Spermatogenesis - Sperm Boot Camp
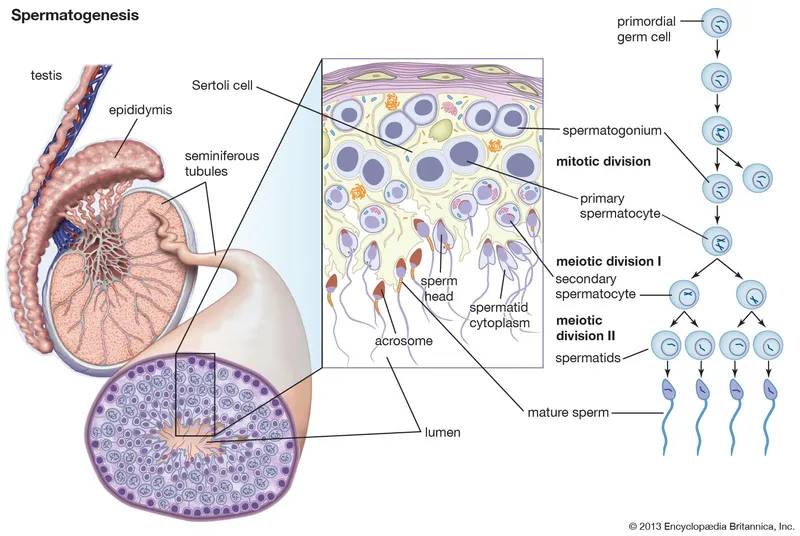
- Process: Formation of spermatozoa from spermatogonial stem cells in seminiferous tubules.
- Duration: ~74 days. Temp: 2-3°C < core body temp.
- Key Cells & Hormones:
- Sertoli cells: Support spermatogenesis (FSH, Testosterone), blood-testis barrier.
- Leydig cells: Produce Testosterone (LH); crucial for spermatogenesis.
- Phases:
- Spermatocytogenesis (Mitosis): Spermatogonia (2n) → Primary spermatocytes (2n).
- Meiosis:
- Meiosis I: Primary spermatocyte (2n) → 2 Secondary spermatocytes (n).
- Meiosis II: Secondary spermatocyte (n) → 2 Spermatids (n).
- Spermiogenesis: Spermatids (n) → Spermatozoa (n) (morphological change).
- Acrosome/flagellum formation, nuclear condensation, cytoplasm shed. No division.
⭐ One full cycle of spermatogenesis, from spermatogonium to mature spermatozoa, takes approximately 74 days in humans.
Hormonal Regulation - Testosterone Tune-Up
- HPG Axis: Central control.
- Hypothalamus: Pulsatile Gonadotropin-Releasing Hormone (GnRH).
- Anterior Pituitary:
- Luteinizing Hormone (LH) → Leydig cells → Testosterone (T) synthesis.
- T: Drives spermatogenesis, 2° sex characteristics, libido, anabolic effects.
- Negative feedback: ↓GnRH pulses (Hypo), ↓LH sensitivity (Ant. Pit.).
- Follicle-Stimulating Hormone (FSH) → Sertoli cells.
- Sertoli cells: Produce ABP (concentrates T), Inhibin B (↓FSH), Aromatase ($T \rightarrow E_2$).
- Luteinizing Hormone (LH) → Leydig cells → Testosterone (T) synthesis.
- Testosterone (T):
- Circulation: ~2% free (active), ~65% SHBG-bound, ~33% albumin-bound.
- Peripheral Conversion:
- To Dihydrotestosterone (DHT) via 5α-reductase: Potent; for external genitalia, prostate, hair.
- To Estradiol ($E_2$) via aromatase: Bone maturation, feedback.
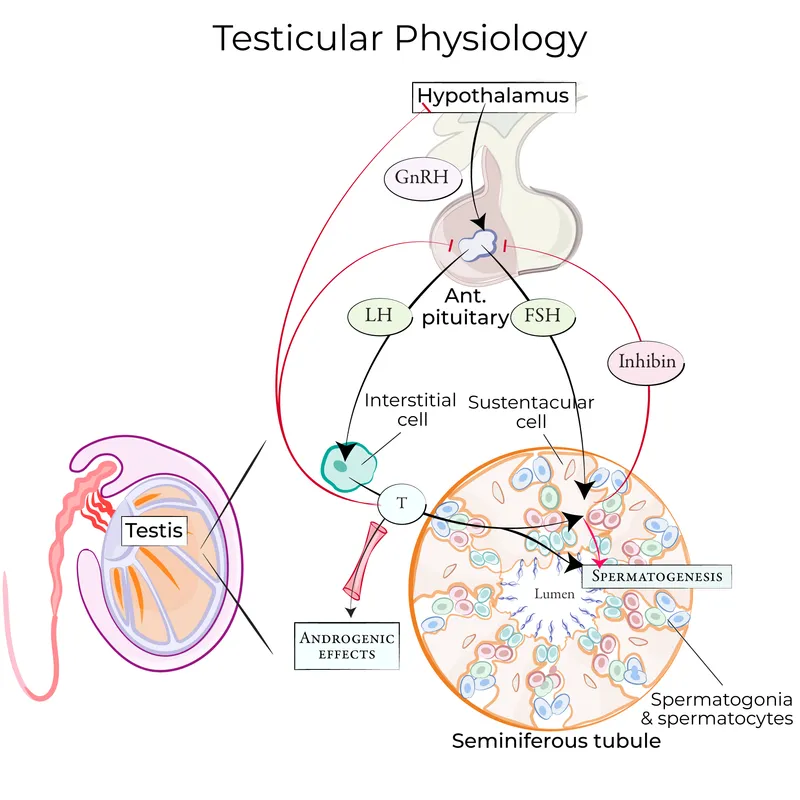
⭐ Pulsatile GnRH secretion is crucial; continuous GnRH (e.g., leuprolide) causes receptor downregulation, leading to medical castration.
