwise in psychiatric emergencies.
- Essential components: Comprehensive history (collateral is vital), physical examination, vital signs, and Mental Status Examination (MSE).
- Red flags: New onset psychosis (especially in elderly), abnormal vitals, focal neurological deficits, toxidromes, and fluctuating consciousness.
- Altered Mental Status (AMS) mandates a thorough medical workup; it's rarely purely psychiatric.
- Key investigations: Include blood glucose, electrolytes, Urine Drug Screen (UDS); consider ECG, CT Head based on clinical suspicion.
- Prioritize patient and staff safety throughout the medical clearance process in the emergency setting.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

