CBT Fundamentals - Mind Over Mood
- Definition: Structured psychotherapy focused on identifying and changing unhelpful thinking patterns (cognitions) and behaviors to alleviate emotional distress.
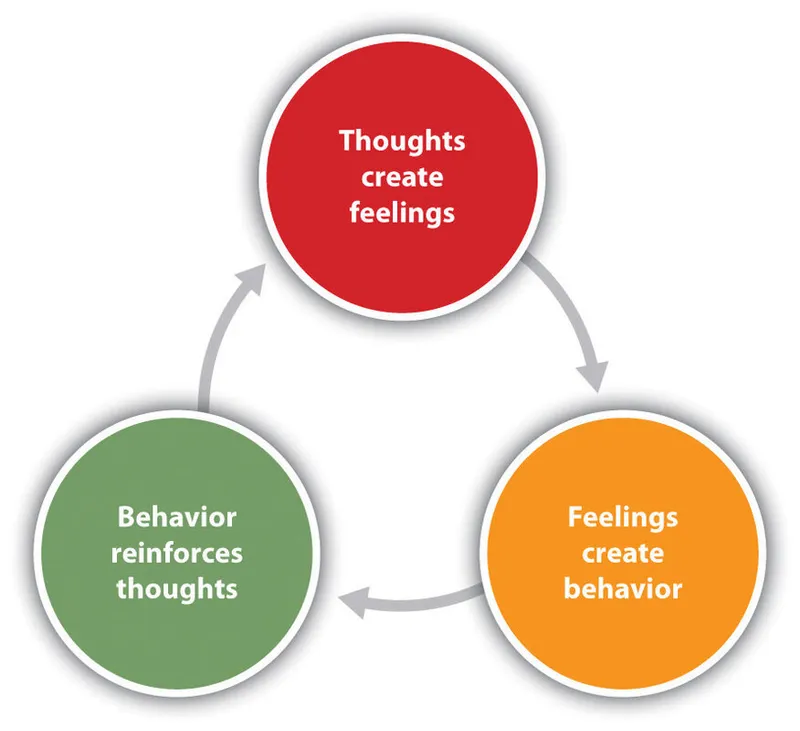
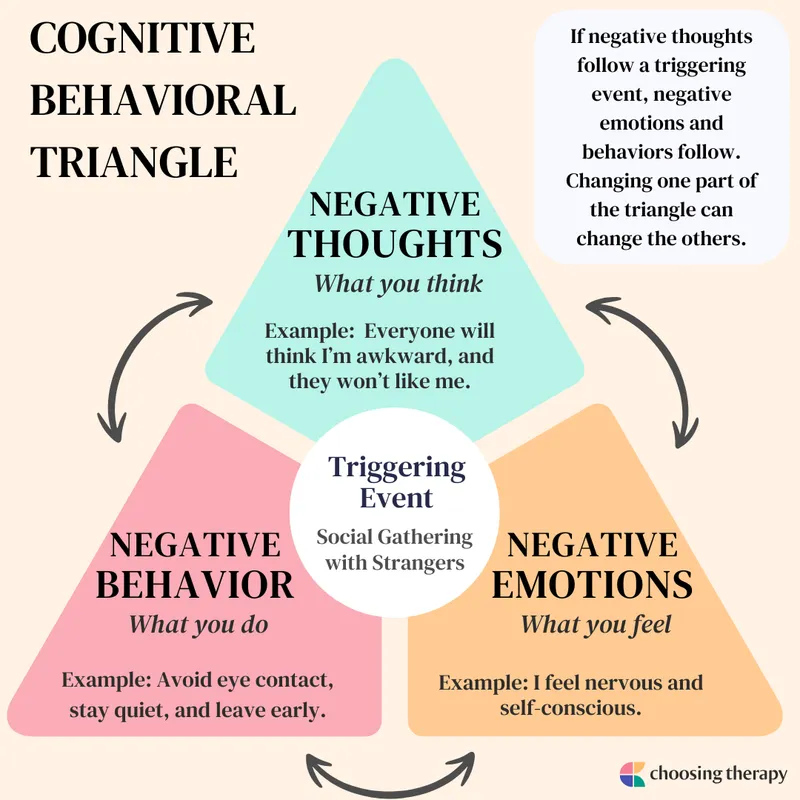
- Cognitive Model (Beck): Proposes that thoughts, feelings, and behaviors are interconnected and influence each other.
