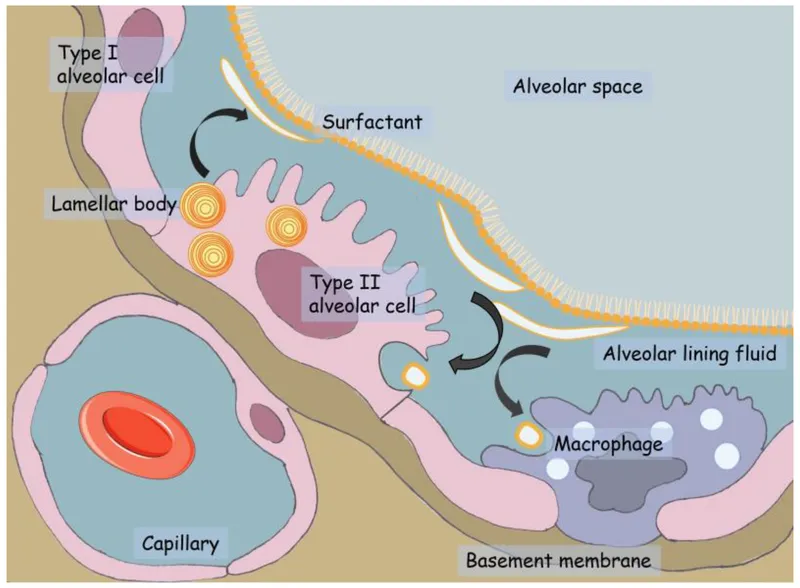
Alveolar-Capillary Membrane - The Thin Red Line
- Primary site of O₂/CO₂ exchange between alveolar air and pulmonary capillary blood.
- Extremely thin barrier (~0.5 µm) facilitating rapid diffusion.
- Composed of three main layers:
- Alveolar epithelium (squamous Type I pneumocytes)
- Fused basal laminae of alveolar and capillary endothelial cells
- Capillary endothelium
- Vast total surface area for gas exchange (approx. 50-100 m²).
- Gas transfer rate follows Fick's Law: $V_{gas} \propto \frac{A \cdot D \cdot \Delta P}{T}$.
⭐ The integrity and minimal thickness of the alveolar-capillary membrane are crucial; conditions like pulmonary fibrosis or edema increase its thickness, impairing gas exchange.
Diffusion Principles - Gas Go Flow
- Gas transfer via passive diffusion, driven by partial pressure gradient $(P_1 - P_2)$.
- Fick's Law: $V_{gas} \propto \frac{A \times D \times (P_1 - P_2)}{T}$
- Factors: 📌 Area, Diff. Coeff, Pressure gradient, Thickness (inverse).
- ↑$A$, ↑$(P_1 - P_2)$, ↑$D$ → ↑$V_{gas}$; ↑$T$ → ↓$V_{gas}$.
- Diffusion Coefficient (D): $D \propto \frac{Sol}{\sqrt{MW}}$ ($Sol$: Solubility, $MW$: Molecular Weight).
- CO2 diffuses ~20x faster than O2 (due to ↑↑ $Sol$).
⭐ CO2 diffuses ~20x faster than O2 across the alveolar membrane due to much higher solubility, despite its larger MW.
Partial Pressures & Gradients - Pressure Play
- Gases move via partial pressure ($P_x$) gradients ($\Delta P$): High $P_x$ → Low $P_x$.
- Dalton's Law: Total pressure = $\Sigma P_x$. $P_x$ = Total Pressure $\times$ Fractional concentration.
- Key Pressures (mmHg):
- Inspired: $P_{O_2}$ ~160
- Alveolar ($P_A$): $O_2$ 100-104; $CO_2$ 40
- Venous ($P_v$): $O_2$ 40; $CO_2$ 45
- Arterial ($P_a$): $O_2$ 95-100; $CO_2$ 40
- $O_2$ Gradient (Alveoli→Blood): 104 ($P_A O_2$) - 40 ($P_v O_2$) $\approx$ 64 mmHg.
- $CO_2$ Gradient (Blood→Alveoli): 45 ($P_v CO_2$) - 40 ($P_A CO_2$) $\approx$ 5 mmHg.
⭐ $CO_2$ is ~20x more soluble than $O_2$, enabling rapid exchange despite a smaller pressure gradient.
- Alveolar Gas Eq: $P_A O_2 = (P_B - P_{H_2O}) \times F_i O_2 - \frac{P_a CO_2}{R}$ ($R \approx 0.8$). 
Ventilation-Perfusion (V/Q) Ratio - Lung's Perfect Match
- Ratio of alveolar ventilation ($V_A$) to pulmonary blood flow ($\dot{Q}$). Crucial for efficient gas exchange.
- Overall normal V/Q ≈ 0.8 ($V_A$ ≈ 4L/min, $\dot{Q}$ ≈ 5L/min).
- Regional Lung Variation (Upright):
- Apex: ↑V/Q (e.g., >3.0), relative dead space.
- Base: ↓V/Q (e.g., <0.6), relative shunt.
- Gravity affects $\dot{Q}$ more than $V_A$.
- V/Q Mismatch:
- V/Q = 0 (Shunt): No ventilation (e.g., atelectasis). 📌 "Sunk" = no air.
- V/Q = ∞ (Dead Space): No perfusion (e.g., PE). 📌 "PEA" = PE Alveolar dead space.
⭐ HPV: Key autoregulation. Diverts blood from hypoxic to well-ventilated areas, optimizing V/Q_matching and systemic oxygenation.
Diffusion Capacity (DLCO) - Exchange Efficiency Test
- Measures transfer of CO from alveoli to blood; assesses gas exchange efficiency.
- Depends on: membrane integrity, surface area, Hb, capillary volume.
- Normal: ~25 ml/min/mmHg.
- Formula: $DLCO = V_{CO} / P_{A_{CO}}$
- ↓ DLCO:
- Interstitial Lung Disease (ILD) (fibrosis), emphysema (↓SA)
- Anemia, pulmonary embolism
- ↑ DLCO:
- Polycythemia, pulmonary hemorrhage
- Exercise, L-R shunts
⭐ DLCO is significantly reduced in emphysema due to alveolar destruction, distinguishing it from chronic bronchitis where DLCO is often normal.
High‑Yield Points - ⚡ Biggest Takeaways
- Gas exchange relies on simple diffusion driven by partial pressure gradients across the thin alveolar-capillary membrane.
- Oxygen binds hemoglobin; CO₂ is primarily transported as bicarbonate (HCO₃⁻).
- Fick's Law: Diffusion rate ∝ (Area × ΔP) / Thickness.
- Ideal Ventilation/Perfusion (V/Q) ratio is ~0.8; mismatch leads to hypoxemia.
- DLCO (Diffusing capacity of the lungs for carbon monoxide) measures gas transfer; reduced in emphysema and pulmonary fibrosis.
- O₂-Hb dissociation curve: Right shift (↓O₂ affinity, ↑O₂ release) by ↑PCO₂, ↑H⁺ (↓pH), ↑Temperature, ↑2,3-DPG.
- Pulmonary shunt (V/Q = 0) and dead space (V/Q = ∞) represent extreme V/Q mismatches impairing gas exchange.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more