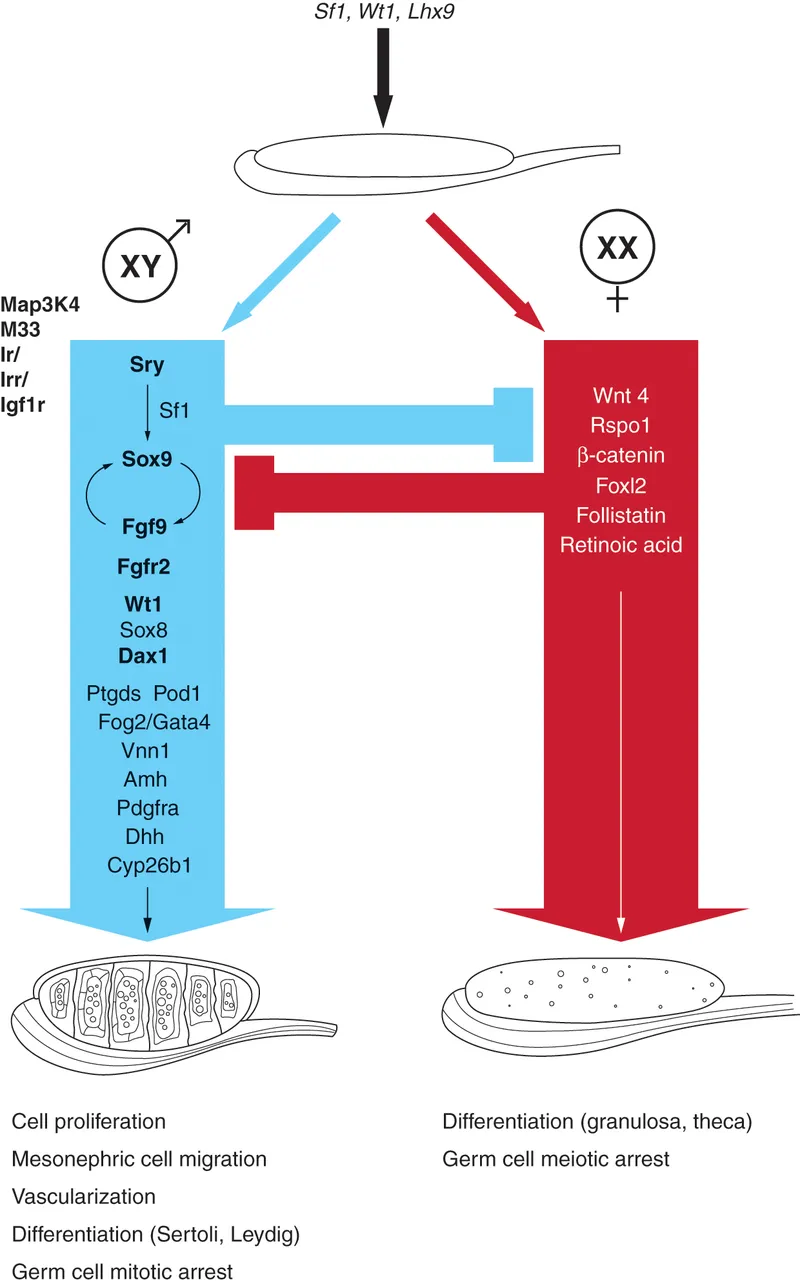
Chromosomal & Gonadal Sex - Blueprint Basics
- Chromosomal Sex: XX (female) or XY (male), set at fertilization.
- Gonadal Sex: Bipotential gonads differentiate into testes or ovaries.
- Indifferent until ~6th-7th week gestation.
- Testicular Pathway (XY):
- SRY gene (Y chromosome, short arm Yp) is key.
- SRY protein = Testis-Determinating Factor (TDF).
- TDF initiates testis formation.
- Ovarian Pathway (XX):
- Default pathway if no SRY/TDF.
- WNT4, RSPO1 essential for ovaries.
⭐ SRY gene on Y chromosome is the primary determinant of testicular differentiation.
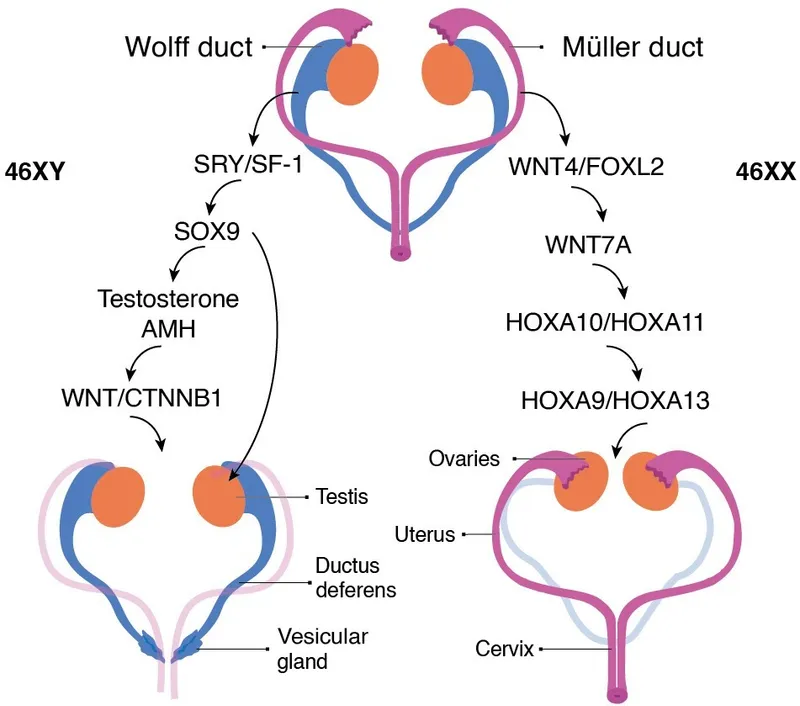
Internal Genital Ducts - Plumbing Plans
- Indifferent Stage: Both Wolffian (mesonephric) & Müllerian (paramesonephric) ducts initially present in both sexes.
