RFTs Overview - Lung Checkup Basics
Respiratory Function Tests (RFTs) are essential non-invasive tools for evaluating lung health and function.
- Purpose of RFTs:
- Diagnosis (e.g., asthma, COPD).
- Monitoring disease progression & therapy.
- Pre-operative risk assessment.
- Classification (Key Types):
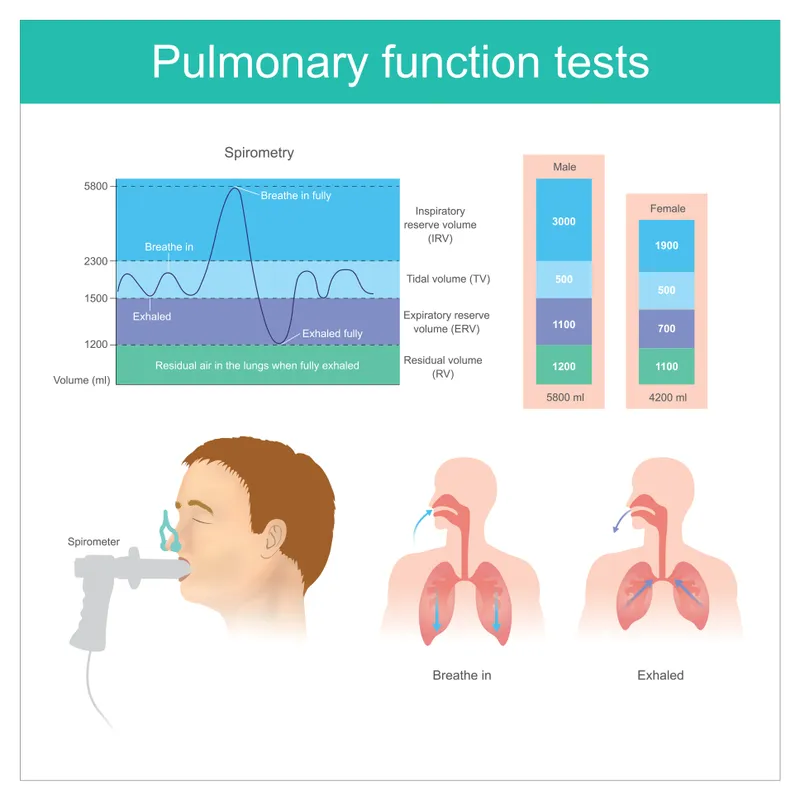
- Spirometry: measures airflow.
- Lung Volumes: measures air capacity (e.g., TLC, RV).
- Diffusion Capacity (DLCO): assesses gas exchange.
- ABGs: evaluate $O_2$/$CO_2$ levels.
- Exercise Tests (CPET): assess exercise capacity.
⭐ RFTs are non-invasive tests crucial for differentiating obstructive vs. restrictive lung diseases.
Spirometry - Airflow Adventures
Key Spirometry Measures:
- FVC (Forced Vital Capacity): Max air exhaled post max inspiration.
- FEV1 (Forced Expiratory Volume in 1s): Air exhaled in 1st second.
- FEV1/FVC Ratio: Key. Normal >0.7-0.8. $FEV_1/FVC < \textbf{0.7}$ (or 70%) = Obstruction.
- PEFR (Peak Expiratory Flow Rate): Max expiratory speed.
- FEF25-75%: Mid-flow; small airways.
