Muscles & Pressures - Pressure Players
-
Inspiratory Muscles:
- Principal: Diaphragm (main, flattens), External Intercostals (elevate ribs).
- Accessory (forced): SCM, Scalenes, Pectoralis.
-
Expiratory Muscles:
- Quiet: Passive (elastic recoil).
- Forced: Internal Intercostals, Abdominal muscles.
-
Key Pressures (relative to Patm = 0 cm H₂O):
- Palv (Intra-alveolar): Airflow driver. Inspiration -1, Expiration +1 cm H₂O.
- Pip (Intrapleural): Pressure in pleural cavity; crucial for lung inflation.
⭐ Intrapleural pressure is normally negative (approx. -5 cm H₂O at end-expiration, -8 cm H₂O at end-inspiration) due to opposing elastic recoils of lung and chest wall.
- Ptp (Transpulmonary): $P_{tp} = P_{alv} - P_{ip}$. Alveolar distending pressure.
Lung Volumes & Capacities - Breath by Numbers
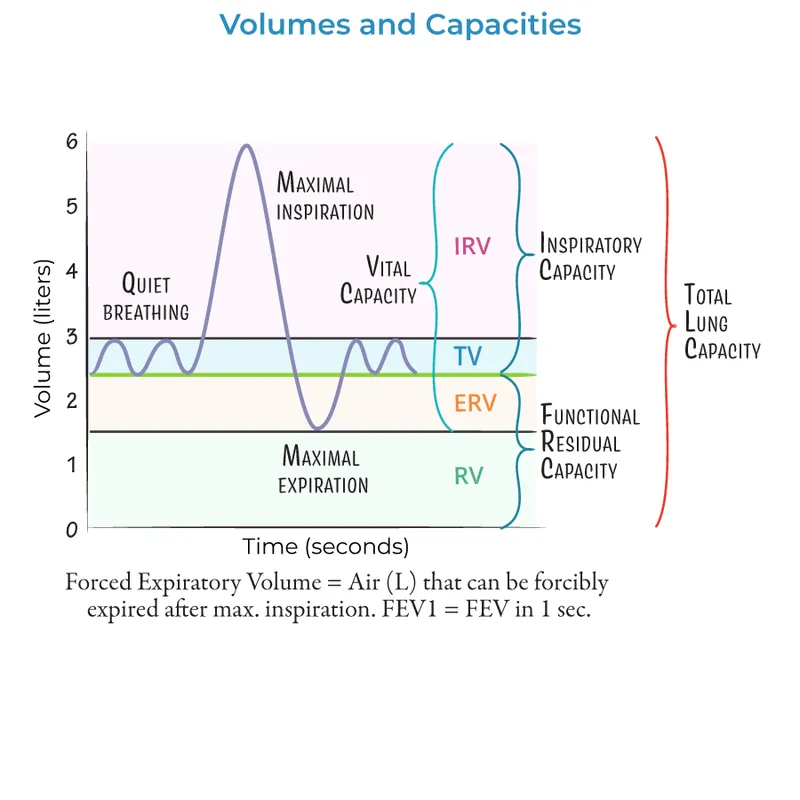
- Volumes:
- Tidal Volume (TV): Air/quiet breath; ~500 mL.
- Inspiratory Reserve (IRV): Max extra air inhaled; ~3000 mL.
- Expiratory Reserve (ERV): Max extra air exhaled; ~1100 mL.
- Residual Volume (RV): Air left after max exhale; ~1200 mL.
- Capacities: (Sums of volumes) 📌 Mnemonic: "Can I Find Vitality Today?" (IC, FRC, VC, TLC)
- Inspiratory (IC): $TV + IRV$; ~3500 mL.
- Functional Residual (FRC): $ERV + RV$; ~2300 mL.
- Vital (VC): $IRV + TV + ERV$; ~4600 mL.
- Total Lung (TLC): $VC + RV$; ~5800 mL.
⭐ Residual Volume (RV), Functional Residual Capacity (FRC), and Total Lung Capacity (TLC) cannot be measured by simple spirometry; require helium dilution or body plethysmography.
Lung Compliance & Surfactant - Stretch & Snap
- Lung Compliance ($C_L$): Lung/chest wall stretchability. $C_L = \Delta V / \Delta P$.