- Male (XY):
- Sertoli cells: Secrete Anti-Müllerian Hormone (AMH) → Müllerian duct regression.
- Leydig cells: Produce Testosterone → Wolffian ducts develop into epididymis, vas deferens, seminal vesicles, ejaculatory ducts.
- Female (XX):
- No AMH: Müllerian ducts develop into fallopian tubes, uterus, upper 1/3 of vagina.
- No Testosterone: Wolffian ducts regress.
⭐ Anti-Müllerian Hormone (AMH), produced by Sertoli cells, is crucial for the regression of Müllerian ducts in males.
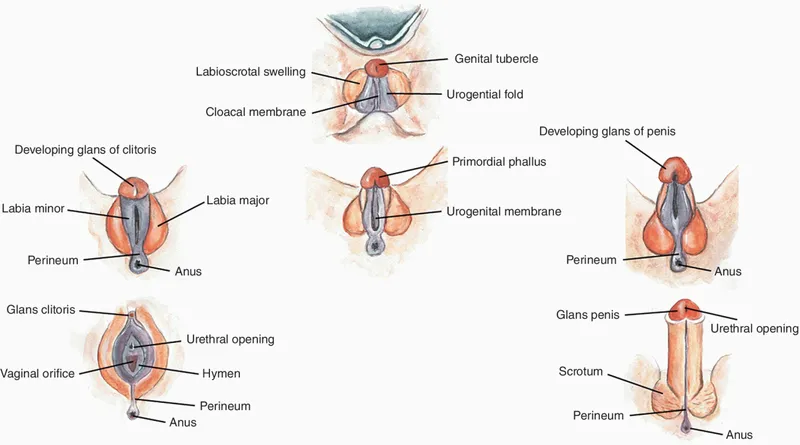
External Genitalia - Outside Story
- Indifferent Stage (<7 weeks):
- Genital tubercle → Glans
- Urogenital folds → Shaft/Labia minora
- Labioscrotal swellings → Scrotum/Labia majora
- Male (DHT-driven):
- Testosterone → DHT (via 5α-reductase).
⭐ Dihydrotestosterone (DHT), converted from testosterone by 5α-reductase, is essential for the development of male external genitalia.
- Tubercle → Penis.
- Folds fuse → Urethra.
- Swellings fuse → Scrotum.
- Female (No DHT):
- Tubercle → Clitoris.
- Folds (unfused) → Labia minora.
- Swellings (unfused) → Labia majora.
 oka
oka
Puberty & Maturation - The Big Reveal
⭐ The first sign of puberty is typically testicular enlargement in boys and thelarche (breast development) in girls.
- Initiated by pulsatile Gonadotropin-Releasing Hormone (GnRH) release from hypothalamus, stimulating pituitary Luteinizing Hormone (LH) & Follicle-Stimulating Hormone (FSH).
- LH/FSH drive gonads: ↑estrogen (girls), ↑testosterone (boys).
- Sequence (Girls): Thelarche (breast buds, ~10-11 yrs), pubarche, menarche.
- Sequence (Boys): Testicular enlargement (>4ml or >2.5cm, ~11-12 yrs), pubarche, voice deepening, spermarche.
- Adrenarche: Adrenal androgens (DHEA/S) contribute to pubic/axillary hair.
- Leads to secondary sexual characteristics (SSCs), growth spurt, and reproductive capability.
- Monitored using Tanner Stages.
Common DSDs - Clinical Correlations
- 46,XX DSDs:
- Congenital Adrenal Hyperplasia (CAH): Ambiguous genitalia, salt wasting (some). Key: 21-hydroxylase deficiency.
- Maternal androgen excess: Fetal virilization.
- 46,XY DSDs:
- Androgen Insensitivity Syndrome (AIS): Female external genitalia, absent uterus, testes present.
- 5α-reductase deficiency: Ambiguous at birth, virilizes at puberty.
- Gonadal Dysgenesis (Swyer): 46,XY, female phenotype, streak gonads.
- Ovotesticular DSD: Both ovarian & testicular tissue; variable phenotype.
⭐ Congenital Adrenal Hyperplasia (CAH), most commonly due to 21-hydroxylase deficiency, is a frequent cause of ambiguous genitalia in 46,XX infants.
High‑Yield Points - ⚡ Biggest Takeaways
- SRY gene on Y chromosome dictates testis development.
- Testes produce AMH (regresses Müllerian ducts) and testosterone (develops Wolffian ducts).
- Sertoli cells secrete AMH; Leydig cells secrete testosterone.
- DHT, from testosterone via 5α-reductase, virilizes external genitalia.
- Absence of SRY leads to ovarian development and female internal/external genitalia.
- Androgen Insensitivity Syndrome (AIS): XY, female phenotype, testes, ↑testosterone, absent uterus_
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more