Flow-Volume Loops:
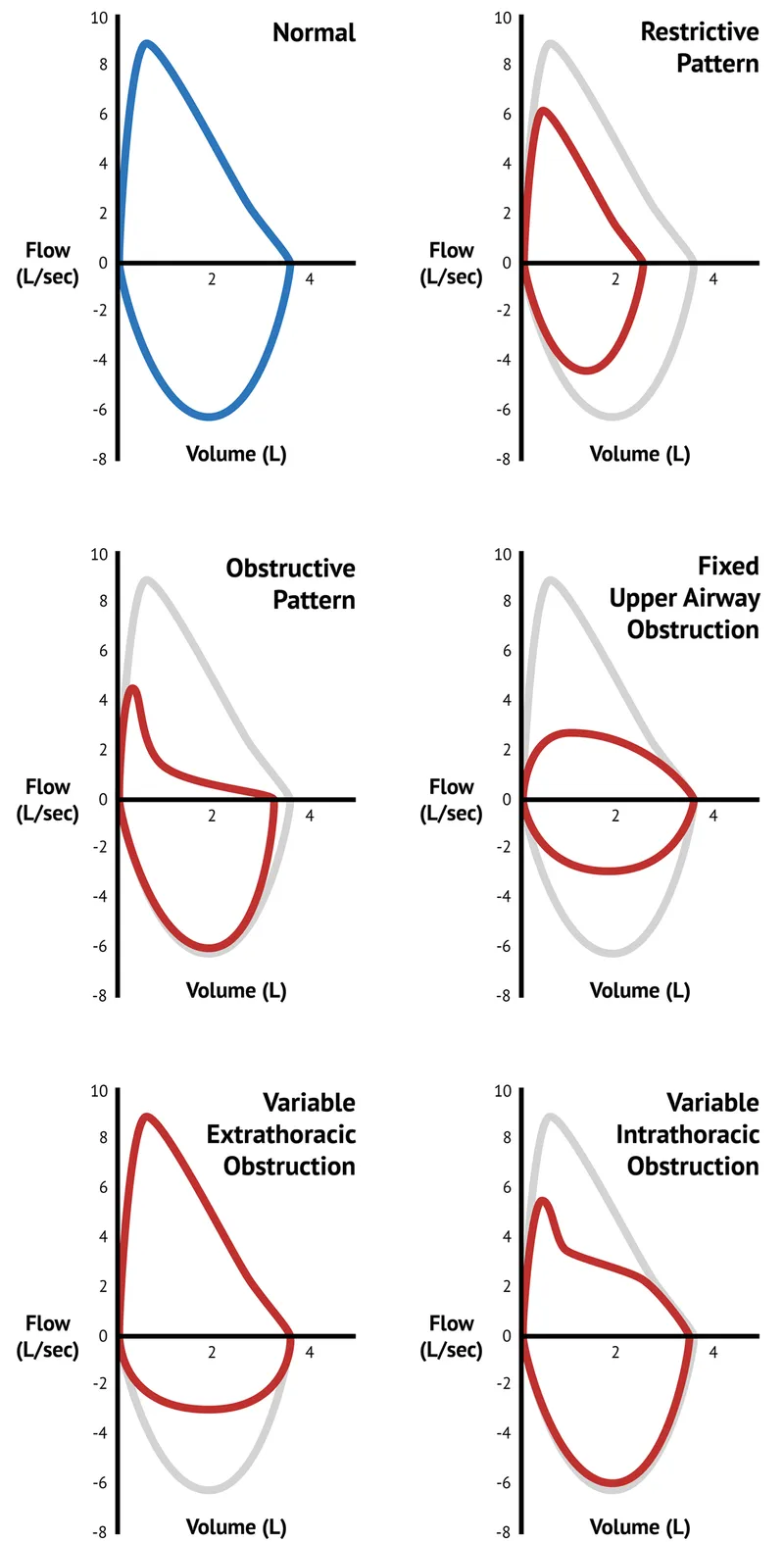
- 📌 Obstructive: 'Scooped-out' appearance. Restrictive: Narrow, tall "witch's hat".
Interpreting Patterns: Severity of obstruction is graded by FEV1 %predicted (e.g., Mild >70%, Moderate 60-69%, Severe 35-49%).
| Feature | Obstructive (Asthma, COPD) | Restrictive (Fibrosis, Chest Wall Dx) |
|---|---|---|
| FEV1 | ↓↓ | ↓ |
| FVC | Normal / ↓ | ↓↓ |
| FEV1/FVC Ratio | ↓ ($< \textbf{0.7}$) | Normal / ↑ |
Spirometry Interpretation Algorithm:
Lung Volumes & Capacities - Air Space Sizing
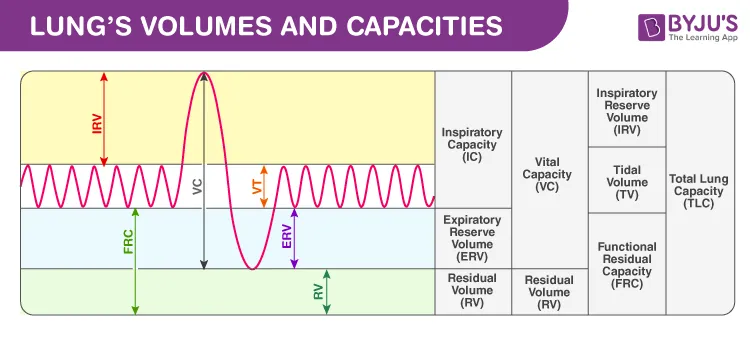
- Lung Volumes (Static):
- Tidal Volume (TV): Air per quiet breath; ~500 mL.