- Normal (lungs): ~200 mL/cm H₂O.
- ↑ $C_L$: Emphysema, aging (easier inflation).
- ↓ $C_L$: Fibrosis, edema, ARDS, NRDS (stiffer lungs).
- Elastic Recoil: Lungs' tendency to deflate post-stretch; opposes compliance.
- Surface Tension: Alveolar air-liquid interface force causing collapse.
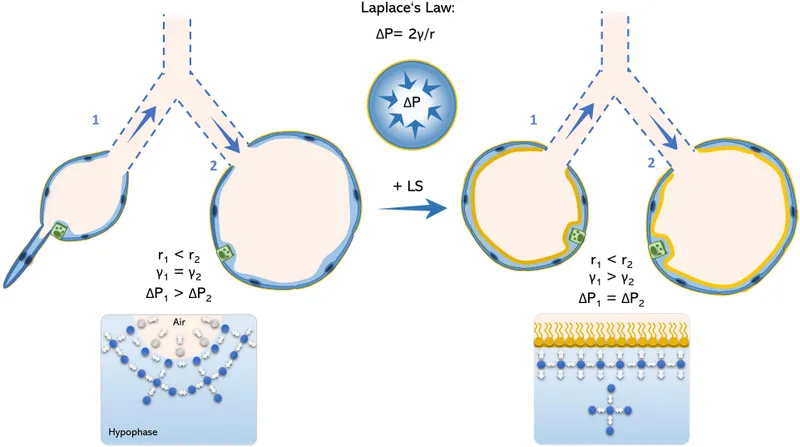
- Laplace's Law: $P = 2T/r$. Smaller alveoli = ↑ collapse risk.
- Pulmonary Surfactant:
- From Type II pneumocytes; main: Dipalmitoylphosphatidylcholine (DPPC).
- Action: ↓ surface tension (esp. small alveoli), ↑ compliance, prevents atelectasis.
- Deficiency: Neonatal RDS.
⭐ Surfactant (DPPC) reduces surface tension more effectively in smaller alveoli (greater concentration as surface area ↓), preventing collapse, per Laplace's Law ($P = 2T/r$).
Airway Resistance & Work - Flow & Force
- Airway Resistance (Raw): Opposition to airflow. $Raw = \frac{\Delta P}{\dot{V}}$ (Pressure gradient / Flow rate).
- Poiseuille's Law: $R \propto \frac{\eta l}{r^4}$; radius ($r$) is dominant. $\eta$=viscosity, $l$=length.
- $\downarrow$Radius (e.g., bronchoconstriction, mucus) $\rightarrow$ significantly $\uparrow$Raw.
- $\uparrow$Lung Volume $\rightarrow$ $\downarrow$Raw (radial traction on airways).
- Flow types: Laminar (smooth, low Raw), Turbulent (disordered, $\uparrow$Raw, e.g., trachea, high flow rates). Reynolds number ($Re$) predicts turbulence.
- Work of Breathing (WOB): Energy expended for ventilation. $W = P \times \Delta V$.
- Components: Elastic work (to overcome lung/chest wall recoil) & Resistive work (to overcome Raw).
- $\uparrow$Elastic work in restrictive diseases (e.g., fibrosis).
- $\uparrow$Resistive work in obstructive diseases (e.g., asthma, COPD).
- $O_2$ cost of breathing: Normally ~1-2% of total $O_2$ consumption; can $\uparrow$ significantly in respiratory disease.
⭐ The medium-sized bronchi (generations 2-5) are the major site of airway resistance, not the smallest airways, because of their summated smaller cross-sectional area compared to the numerous terminal bronchioles in parallel.
High‑Yield Points - ⚡ Biggest Takeaways
- Inspiration: active process (diaphragm, external intercostals).
- Expiration: normally passive (elastic recoil); forced uses internal intercostals, abdominals.
- Intrapleural pressure: always negative, crucial for lung expansion.
- Surfactant (DPPC): ↓ surface tension, prevents alveolar collapse, ↑ compliance. Deficiency causes RDS.
- Lung compliance: ↑ in emphysema, ↓ in fibrosis/edema.
- Airway resistance: highest in medium-sized bronchi.
- Work of breathing: ↑ with ↓ compliance or ↑ resistance.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

