Follicular Development & LH Surge - Eggcellent Race
- Follicular Growth (FSH-driven): Primordial → Primary → Secondary (antral) → Graafian (dominant).
- Granulosa cells: Convert androgens to estrogen (aromatase).
- Theca cells: Produce androgens (LH-dependent).
- LH Surge: Triggered by sustained ↑ estrogen (positive feedback from dominant follicle).
- Key Actions of LH Surge:
- Oocyte completes Meiosis I (becomes secondary oocyte).
- Triggers ovulation (follicle rupture).
- Luteinization of follicular cells → Corpus Luteum.
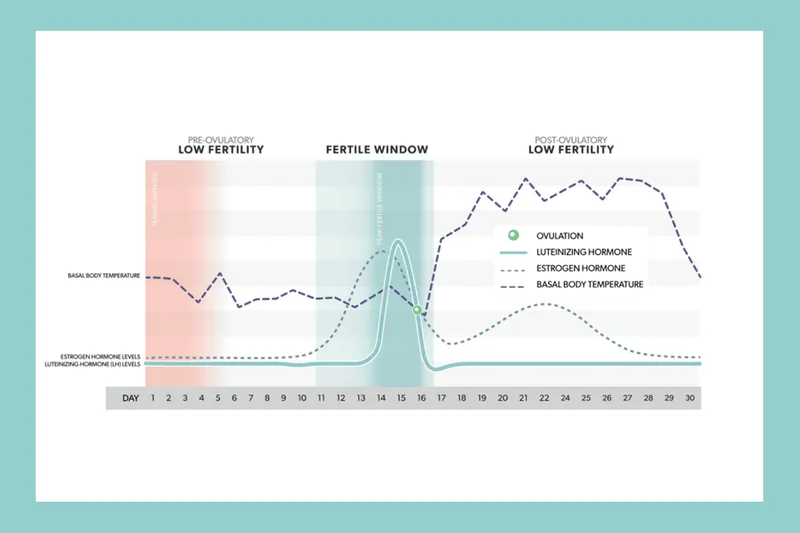
⭐ The LH surge, crucial for ovulation, typically begins 24-36 hours before oocyte release, with the oocyte being extruded approximately 10-12 hours after the LH peak.
Ovulation & Corpus Luteum - Pop & Progesterone
- Ovulation:
- Trigger: LH surge (~10-12 hrs post-peak).
- Mechanism: ↑ Proteolytic enzymes (e.g., collagenase) → follicular rupture.
- Oocyte released: Secondary oocyte (metaphase II).
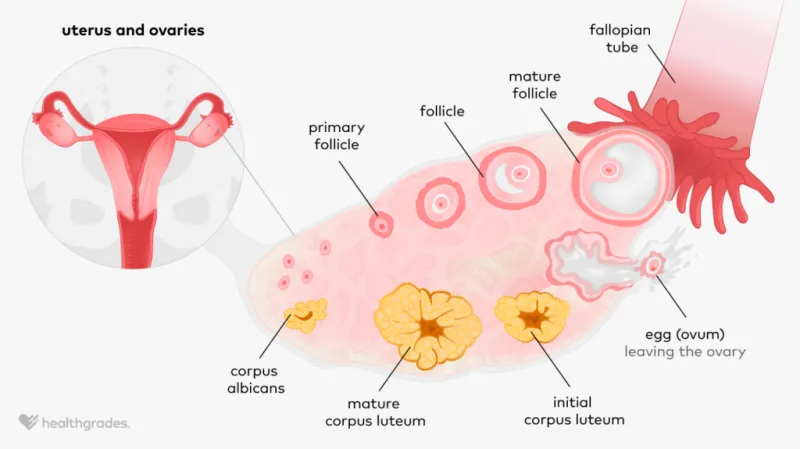
- Corpus Luteum (CL):
- Formed from follicle remnants (granulosa & theca cells).
- Secretes: Progesterone (dominant), estrogen, inhibin A.
- Lifespan: ~14 days (no fertilization) → corpus albicans.
- Pregnancy: Rescued by hCG; persists ~12 weeks.
- Progesterone Actions:
- Endometrium: Secretory changes for implantation.
- Myometrium: ↓ contractility.
- Cervical mucus: Thick, scanty.
