Introduction & Etiology - Psychosis Unveiled
- Psychosis: Acute syndrome; loss of reality contact. Manifests as hallucinations (esp. auditory), delusions, disorganized thought/speech/behavior. A psychiatric emergency.
- Etiology (Triad):
- Primary Psychiatric: Schizophrenia, Bipolar I (mania), Brief Psychotic Disorder.
- Substance-Induced: Alcohol (withdrawal), Cannabis, Stimulants (e.g., amphetamine).
- Organic/Medical (Secondary):
- CNS: Infections (encephalitis), trauma, tumor, epilepsy.
- Metabolic: Hypoglycemia, uremia, hepatic encephalopathy.
- Endocrine: Thyroid storm, Cushing's.
- Autoimmune: Anti-NMDA Receptor Encephalitis.
⭐ Delirium can mimic psychosis; always rule out organic causes first in new-onset psychosis, especially in elderly or medically ill.
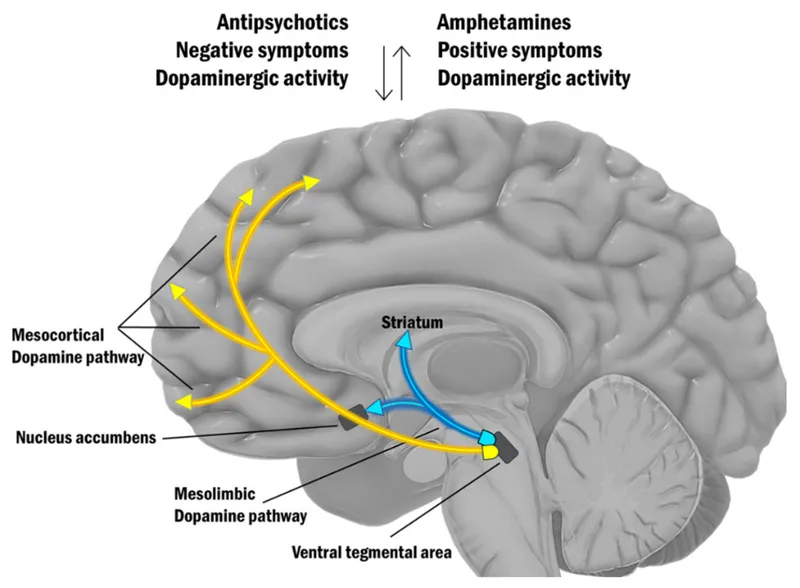
- Pathophysiology: Primarily ↑ dopamine in mesolimbic pathway.
 oka
oka
Clinical Features - Mind in Turmoil
- Perception: Hallucinations (auditory most common; e.g., voices commenting, commanding).
- Thought Content: Delusions (fixed, false beliefs; e.g., persecutory, grandiose, referential).
- Thought Form/Stream: Disorganized speech (e.g., flight of ideas, tangentiality, incoherence, thought block).
- Behavior: Agitation, aggression, unpredictable actions, bizarre posturing, catatonic features (stupor, excitement), poor self-care.
- Mood & Affect: Incongruent affect, labile mood, perplexity, fear, irritability.
- Insight & Judgment: Markedly impaired insight (unawareness of illness); poor judgment leading to risk.
⭐ Auditory hallucinations, especially third-person (voices discussing patient) or thought echo, are highly suggestive of schizophrenia-spectrum psychosis but can occur in other psychoses too.
Differential Diagnosis - Spotting the Mimics
Acute psychosis requires rapid exclusion of organic causes.
- 📌 Key Red Flags for Organic Cause:
- Sudden onset, age >40
- Fluctuating sensorium (delirium)
- Abnormal vitals, neuro deficits
- Substance use, new meds
- No prior psych history
⭐ New-onset psychosis in older adults or with atypical features (visual hallucinations, cognitive issues) strongly suggests an organic cause.
Investigations - Unmasking the Truth
- Goals: Rule out organic causes, establish baseline.
- Core Bloods & Urine:
- CBC, inflammatory markers (ESR, CRP)
- RFT, LFT, electrolytes, glucose
- TFTs
- Urine R/M, Urine Drug Screen (UDS)
- Essential: ECG (baseline QTc).
- Neuroimaging (CT/MRI): If:
- First episode psychosis
- Focal neurological deficits
- Head trauma, atypical course
- Targeted (if suspected):
- EEG (seizures)
- LP (CNS infection)
- Serology (HIV, VDRL), Vit B12/Folate
⭐ Neuroimaging (CT/MRI) is crucial in first-episode psychosis to exclude structural brain pathology.
Emergency Management - Calming the Storm
- Safety First: Ensure safety (patient, staff). Verbal de-escalation. Low-stimulus environment.
- Medical Assessment: Rule out organic causes (📌 DIMS: Drugs, Infection, Metabolic, Structural). Check vitals, glucose, O2 sat. Labs: electrolytes, tox screen. Consider ECG, CT head.
- Rapid Tranquilization (RT): If de-escalation fails/danger.
- Oral (cooperative): Risperidone 1-2mg / Olanzapine 5-10mg.
- IM (agitation): Lorazepam 2-4mg; Haloperidol 5mg; Olanzapine 5-10mg.
- Combination (e.g., Haloperidol 5mg + Lorazepam 2mg IM) effective.
- Physical Restraints: Last resort for safety. Monitor closely. Document.
⭐ Always prioritize excluding reversible medical/toxic causes of psychosis before initiating antipsychotics if the clinical picture is unclear.
High‑Yield Points - ⚡ Biggest Takeaways
- Always rule out organic causes (delirium, substances, medical illness) first in acute psychosis.
- Patient and staff safety is paramount; use rapid tranquilization (e.g., haloperidol, olanzapine) for severe agitation.
- Distinguish from delirium: psychosis has clear sensorium, delirium has fluctuating consciousness.
- Schneiderian first-rank symptoms strongly suggest schizophrenia but are not pathognomonic.
- Monitor for antipsychotic side effects: acute dystonia, akathisia, NMS.
- Duration is key: Brief Psychotic Disorder (<1 month), Schizophreniform (1‑6 months).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

