Initiation of Labor - Go Time Signals
- Mechanical Factors: Uterine overdistension → ↑contractility.
- Fetal Endocrine Signals:
- Fetal Hypothalamic-Pituitary-Adrenal (HPA) axis maturation: ↑Fetal cortisol → ↑placental Corticotropin-Releasing Hormone (CRH).
- Placental CRH: Positive feedback, ↑Dehydroepiandrosterone Sulfate (DHEAS) → ↑estrogens.
- Hormonal Shift: ↑Estrogen / ↓Progesterone Ratio
- Estrogen: ↑Gap junctions (connexin-43), ↑oxytocin receptors, ↑prostaglandin (PG) synthesis.
- Progesterone: Functional withdrawal (altered receptor activity, not just ↓levels).
- Prostaglandins (PGE₂, PGF₂α):
- Key for cervical ripening (PGE₂) & myometrial contractions (PGF₂α, PGE₂).
- Synthesized in amnion, chorion, decidua.
- Oxytocin:
- ↑Myometrial contractility (via IP₃/DAG pathway).
- Ferguson Reflex: Cervical stretch → ↑oxytocin release (positive feedback).
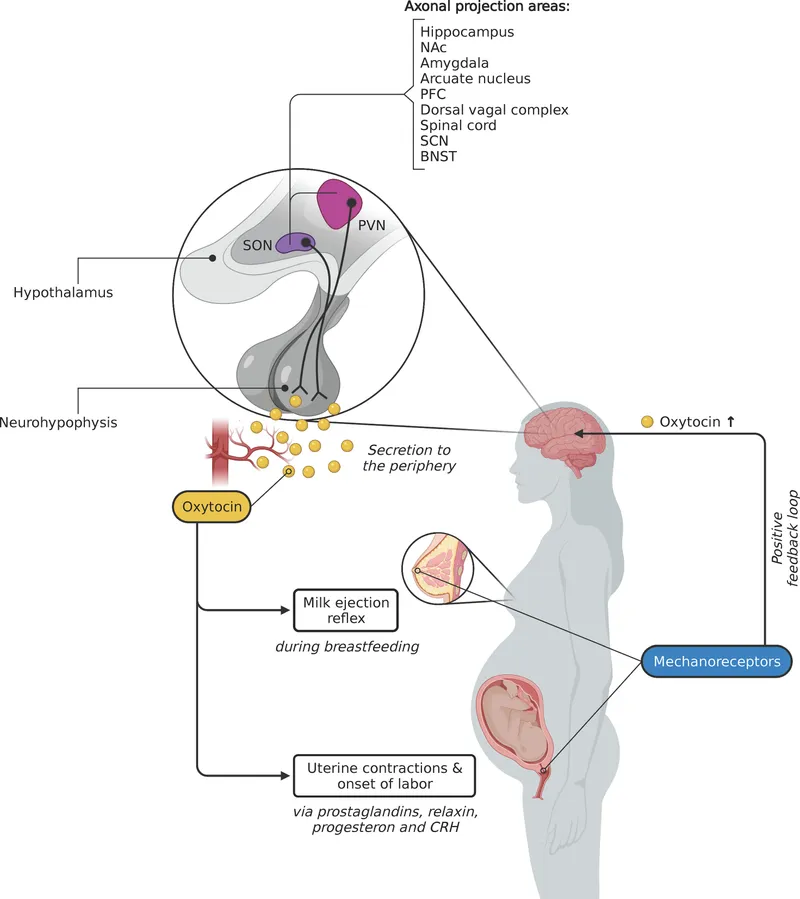
⭐ Placental CRH acts as a "placental clock"; its levels rise exponentially in the third trimester, influencing the timing of parturition and fetal lung maturation.
Stages of Labor - The Parturition Path
- Stage 1: Cervical Dilation (True labor pains → Full dilation 10 cm)
- Latent Phase: 0-4 cm (Primigravida: ~8h, Multigravida: ~5h)
- Active Phase: 4-10 cm (Dilation: P: ~1.2 cm/hr, M: ~1.5 cm/hr)
- Stage 2: Fetal Expulsion (Full dilation → Fetal delivery)
- Duration: P: ~2h (epidural ~3h); M: ~1h (epidural ~2h)
⭐ Crowning: Biparietal diameter distends vulva; no recession.
- Stage 3: Placental Expulsion (Fetal delivery → Placental delivery)
- Duration: 5-15 min (>30 min abnormal)
- Signs: Blood gush, cord lengthens, uterus firms & rises.
- Stage 4: Observation (1-4h postpartum)
- Monitor: Uterine tone, bleeding (PPH).
Mechanism of Labor - Baby's Exit Route
Sequential fetal movements for birth canal passage:
- Engagement: Fetal head's biparietal diameter passes pelvic inlet.
- Descent: Continuous downward movement throughout labor.
- Flexion: Fetal chin tucks to chest, presenting smaller diameter (suboccipitobregmatic).