Semen & Fertilization - The Vital Fluid
Semen: Key Parameters & Sources
- Vol: 2-5 mL; pH: 7.2-7.8 (alkaline)
- Sperm: >16 M/mL; Motility >40% progressive; Morphology >4% normal (WHO 2021)
- Sources:
- Seminal Vesicles (~65%): Fructose (energy), prostaglandins, coagulants
- Prostate (~25%): PSA (liquefaction), citrate, zinc, acid phosphatase
- Bulbourethral Glands (<5%): Alkaline mucus (neutralizes acidity, lubrication)
Fertilization Steps
- Capacitation: Sperm activation in female tract (cholesterol loss, $↑Ca^{2+}$ influx).
- Acrosome Rxn: Enzymes (hyaluronidase, acrosin) released to digest Zona Pellucida (ZP).
- Cortical Rxn: Oocyte releases granules; ZP hardens (prevents polyspermy).
- Syngamy: Fusion of male & female pronuclei → Zygote.
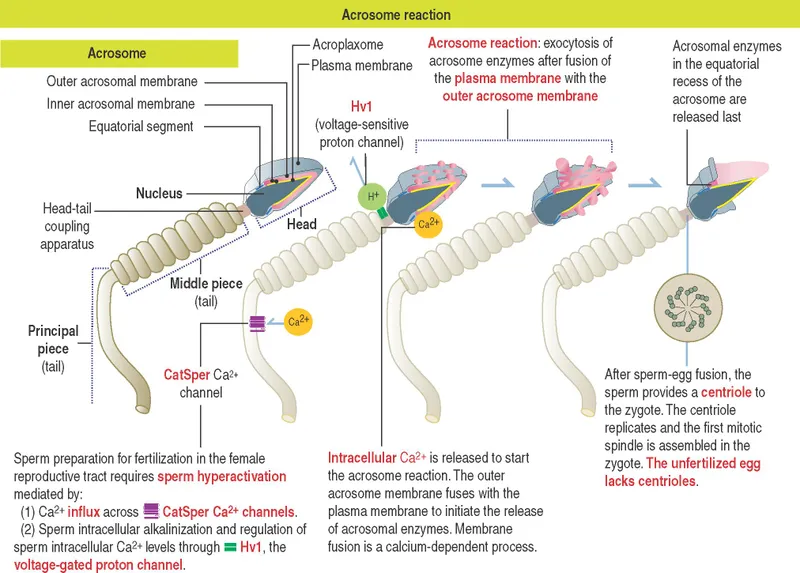
⭐ Capacitation in the female tract is vital for sperm to fertilize; involves cholesterol removal from the sperm membrane and changes in surface glycoproteins, unmasking binding sites.
Male Sexual Act - The Climax Cascade
- Sequence: Erection → Emission → Ejaculation → Resolution.
- Erection (Parasympathetic: S2-S4, Pelvic n.):
- NO release → ↑cGMP → vasodilation (corpora cavernosa/spongiosum).
- PDE-5 inhibitors (Sildenafil) maintain erection by ↓cGMP breakdown.
- Emission (Sympathetic: T10-L2, Hypogastric n.):
- Smooth muscle contraction (vas deferens, seminal vesicles, prostate) → semen to prostatic urethra.
- Ejaculation (Sympathetic & Somatic: Pudendal n.):
- Rhythmic muscle contractions (bulbospongiosus, ischiocavernosus) → semen expulsion.
- Bladder neck (internal sphincter) closes (sympathetic) preventing retrograde flow.
- Resolution (Sympathetic): Vasoconstriction → detumescence.
⭐ Emission is the "point of no return"; ejaculation typically follows.
High‑Yield Points - ⚡ Biggest Takeaways
- Spermatogenesis occurs in seminiferous tubules; requires temperature 2-3°C below body.
- Sertoli cells support sperm, form blood-testis barrier, secrete Inhibin B (↓FSH).
- Leydig cells (interstitial), via LH, produce Testosterone.
- Testosterone drives male secondary sexual characteristics, libido, and anabolism.
- FSH → Sertoli cells (spermatogenesis); LH → Leydig cells (testosterone).
- Erection: Parasympathetic (NO); Emission/Ejaculation: Sympathetic.
- Sperm capacitation (female tract) & acrosome reaction vital for fertilization.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

