Female Reproductive Physiology - Eggcellent Adventures
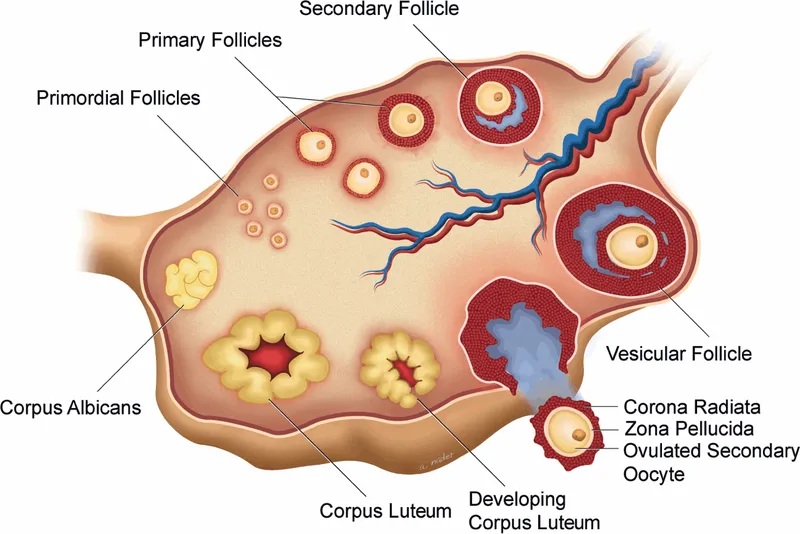
- Folliculogenesis: Maturation journey from primordial follicle → primary → secondary → mature Graafian follicle (~20mm).
- Two-Cell, Two-Gonadotropin Theory:
- Theca cells (LH stimulation): Synthesize androgens.
- Granulosa cells (FSH stimulation): Convert androgens to estrogen via aromatase.
- Ovulation: LH surge (peaks 24-36h before) triggers release of oocyte.
⭐ The LH surge, triggered by sustained high estrogen levels (positive feedback), is essential for ovulation.
- Luteal Phase:
- Corpus Luteum: Forms post-ovulation; secretes progesterone (maintains endometrium).
- Corpus Albicans: Scar tissue if no pregnancy.
Female Reproductive Physiology - Monthly Makeover
Uterine cycle (21-35 days); menses 2-7 days. 📌 M-PES (Menstrual, Proliferative-Estrogen, Secretory-Progesterone).
- Menstrual Phase (Days 1-5):
- ↓Progesterone → spiral artery spasm, endometrial shedding.
- Proliferative Phase (Days 6-14, variable):
- Estrogen-driven: endometrial growth, glands & spiral arteries elongate.
- Secretory Phase (Days 15-28, fixed ~14 days):
- Progesterone-dominant: glandular tortuosity & secretion (glycogen, mucus), spiral arteries coil. Decidualization for implantation.
- No implantation: ↓progesterone → menstruation.
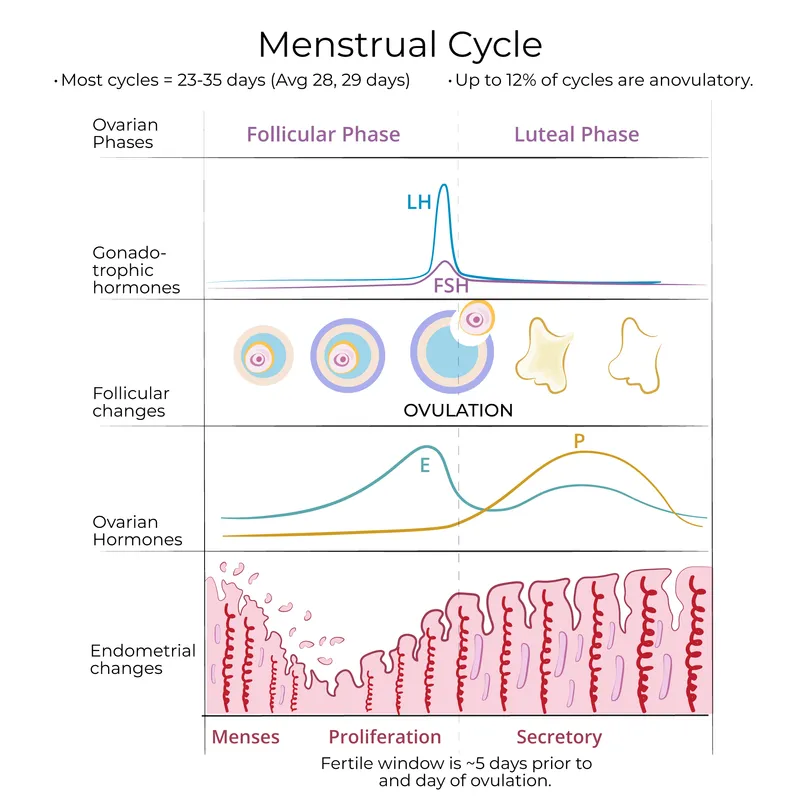
⭐ The secretory phase endometrium, rich in glycogen and mucus, is prepared by progesterone for potential implantation.