- Inspiratory Reserve Volume (IRV): Max extra air inhaled after normal inspiration; ~3000 mL.
- Expiratory Reserve Volume (ERV): Max extra air exhaled after normal expiration; ~1100 mL.
- Residual Volume (RV): Air left in lungs after max exhalation; ~1200 mL. (Not measured by spirometry)
- Lung Capacities (Combinations of ≥2 volumes):
- Inspiratory Capacity (IC): $IC = TV + IRV$; ~3500 mL.
- Functional Residual Capacity (FRC): $FRC = ERV + RV$; ~2300 mL. (Lung volume at rest)
- Vital Capacity (VC): $VC = IRV + TV + ERV$; ~4600 mL.
- Total Lung Capacity (TLC): $TLC = RV + ERV + TV + IRV$; ~5800 mL. (TLC < 80% predicted: Restriction)
- FRC & RV Measurement Methods:
- Helium dilution technique
- Nitrogen washout method
- Body Plethysmography
⭐ Body plethysmography measures total thoracic gas, including trapped gas (e.g., in bullae), making it the gold standard for FRC & TLC measurement.
DLCO & Specialized Tests - Gas Exchange & Challenges
-
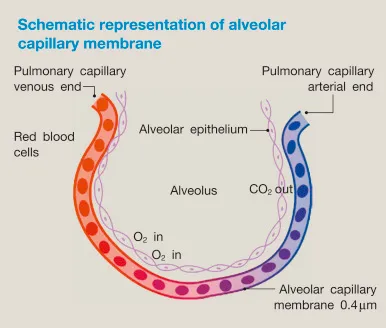
Diffusing Capacity (DLCO/TLCO): Measures gas transfer across alveolo-capillary membrane.
- Principle: CO uptake reflects O₂ exchange. $V_{gas} = \frac{A \cdot D_M \cdot (P_1 - P_2)}{T}$.
- Abnormal: < 80% predicted.
- Factors affecting DLCO:
- ↓ DLCO: Anemia, emphysema (↓area), ILD (↑thickness), pulmonary embolism (↓blood flow), smoking (↑COHb).
- ↑ DLCO: Polycythemia, pulmonary hemorrhage, exercise, asthma (can be normal/↑).
 ⭐ > DLCO ↓ in emphysema (alveolar destruction), often normal/↑ in asthma & chronic bronchitis (without emphysema).
⭐ > DLCO ↓ in emphysema (alveolar destruction), often normal/↑ in asthma & chronic bronchitis (without emphysema).
-
Bronchodilator Reversibility Test:
- For asthma diagnosis/assessment.
- Significant response: Post-bronchodilator FEV₁ or FVC ↑ > 12% AND > 200mL.
-
Bronchoprovocation Test (e.g., Methacholine Challenge):
- Diagnoses airway hyperresponsiveness (AHR), e.g., in asthma.
- Positive: FEV₁ ↓ by 20% (PC₂₀) at low agonist concentration.
High‑Yield Points - ⚡ Biggest Takeaways
- FEV1/FVC ratio is key: ↓ in obstructive, normal/↑ in restrictive diseases.
- DLCO (diffusing capacity) is ↓ in emphysema and most ILDs.
- Spirometry measures dynamic lung volumes (FVC, FEV1) and flow rates.
- RV & TLC are ↑ in obstructive (air trapping), ↓ in restrictive patterns.
- Flow-volume loops: characteristic scooped (obstructive), miniature (restrictive), or flattened (fixed obstruction) patterns.
- Bronchodilator reversibility (FEV1 ↑ >12% & >200mL) suggests asthma.
- Methacholine challenge assesses bronchial hyperresponsiveness in suspected asthma_._
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