- Situation → Thoughts → Emotions → Behaviors → Physical Sensations (cycle).
- Maladaptive thoughts (e.g., catastrophizing, overgeneralization) are key targets.
- Goals in Anxiety:
- Identify & challenge cognitive distortions contributing to anxiety.
- Modify avoidance and safety-seeking behaviors.
- Develop adaptive coping strategies & problem-solving skills.
- Reduce physiological arousal and subjective distress.
⭐ CBT's primary focus is on the 'here and now', addressing current distressing symptoms and maladaptive patterns rather than extensive exploration of the past.
CBT Techniques - Anxiety Busters
Core strategies to manage anxiety by modifying thoughts and behaviors.
- Cognitive Restructuring:
- Identify & challenge negative automatic thoughts (NATs).
- Use thought records: Situation → Thought → Emotion → Evidence → Balanced thought.
- 📌 Socratic questioning helps uncover and dispute cognitive distortions (e.g., catastrophizing, overgeneralization).
- Exposure Therapy: Gradually confront feared stimuli.
- Develop an exposure hierarchy (least to most anxiety-provoking).
- Types:
- In vivo: Real-life exposure.
- Imaginal: Vividly imagining the feared situation.
- Interoceptive: Inducing feared physical sensations (e.g., for panic disorder).
⭐ Exposure with Response Prevention (ERP) is the cornerstone of CBT for Obsessive-Compulsive Disorder (OCD).
- Behavioral Experiments: Test the validity of anxious predictions in real-life situations.
- Relaxation Techniques:
- Progressive Muscle Relaxation (PMR).
- Diaphragmatic (deep) breathing.
- Problem-Solving Skills: Define problem → Generate solutions → Implement → Evaluate.
- Homework: Crucial for generalizing skills learned in therapy to daily life.
Disorder-Specific CBT - Tailored Tactics
⭐ Interoceptive exposure is particularly useful for Panic Disorder.
| Disorder | Core CBT Focus | Primary Techniques |
|---|---|---|
| GAD | Managing persistent, excessive worry; Modifying beliefs about worry's utility; Increasing uncertainty tolerance. | Worry exposure (imaginal/in-vivo); Cognitive restructuring; Problem-solving training; Relaxation techniques. |
| Panic Disorder | Reducing fear of panic attacks & physical sensations; Correcting catastrophic misinterpretations of these sensations. | Interoceptive exposure (to feared bodily sensations); Cognitive restructuring (of "dying/losing control" thoughts). |
| Social Anxiety Disorder (SAD) | Overcoming intense fear of social scrutiny/negative evaluation; Reducing associated avoidance & safety behaviors. | Graded exposure to feared social situations; Cognitive restructuring (of negative self-beliefs); Safety behavior elimination. |
| Specific Phobias | Extinguishing the intense, irrational fear response to a specific object or situation; Relearning safety. | Systematic desensitization (pairing relaxation with graded exposure); In-vivo exposure; Participant modeling. |
CBT Efficacy & Nuances - Proven Power
- Strong evidence base: First-line therapy for many anxiety disorders (e.g., GAD, Panic Disorder, Social Anxiety, PTSD, OCD).
- Relapse prevention: Equips patients with durable coping skills, reducing recurrence.
- Common challenges: Requires patient motivation and consistent homework completion.
- Indian context: Adaptations for cultural nuances and resource availability are key.
⭐ CBT has demonstrated long-lasting effects, often persisting even after therapy termination.
High‑Yield Points - ⚡ Biggest Takeaways
- CBT identifies and modifies maladaptive thoughts & behaviors perpetuating anxiety.
- Core techniques: exposure therapy (for phobias, panic) and cognitive restructuring.
- Homework is vital for generalizing skills and ensuring treatment success.
- First-line treatment for GAD, Panic Disorder, Social Anxiety, PTSD, and OCD.
- Typically structured and time-limited (e.g., 12-20 sessions), focusing on current issues.
- Exposure and Response Prevention (ERP) is the CBT cornerstone for OCD.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