Female Reproductive Physiology - Hormone Harmony
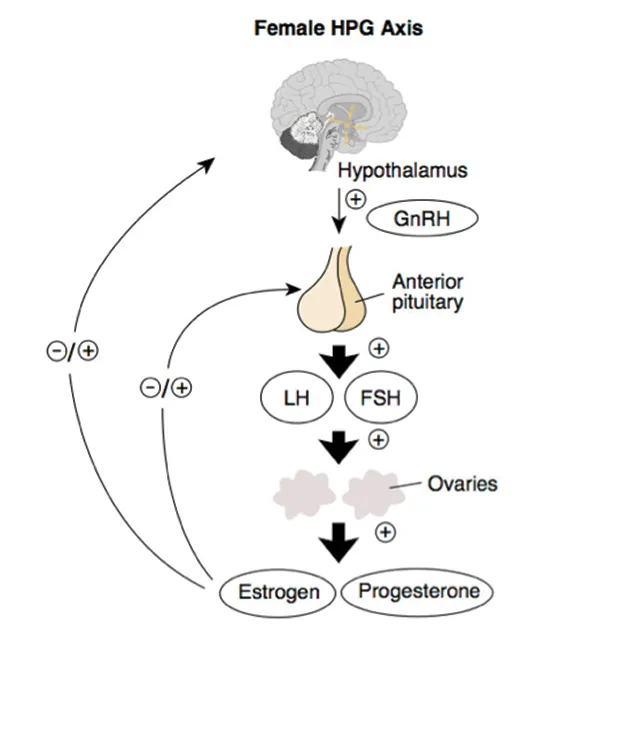
- Hypothalamus: Secretes GnRH (pulsatile) → stimulates Ant. Pituitary.
- Ant. Pituitary: Releases FSH (follicle growth) & LH (ovulation/corpus luteum) → act on Ovary.
- Ovary Hormones & Feedback Loops:
- Estrogen:
- Low/Moderate levels: Negative feedback on FSH/LH (↓).
- Sustained High (pre-ovulatory): Positive feedback → LH surge (↑).
- Progesterone: Strong negative feedback on GnRH/LH/FSH (↓).
- Inhibin B (granulosa cells): Negative feedback, selectively ↓FSH.
- Activin (granulosa cells): Positive feedback, stimulates ↑FSH.
- Estrogen:
⭐ Inhibin B, produced by granulosa cells under FSH stimulation, selectively inhibits FSH secretion from the anterior pituitary.
Female Reproductive Physiology - Conception & Kick-off
- Gamete Transport & Fertilization:
- Sperm: Capacitation & acrosome reaction.
- Ovum: Picked up by fimbriae.
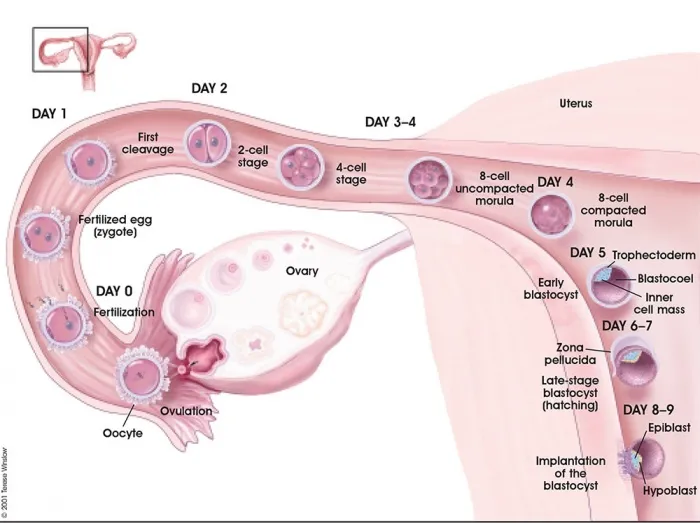
- Fertilization site: Ampulla of fallopian tube.
⭐ Fertilization typically occurs in the ampulla of the fallopian tube, the widest part of the tube.
- Early Development: Zygote → Morula → Blastocyst (Inner cell mass & Trophoblast).
- Implantation (Day 6-10 post-ovulation): Apposition, Adhesion, Invasion.
- Trophoblast differentiates: Syncytiotrophoblast (produces hCG) & Cytotrophoblast.
- hCG (Human Chorionic Gonadotropin):
- Rescues corpus luteum; basis of pregnancy tests.
- Detectable in serum: 8-11 days post-conception.
- Doubles every 48-72 hours in early viable intrauterine pregnancy.
Female Reproductive Physiology - The Grand Pause
- Menopause: 12 months amenorrhea post-FMP. Avg. age ~51 (45-55 yrs). Perimenopause is transition.
- Cause: Ovarian follicle depletion → ↓Estrogen, ↓Inhibin → ↑FSH (diagnostic, >30-40 mIU/mL), ↑LH.
- Features: Vasomotor (hot flashes), urogenital atrophy, mood/sleep issues, osteoporosis risk.
⭐ Markedly elevated serum FSH levels (e.g., > 30-40 mIU/mL) are a hallmark of menopause due to loss of negative feedback from ovarian estrogen and inhibin.
High‑Yield Points - ⚡ Biggest Takeaways
- Menstrual cycle is orchestrated by GnRH, FSH, LH, estrogen, and progesterone.
- Ovulation is triggered by an LH surge, typically around day 14.
- Corpus luteum produces progesterone to maintain the endometrium.
- Fertilization usually occurs in the ampulla of the fallopian tube.
- hCG (human chorionic gonadotropin) maintains the corpus luteum in early pregnancy.
- Estrogen is responsible for secondary sexual characteristics and endometrial proliferation.
- Progesterone is the "pregnancy hormone," promoting endometrial secretion and uterine quiescence.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

