Definition & Classification - Degrees of Chill
- Hypothermia: Core body temperature (CBT) falls below 35°C (95°F).
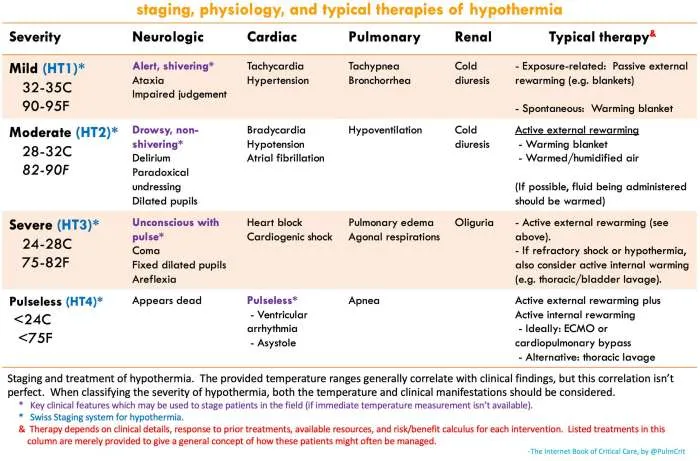
- Classification by Severity (Degrees):
- Mild: 32-35°C (90-95°F)
- Features: Max. shivering, confusion, ataxia, tachycardia.
- Moderate: 28-32°C (82-90°F)
- Features: Shivering stops, ↓level of consciousness, bradycardia, arrhythmias.
- Severe: < 28°C (< 82°F)
- Features: Unconsciousness, vital signs barely detectable, risk of VF/asystole.
- Mild: 32-35°C (90-95°F)
⭐ Osborn J wave (late delta wave or camel-hump sign) on ECG is characteristic in moderate hypothermia (28-32°C).
Pathophysiology - Systemic Slowdown
Global ↓ metabolic rate & organ function from progressive cooling.
- Key Mechanism: ↓ Temperature → ↓ Enzyme activity ($Q_{10}$ effect: rate ≈halves per 10°C drop).
- CNS Depression: ↓ Neural metabolism → Confusion, lethargy, coma.
- Cardiovascular Effects:
- Initial brief tachycardia → Bradycardia, ↓ Contractility, ↓ Cardiac Output (CO).
- ↑ Myocardial irritability → Arrhythmias (Atrial Fibrillation, Ventricular Fibrillation, Asystole).
- ECG: Osborn J wave (esp. <32°C), prolonged PR, QRS, QT intervals.
- Respiratory Depression: ↓ Central drive → Hypoventilation, CO₂ retention, respiratory acidosis. ↓ Airway reflexes.
- Renal Dysfunction: "Cold diuresis" (impaired ADH effect & tubular function) → Hypovolemia.
- Hematologic Changes: ↑ Blood viscosity, platelet dysfunction, impaired coagulation enzyme activity → Bleeding risk.
- Metabolic: ↓ O₂ consumption, ↓ ATP production. Hyperglycemia (due to ↓ insulin release & sensitivity).
⭐ Osborn J waves (positive deflection at QRS-ST junction) are characteristic ECG findings in hypothermia, typically appearing when core temperature drops below 32°C (89.6°F).
Clinical Features & Diagnosis - Icy Indicators
- Core Temperature is Key: Low-reading thermometer (rectal, esophageal).
- Stages (Core Temp):
- Mild (32-35°C): Shivering, ↑HR, ↑BP, ↑RR. Confusion, ataxia (📌 "umbles"). Cold diuresis.
- Moderate (28-32°C): Shivering stops. ↓HR, ↓BP, ↓RR. Stupor. Osborn J wave on ECG. Arrhythmias (AF).
- Severe (<28°C): Coma. Profound bradycardia/hypotension. VF/Asystole risk. Areflexia.
⭐ Osborn J wave (camel hump) on ECG is characteristic, best in precordial leads.
- ECG:
- Osborn J wave (positive deflection at QRS-ST junction).
- Bradycardia, prolonged PR, QRS, QT intervals.
- Arrhythmias: AF, VF, Asystole.
- Labs:
- Acidosis (metabolic/respiratory).
- ↑ Hct (hemoconcentration).
- Electrolyte shifts (K+ variable; ↑K+ in severe = poor prognosis).
- Coagulopathy.
Management & Complications - Thawing Tactics & Threats
Management (Thawing):
- Core: ABCs, remove wet, insulate.
- Rewarming by Severity (Core Temp T):
- Mild (T >32°C): Passive external (blankets).
- Moderate (T 28-32°C): Active external (forced air; trunk first to avoid afterdrop ⚠️).
- Severe (T <28°C / unstable): Active internal (warm IV fluids 40-42°C, warm O2, lavage; ECMO/CPB if arrest/refractory).
- CPR: Continue if arrested. Defib/drugs often fail if T <30°C.
Complications (Threats):
- Rewarming: Afterdrop, shock (hypotension).
- Cardiac: Osborn J wave, AF, VT/VF (refractory <30°C).
- Metabolic: ↓K+, ↓Mg++, glucose dysregulation.
- Systemic: Coagulopathy, rhabdomyolysis, ARDS.
⭐ VF in hypothermia is often refractory to defibrillation until core temp >30°C.
High‑Yield Points - ⚡ Biggest Takeaways
- Hypothermia: Core body temperature <35°C (95°F).
- Stages: Mild (32-35°C), Moderate (28-32°C), Severe (<28°C). Shivering stops below 30-32°C.
- ECG: Osborn J wave (pathognomonic), bradycardia, prolonged intervals (PR, QRS, QT), risk of Ventricular Fibrillation.
- Rewarming: Passive external for mild; active core rewarming (warm IV fluids, lavage) for moderate/severe.
- Paradoxical undressing and terminal burrowing are behavioral changes in severe hypothermia.
- Complications: Arrhythmias, rhabdomyolysis, coagulopathy, ARDS, pancreatitis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