- Thermogenic: ↑ basal body temp (~0.5°C).
- Inhibits GnRH, LH, FSH. 📌 Progesterone Promotes Pregnancy.
⭐ The corpus luteum, formed post-ovulation, secretes progesterone which is vital for endometrial preparation and maintenance of early pregnancy; its lifespan is ~14 days without hCG stimulation.
Sperm Capacitation & Acrosome Rxn - Swimmers' Gauntlet
-
Sperm Capacitation: Final maturation in female reproductive tract (~5-7 hrs).
- Key changes:
- Removal of cholesterol & glycoproteins from sperm head.
- ↑ Membrane fluidity & Ca²⁺ influx.
- Hyperactivated motility (whiplash tail movements).
- Prepares sperm for acrosome reaction & fertilization.
- Key changes:
-
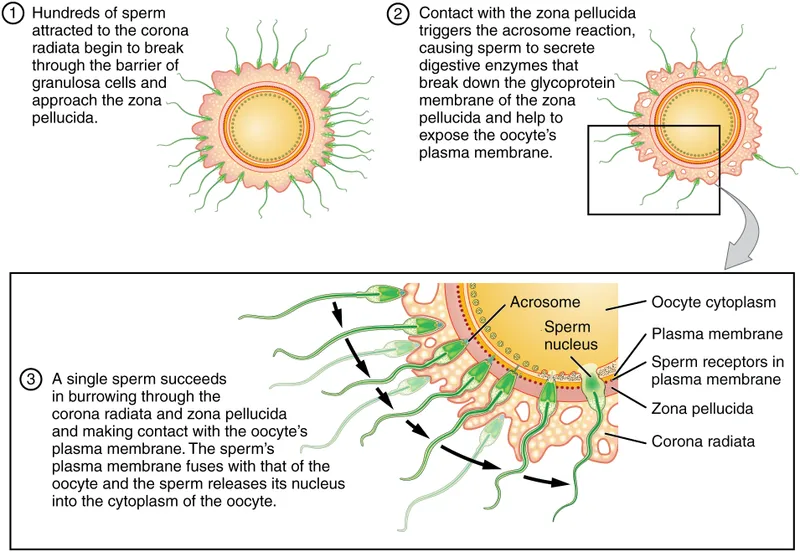
Acrosome Reaction: Triggered by sperm binding to Zona Pellucida (ZP3 glycoprotein).
- Process:
- Fusion of sperm's plasma membrane with outer acrosomal membrane.
- Release of acrosomal enzymes: Hyaluronidase (digests corona radiata), Acrosin (digests zona pellucida).
- Enables sperm to penetrate zona pellucida.
- Process:
⭐ Sperm capacitation, occurring in the female reproductive tract, involves removal of cholesterol and glycoproteins from the sperm head, leading to hyperactivated motility and enabling the acrosome reaction.

Fertilization & Polyspermy Block - Zygote Genesis
- Fertilization Steps:
- Sperm: Capacitation & acrosome reaction enable penetration.
- Pathway: Corona radiata → Zona Pellucida (ZP3 binding) → oocyte membrane fusion.
- Polyspermy Block: Critical to prevent aneuploidy.
- Fast Block: Oocyte membrane depolarization (transient).
- Slow Block (Zona Reaction): Cortical granule release → ZP hardening.
⭐ The cortical reaction, triggered by sperm-oocyte fusion, results in the release of cortical granules, causing the zona pellucida to harden (zona reaction), thus providing the primary block to polyspermy.
- Zygote Genesis:
- Oocyte: Completes Meiosis II post-sperm entry.
- Pronuclei: Male & female pronuclei form.
- Syngamy: Fusion of pronuclei → diploid zygote.
High‑Yield Points - ⚡ Biggest Takeaways
- LH surge is the primary trigger for ovulation.
- Ovulation occurs ~10-12 hours after LH peak or 24-36 hours after LH surge onset.
- Corpus luteum secretes progesterone, vital for endometrial support.
- Fertilization most commonly occurs in the ampulla of the fallopian tube.
- Capacitation and acrosome reaction are essential for sperm to fertilize the oocyte.
- Oocyte completes Meiosis II only after sperm penetration.
- Zona reaction and cortical reaction block polyspermy.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