- Internal Rotation: Occiput rotates anteriorly towards pubic symphysis.
- Extension: Head extends as occiput passes under pubic symphysis; crowning.
- Restitution: Head externally rotates to align with shoulders.
- External Rotation: Shoulders rotate into antero-posterior pelvic diameter.
- Expulsion: Anterior shoulder, then posterior shoulder, then body deliver.
📌 Mnemonic: Every Darn Fool In Rotterdam Eats Rotten Eggs (for the cardinal movements)
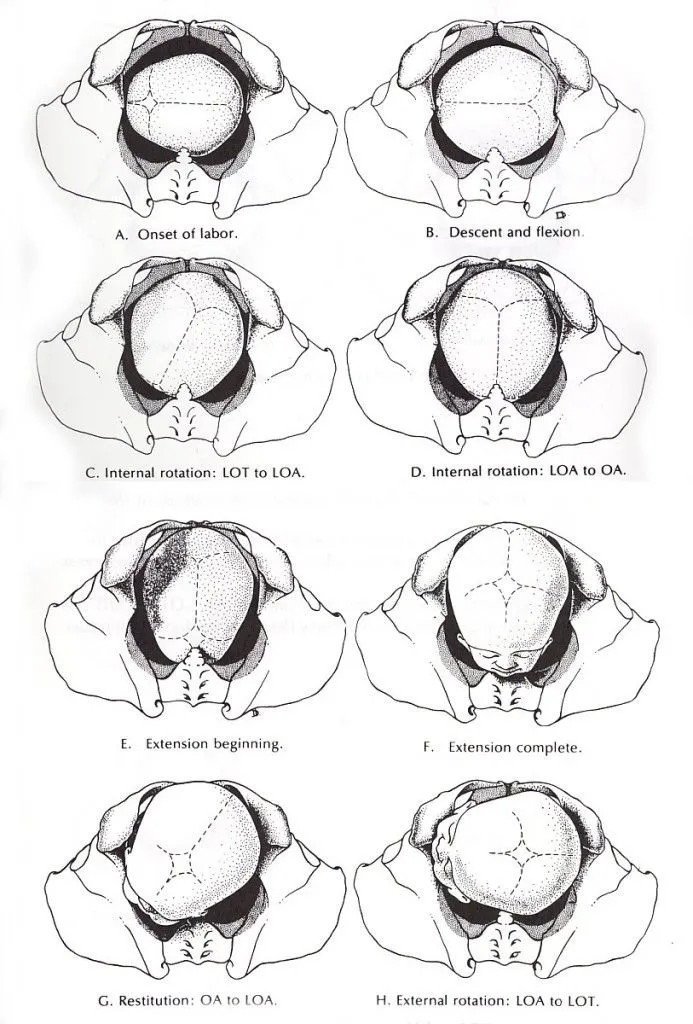
⭐ The Left Occipito-Anterior (LOA) is the most common and favorable fetal position.
Maternal Physiology & Pain Relief - Mom's Labor Load
- Maternal Physiology:
- CV: ↑CO (~50% 2nd stage), ↑BP. Risk: Supine hypotension.
- Resp: Hyperventilation → resp. alkalosis. ↑O₂ consumption.
- Haem: Physiologic leukocytosis (WBC up to 25k-30k/mm³).
- GI: ↓Gastric emptying (aspiration risk).
- Labor Pain Pathways:
- 1st Stage: T10-L1 (visceral - uterine/cervical).
- 2nd Stage: S2-S4 (somatic - perineal).
- Pain Relief in Labor:
- Non-Pharmacological: Lamaze, TENS, hydrotherapy, breathing.
- Pharmacological (Systemic):
- Inhalational: Entonox (50% N₂O + 50% O₂).
- Opioids: Pethidine, Fentanyl (⚠️ neonatal resp. depression).
- Regional Analgesia (Most Effective):
- Epidural: Bupivacaine + Fentanyl. S/E: hypotension, ↑2nd stage, headache.
- Spinal: C-section, rapid analgesia.
- Pudendal block: Perineal pain, episiotomy.
⭐ Epidural analgesia, while highly effective, is associated with an increased risk of instrumental delivery and a longer second stage of labor.
High‑Yield Points - ⚡ Biggest Takeaways
- Ferguson reflex: cervical stretch → oxytocin release (posterior pituitary).
- Oxytocin & Prostaglandins (PGF2α, PGE2): drive uterine contractions; prostaglandins also ensure cervical ripening.
- ↑ Estrogen/Progesterone ratio: sensitizes uterus to oxytocin.
- Stages of Labor: 1st (cervical dilation), 2nd (fetal expulsion), 3rd (placental delivery).
- Relaxin: aids cervical softening & pelvic ligament relaxation.
- Lightening: fetal head descent into pelvis, often pre-labor.
- CRH (Corticotropin-Releasing Hormone) from placenta also plays a role in timing parturition by increasing fetal cortisol which promotes surfactant production and lung maturity impacting prostaglandin synthesis indirectly.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

