Pressures & Mechanics - Boyle's Beatbox
- Boyle's Law: $P_1V_1 = P_2V_2$. Air flows from high to low pressure. 📌 Boyle's Beatbox: ↑Volume, ↓Pressure.
- Key Pressures (relative to Atmospheric $0 \text{ cm H}_2\text{O}$):
- Intra-alveolar (Palv):
- Inspiration: $-1 \text{ cm H}_2\text{O}$
- Expiration: $+1 \text{ cm H}_2\text{O}$
- Intrapleural (Pip): Normally $-5 \text{ cm H}_2\text{O}$.
- Inspiration: Becomes more negative (e.g., $-7.5 \text{ cm H}_2\text{O}$).
⭐ Intrapleural pressure is always negative during quiet breathing, becoming more negative during inspiration.
- Transpulmonary (Ptp): $P_{tp} = P_{alv} - P_{ip}$. Keeps alveoli open.
- Intra-alveolar (Palv):
- Mechanics of Breathing:
- Inspiration (Active): Diaphragm & external intercostals contract → ↑ Thoracic volume → ↓Palv → Air in.
- Expiration (Passive): Muscle relaxation, elastic recoil → ↓ Thoracic volume → ↑Palv → Air out.
Lung Volumes & Capacities - Spiro Squad
Spirometry measures lung air movement, key for diagnosis.
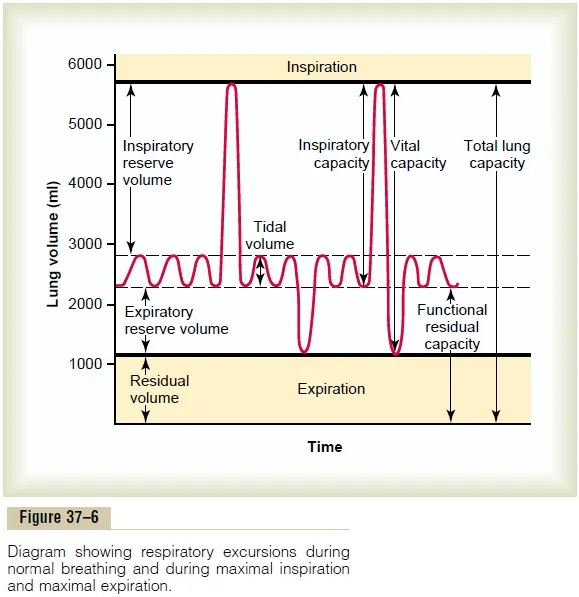
Lung Volumes:
- Tidal Volume (TV): Air/quiet breath. ~500 mL.
- Inspiratory Reserve Volume (IRV): Max air inhaled beyond TV. ~3000 mL.
- Expiratory Reserve Volume (ERV): Max air exhaled beyond TV. ~1100 mL.
- Residual Volume (RV): Air in lungs after max exhale. ~1200 mL.
Lung Capacities:
- Inspiratory Capacity (IC): Max air inhaled from FRC start. $IC = TV + IRV$. ~3500 mL.
- Functional Residual Capacity (FRC): Air in lungs after normal exhale. $FRC = ERV + RV$. ~2300 mL.
- Vital Capacity (VC): Max air exhaled after max inhale. $VC = IRV + TV + ERV$. ~4600 mL.
- Total Lung Capacity (TLC): Total air in lungs after max inhale. $TLC = VC + RV$. ~5800 mL.
📌 Residual Volume & capacities with it (FRC, TLC) Can't Measure Simply (via spirometry).
⭐ Functional Residual Capacity (FRC) cannot be measured by simple spirometry as it includes Residual Volume (RV).
Compliance & Resistance - Elastic Airflow
- Compliance (C): Lung distensibility. $C = \Delta V / \Delta P$.
- ↑C: Emphysema, aging.
- ↓C: Fibrosis, edema, ARDS, ↓surfactant.
- Specific Compliance: $C / \text{FRC}$.
- Surface Tension & Surfactant:
- Alveolar surface tension (Laplace: $P = 2T/r$) promotes collapse.
- Surfactant (Type II pneumocytes; DPPC): ↓Surface tension, ↑C, prevents atelectasis.
⭐ Surfactant, produced by Type II pneumocytes, reduces surface tension and increases lung compliance, preventing alveolar collapse.
- Airway Resistance (R): Opposition to airflow. $R = \Delta P / \dot{V}$.
- Poiseuille's Law: $R \propto \eta L / r^4$. Radius (r) is key (📌 Radius Rules Resistance).
- Major site: Medium-sized bronchi.
- ↑R: Bronchoconstriction (asthma, parasymp.), mucus, ↓lung volume.
- ↓R: Bronchodilation (symp.), ↑lung volume (radial traction).
Work & Dead Space - Effort & Empties
- Work of Breathing (WOB): Energy for lung inflation (overcomes elastic recoil, airway resistance).
- ↑ WOB: Restrictive (fibrosis), Obstructive (asthma, COPD).
- O2 cost: 1-3% of total O2 consumption; ↑ to 25-30% (disease/exercise).
- Dead Space (DS): Air not participating in gas exchange.
- Anatomical DS (ADS): Volume of conducting airways; ~150 \text{ mL} (or ~2 \text{ mL/kg}).
- Alveolar DS: Volume of alveoli ventilated but not perfused; ↑ in V/Q mismatch.
- Physiological DS (PDS): Sum of ADS + Alveolar DS. 📌 PADS. Bohr's equation: $V_D/V_T = (P_aCO_2 - P_ECO_2) / P_aCO_2$.
- Alveolar Ventilation ($V_A$): Volume of fresh air for gas exchange. $V_A = (\text{Tidal Volume } V_T - \text{Dead Space } V_D) \times \text{Respiratory Rate (RR)}$.

⭐ Physiological dead space approximates anatomical dead space in healthy individuals but increases significantly in lung diseases with V/Q mismatch (e.g., pulmonary embolism, emphysema).
High‑Yield Points - ⚡ Biggest Takeaways
- Normal quiet inspiration: driven by diaphragm contraction and external intercostals.
- Forced inspiration: uses accessory muscles like scalenes and sternocleidomastoids.
- Forced expiration: an active process using abdominal and internal intercostal muscles.
- Intrapleural pressure: always negative relative to atmosphere, preventing lung collapse.
- Surfactant (Type II pneumocytes): reduces alveolar surface tension, increasing compliance.
- Airway resistance: highest in medium-sized bronchi, not the smallest airways.
- Lung compliance: lung's distensibility; increased in emphysema, decreased in fibrosis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

